Orientation and Mobility Specialist Manual
Printing the manual material found at this website for long-term use is not advisable. Department Policy material is updated periodically and it is the responsibility of the users to check and make sure that the policy they are researching or applying has the correct effective date for their circumstances.
If you experience any difficulty opening a section or link from this page, please email the webmaster.
How to Search this manual:
This edition has three search options.
- Search the whole manual. Open the Complete Manual pane. From your keyboard press the Ctrl and F keys at the same time. A search box will appear. Type in a descriptive or key word (for example "Denials". The search box will show all locations where denials discussed in the manual.
- Search by Chapter. Open any Chapter tab (for example the "Billing Procedures" tab). From your keyboard press the Ctrl and F keys at the same time. A search box will appear. Type in a descriptive or key word (for example "Denials". The search box will show where denials discussed in just that chapter.
- Site Search. Search the manual as well as other documents related to a particular search term on the Montana Healthcare Programs Site Specific Search page.
Prior manuals may be located through the provider website archives.
Updated 04/14/2022
Orientation and Mobility Specialist Services Manual
To print this manual, right click your mouse and choose "print". Printing the manual material found at this website for long-term use is not advisable. Department Policy material is updated periodically and it is the responsibility of the users to check and make sure that the policy they are researching or applying has the correct effective date for their circumstances.
Update Log
Orientation and Mobility Specialist Services Manual
To print this manual, right click your mouse and choose "print". Printing the manual material found at this website for long-term use is not advisable. Department Policy material is updated periodically and it is the responsibility of the users to check and make sure that the policy they are researching or applying has the correct effective date for their circumstances.
Publication History
This publication supersedes all previous Orientation and Mobility Specialist Services handbooks. Published by the Montana Department of Public Health & Human Services, January 2005.
Updated January 2011, December 2011, March 2012, October 2016, April 2017, June 2017, June 2018, January 2020, and April 2022.
CPT codes, descriptions and other data only are copyright 2014 American Medical Association (or such other date of publication of CPT). All Rights reserved. Applicable FARS/DFARS Apply.
Update Log
04/14/2022
- Removed Nurse First Advice Line references.
- Removed HIP references.
- Updated Index to Search Options.
01/01/2020
- Cost Share references removed from Billing Procedures, and Submitting A Claim Chapters.
- Term "Medicaid" replaced with "Montana Healthcare Programs" throughout the manual.
06/04/2018
Removed commercial resource references.
06/20/2017
Orientation and Mobility Specialist Services Manual converted to an HTML format and adapted to 508 Accessibility Standards.
End Update Log Chapter
Table of Contents
Key Contacts
Key Websites
Introduction
Manual Organization
Manual Maintenance
Rule References
Claims Review (MCA 53-6-111, ARM 37.85.406)
Getting Questions Answered
Othe Department Programs
Covered Services
General Coverage Principles
- Services within Scope of Practice (ARM 37.86.2235)
- Certification
- EPSDT (ARM 37.86.2201-2235)
Noncovered Services (ARM 37.85.207)
Coverage of Specific Services
Verifying Coverage
Passport and Prior Authorization
What Is Passport to Health? (ARM 37.85.5101-5120, ARM 37.86.5303 and 37.86.5201-5206)
- Passport to Health Primary Care Case Management (ARM 37.86.5101-5120)
- Team Care (ARM 37.86.5303)
Prior Authorization
Coordination of Benefits
When Members Have Other Coverage
Identifying Additional Coverage
When a Member Has Medicare
- Medicare Part B Crossover Claims
When a Member Has TPL (ARM 37.85.407)
- Exceptions to Billing Third Party First
- Requesting an Exemption
- When the Third Party Pays or Denies a Service
- When the Third Party Does Not Respond
Billing Procedures
Claim Forms
Timely Filing Limits (ARM 37.85.406)
- Tips to Avoid Timely Filing Denials
When to Bill Montana Healthcare Members (ARM 37.85.406)
Member Co-Payments (ARM 37.85.204)
When Members Have Other Insurance
Billing for Retroactively Eligible Members
Usual and Customary Charge (ARM 37.85.406)
Coding
Using the Montana Healthcare Programs Fee Schedule
Using Modifiers
Billing Tips for Specific Providers
- Orientation and Mobility Specialist Services
The Most Common Billing Errors and How to Avoid Them
Submitting a Claim
Electronic Claims
Billing Electronically with Paper Attachments
Paper Claims
CMS-1500 Agreement
Claim Inquiries
Avoiding Claim Errors
Remittance Advices and Adjustments
Electronic Remittance Advice
- Credit Balance Claims
Rebilling and Adjustments
- Timeframe for Rebilling or Adjusting a Claim
- Rebilling Montana Healthcare Programs
- How to Rebill
- Adjustments
- When to Request an Adjustment
- How to Request an Adjustment
- Completing an Adjustment Request Form
- Mass Adjustments
Payment and the RA
How Payment Is Calculated
Overview
How Payment is Calculated on TPL Claims
How Payment is Calculated on Medicare Crossover Claims
Other Factors That May Affect Payment
Appendix A: Forms
Individual Adjustment Request
Paperwork Attachment Cover Sheet
Definitions and Acronyms
Index
End of Table of Contents Chapter
Key Contacts
Hours for Key Contacts are 8:00 a.m. to 5:00 p.m. Monday through Friday (Mountain Time), unless otherwise stated. The phone numbers designated “In state” will not work outside Montana.
Direct Deposit Arrangements
Providers who need to enroll in electronic funds transfer (EFT) and register for electronic remittance advices (RAs) should contact Provider Relations for assistance. Providers should mail or fax their completed documentation to Provider Relations:
Provider Relations
P.O. Box 4936
Helena, MT
1 (800) 624-3958 or (406) 442-4402
(406) 442-4402 Fax
EDI Solutions Help Desk
For questions regarding electronic claims submission:
(800) 987-6719 In/Out of state
(406) 442-1837 Helena
(850) 385-1705 Fax
Send e-mail inquiries to:
Mail to:
EDI Solutions Montana
P.O. Box 4936
Helena, MT 59604
Member Eligibility
There are several methods for verifying member eligibility. The most commonly used methods are below. For additional methods and details on each, see the Member Eligibility and Responsibilities chapter in the General Information for Providers manual.
FaxBack: (800) 714-0075 (24 hours)
Voice Response System: (800) 362-8312 (24 hours)
Montana Access to Health Web Portal: https://mtaccesstohealth.portal.conduent.com/mt/general/home.d
Medifax EDI: (800) 444-4336 Ext. 2072 (24 hours)
Orientation and Mobility Specialist Services
(406) 444-4066 In/Out of state
(406) 444-1861 Fax
Send written inquiries to:
O&M Specialist Program Officer
DPHHS
P.O. Box 202951
Helena, MT 59620-2951
Paper Claims
Send paper claims to:
Claims Processing Unit
P.O. Box 8000
Helena, MT 59604
Parents Let’s Unite for Kids (PLUK)
PLUK
516 North 32nd Street
Billings, MT 59101-6003
(406) 255-0540 Phone
(800) 222-7585 Phone
(406) 255-0523 Fax
E-mail: info@pluk.org
Website: http://www. pluk.org/
Provider Relations
For questions about eligibility, payments, denials, or general claims questions, or questions about Montana Healthcare Programs or Passport provider enrollment, address or phone number changes:
(800) 624-3958 In/Out of state
(406) 442-1837 Helena
Send e-mail inquiries to: MTPRHelpdesk@conduent.com
Send written inquiries to:
Provider Enrollment Unit
P.O. Box 4936
Helena, MT 59604
Provider’s Policy Questions
For policy questions, contact the appropriate division of the Department of Public Health and Human Services; see the Introduction chapter in the General Information for Providers manual.
Secretary of State
The Secretary of State’s office publishes the most current version of the Administrative Rules of Montana (ARM).
(406) 444.2055 Phone
Send written inquiries to:
Secretary of State
P.O. Box 202801
Helena, MT 59620-2801
Team Care
For questions about the Team Care program:
(406) 444-4540 Phone
(406) 444-1861 Fax
Send written inquiries to:
Team Care Program Officer
Managed Care Bureau
DPHHS
P.O. Box 202951
Helena, MT 59620-2951
Third Party Liability
For questions about private insurance, Medicare or other third party liability:
(800) 624-3958 In/Out of state
(406) 442-1837 Helena
(406) 442-4402 Fax
Send written inquiries to:
Third Party Liability Unit
P.O. Box 5838
Helena, MT 59604
End of Key Contacts Chapter
Key Websites
EDI Gateway - https://edisolutionsmmis.portal.conduent.com/gcro/
Gateway is Montana’s HIPAA clearinghouse. Visit this website for more information on:
- EDI support
- Enrollment
- Manuals
- Provider services
- Software
Health Resources Division
- Big Sky Rx: Helps Medicare members pay for Medicare-approved prescription drug insurance premiums.
- Electronic Billing: How to submit Montana Healthcare Programs claims electronically.
- Healthy Montana Kids: Information on HMK. See website below.
- Montana Healthcare Programs member: Montana Healthcare Programs services for adults and children.
- Montana Healthcare Programs Provider Information: See Montana Access to Health (MATH) Web Portal and Provider Information Website below.
- Montana Healthcare Programs Fraud and Abuse Reporting: Provides telephone numbers to call if you have concerns about Montana Healthcare Programs fraud or abuse.
- Montana Healthcare Programs:
- Passport to Health: Information and enrollment forms for the Passport to Health primary care case management program.
- Prescription Assistance Programs: Summary of information on the programs designed to make prescription drugs more affordable.
- Team Care: Information and enrollment information for the Team Care program.
Provider Information Website
https://medicaidprovider.mt.gov/
- Fee schedules
- Forms
- Frequently asked questions (FAQs)
- HIPAA update
- Key contacts
- Links to other websites and more
- Montana Healthcare Programs news
- Newsletters
- Provider enrollment
- Provider manuals, notices and manual replacement pages
- Remittance advice notices
- Upcoming events
End of Key Websites Chapter
Introduction
Thank you for your willingness to serve members of the Montana Healthcare Programs and other medical assistance Programs administered by the Department of Public Health and Human Services.
Manual Organization
This manual provides information specifically for providers of orientation and mobility specialist services. Additional essential information for providers is contained in the separate General Information for Providers manual. Each provider is asked to review both manuals.
A table of contents and an index allow you to quickly find answers to most questions. The margins contain important notes with extra space for writing notes. Each manual contains a list of Key Contacts. We have also included a space on the back of the front cover to record your NPI/API for quick reference when calling Provider Relations.
Manual Maintenance
In order to remain accurate, manuals must be kept current. Changes to manuals are provided through notices and replacement pages, which are posted on the Provider Information website. (See Key Websites.) When replacing a page in a paper manual, file the old pages and notices in the back of the manual for use with claims that originated under the old policy.
Rule References
Providers must be familiar with all current rules and regulations governing the Montana Healthcare Programs. Provider manuals are to assist providers in billing Montana Healthcare programs; they do not contain all Montana Healthcare programs rules and regulations. Rule citations in the text are a reference tool; they are not a summary of the entire rule. In the event that a manual conflicts with a rule, the rule prevails. Links to rules are available on the Provider Information website (See Key Websites). Paper copies of rules are available through the Secretary of State’s office (See Key Contacts).
Providers are responsible for knowing and following current laws and regulations.
In addition to the Montana Healthcare programs rules outlined in the General Information for Providers manual, the following rules and regulations are also applicable to the orientation and mobility specialist Programs:
- Code of Federal Regulations (CFR)
- 42 CFR 441 Subpart B
- Montana Code Annotated (MCA)
- MCA 53-6-101
- Administrative Rules of Montana (ARM)
- ARM 37.86.2201–37.86.2235
Claims Review (MCA 53-6-111, ARM 37.85.406)
The Department is committed to paying Montana Healthcare programs providers’ claims as quickly as possible. Montana Healthcare programs claims are electronically processed and usually are not reviewed by medical experts prior to payment to determine if the services provided were appropriately billed. Although the computerized system can detect and deny some erroneous claims, there are many erroneous claims which it cannot detect. For this reason, payment of a claim does not mean that the service was correctly billed or the payment made to the provider was correct. The Department performs periodic retrospective reviews, which may lead to the discovery of incorrect billing or incorrect payment. If a claim is paid, and the Department later discovers that the service was incorrectly billed or paid or the claim was erroneous in some other way, the Department is required by federal regulation to recover any overpayment, regardless of whether the incorrect payment was the result of Department or provider error or other cause.
Getting Questions Answered
The provider manuals are designed to answer most questions; however, questions may arise that require a call to a specific group (such as a prior authorization contractor or Provider Relations). The list of Key Contacts at the front of this manual has important phone numbers and addresses pertaining to this manual. The Introduction chapter in the General Information for Providers manual also has a list of contacts for specific Programs policy information. Montana Healthcare programs manuals, provider notices, replacement pages, fee schedules, forms, and much more are available on the Provider Information website (See Key Websites).
Other Department programs
The Montana Healthcare programs orientation and mobility specialist services in this manual are not benefits of the Mental Health Services Plan (MHSP), so the information in this manual does not apply to MHSP. For more information on MHSP, see the mental health manual available on the Provider Information website (See Key Websites).
The Montana Healthcare programs orientation and mobility specialist services in this manual are not covered benefits of Healthy Montana Kids (HMK). Additional information regarding HMK benefits is available by contacting Blue Cross and Blue Shield of Montana at 1 (800) 447-7828, or by visiting the HMK website (See Key Websites).
End of Introduction Chapter
Covered Services
General Coverage Principles
This chapter provides covered services information that applies specifically to services provided by orientation and mobility specialists. Like all health care services received by Montana Healthcare Programs members, services rendered by these providers must also meet the general requirements listed in the General Information for Providers manual, Provider Requirements chapter.
Services within Scope of Practice (ARM 37.86.2235)
Services are covered only when they are within the scope of the provider’s certification. As a condition of participation in the Montana Healthcare Program all providers must comply with all applicable state and federal statutes, rules and regulations, including but not limited to federal regulations and statutes found in Title 42 of the Code of Federal Regulations and the United States Code governing the Montana Healthcare Program and all applicable Montana statutes and rules governing licensure and certification.
Certification
A provider of EPSDT blind and low vision services, or orientation and mobility specialist, must be certified in accordance with the established organizations outlined in ARM 37.86.2235. These include the Academy for Certification of Vision Rehabilitation and Education Professionals (ACVREP) or a National Orientation and Mobility Certification (NOMC) offered by the National Blindness Professional Certification Board (NBPCB).
EPSDT (ARM 37.86.2201–2235)
The Early and Periodic Screening, Diagnosis, and Treatment (EPSDT) program is a comprehensive approach to health care for Montana Healthcare Programs members under age 21. It is designed to prevent, identify, and then treat health problems before they become disabling. Under EPSDT, Montana Healthcare Programs-eligible children may receive any medically necessary covered service, including all orientation and mobility specialist services described in this manual.
Noncovered Services (ARM 37.85.207)
Montana Healthcare Programs does not cover the following services:
- Services provided to Montana Healthcare Programs members who are absent from the state, with the following exceptions:
- Medical emergency;
- Required medical services are not available in Montana. Prior authorization may be required; see the fee schedule on the provider type page of the website.
- If the Department has determined that the general practice for members in a particular area of Montana is to use providers in another state;
- When out-of-state medical services and all related expenses are less costly than in-state services; or
- When Montana makes adoption assistance or foster care maintenance payments for a member who is a child residing in another state.
Coverage of Specific Services
EPSDT blind and low vision services are included as a component under the EPSDT program.
Children with blind or low vision problems may be referred to a certified orientation and mobility specialist for services. The Montana Healthcare Programs blind and low vision services program covers the following services for children under age 21 through the EPSDT program:
- Assessment of the child’s visual status
- Children with blind or low vision needs may be referred to a certified orientation and mobility specialist for services.
- The Montana Healthcare Programs EPSDT blind and low vision services program covers these services for children:
- Sensory integrative techniques to enhance sensory processing and promote adaptive responses to environmental demands.
- Self-care/home management training in activities of daily living (ADLs), instruction in use of assistive/adaptive equipment.
Verifying Coverage
The easiest way to verify coverage for a specific service is to check the Department’s fee schedule for your provider type. In addition to being listed on the fee schedule, all services provided must also meet the coverage criteria listed in this chapter and in the Provider Requirements chapter of the General Information for Providers manual.
Use the fee schedule in conjunction with the more detailed coding descriptions listed in the current CPT and HCPCS coding books. Fee schedules are available on your provider type page on the Provider Information website (See Key Websites).
End of Covered Services Chapter
Passport and Prior Authorization
What Is Passport to Health? (ARM 37.86.5101–5120, ARM 37.86.5303, and ARM 37.86.5201–5206)
Passport to Health is the managed care program for Montana Healthcare Programs and Healthy Montana Kids (HMK) Plus members. The four Passport programs encourage and support Montana Healthcare Programs and HMK Plus members and providers in establishing a medical home and in ensuring the appropriate use of Montana Healthcare Programs and HMK Plus services:
- Passport to Health Primary Care Case Management
- Team Care
Montana Healthcare Programs does not pay for services when prior authorization or Passport requirements are not met.
Montana Healthcare Programs and HMK Plus members who are eligible for Passport must enroll in the program (about 70% of Montana Healthcare Programs and HMK Plus members are eligible). Each enrollee has a designated Passport provider who is typically a physician, midlevel practitioner, or primary care clinic.
Passport to Health Primary Care Case Management (ARM 37.86.5101–5120)
The Passport provider provides primary care case management (PCCM) services to their members. This means he/she provides or coordinates the member’s care and makes referrals to other Montana Healthcare Programs and HMK Plus providers when necessary. Under Passport, Montana Healthcare Programs and HMK Plus members choose one primary care provider (PCP) and develop an ongoing relationship that provides a medical home. The medical home is a concept that encourages a strong doctor-member relationship. An effective medical home is accessible, continuous, comprehensive, coordinated, and operates within the context of family and community.
With some exceptions, all services to Passport members must be provided or approved by the member’s Passport provider or Montana Healthcare Programs/HMK Plus will not reimburse for those services. (See Services That Do Not Require Passport Approval later in this chapter.) The member’s Passport provider is also referred to as the PCP.
Different codes are issued for Passport approval and prior authorization, and both must be recorded on the claim form.
Team Care (ARM 37.86.5303)
Team Care is designed to educate members to effectively access medical care. Members with a history of using services at an amount or frequency that is not medically necessary are enrolled in Team Care. Members enrolled in Team Care are also enrolled in Passport. Team Care follows the same Passport rules and guidelines for referrals, enrollment/disenrollment, prior authorization, and billing processes. However, while Passport members can change providers without cause, as often as once a month, Team Care members are locked in to one provider and one pharmacy. Providers are encouraged to make a referral to the Team Care Program Officer if they feel one of their members is appropriate for the program. A Passport provider receives an enhanced case management fee of $6 per member per month for Team Care members. When checking Montana Healthcare Programs or HMK Plus eligibility on the MATH web portal (See Key Websites). A Team Care member’s provider and pharmacy will be listed. Write all Montana Healthcare Programs and HMK Plus prescriptions to the designated pharmacy.
In practice, providers will most often encounter Montana Healthcare Programs and HMK Plus members who are enrolled in Passport. Specific services may also require prior authorization (PA) even if the member is a Passport enrollee. Passport referral and approval requirements and PA requirements are described in the General Information for Providers manual. Specific PA requirements can be found in the provider fee schedules.
Prior Authorization
Orientation and mobility specialist services that are a covered service of Montana Healthcare Programs generally do not require prior authorization. Refer to the Montana Healthcare Programs fee schedule for your provider type for PA requirements.
End of Passport and Prior Authorization Chapter
Coordination of Benefits
When Members Have Other Coverage
Montana Healthcare Programs members often have coverage through Medicare, workers’ compensation, employment-based coverage, individually purchased coverage, etc. Coordination of benefits is the process of determining which source of coverage is the primary payer in a particular situation. In general, providers should bill other carriers before billing Montana Healthcare Programs, but there are some exceptions (See the Exceptions to Billing Third Party First section in this chapter). Medicare is processed differently than other sources of coverage.
Identifying Additional Coverage
The member’s Montana Healthcare Programs eligibility verification may identify other payers such as Medicare or other third party payers. (See the General Information for Providers manual, Member Eligibility and Responsibilities chapter.) If a member has Medicare, the Medicare ID number is provided. If a member has additional coverage, the carrier is shown. Some examples of third party payers include:
- Private health insurance
- Employment-related health insurance
- Workers’ compensation insurance*
- Health insurance from an absent parent
- Automobile insurance*
- Court judgments and settlements*
- Long-term care insurance
*These third party payers (and others) may not be listed on the member’s Montana Healthcare Programs eligibility verification.
Providers should use the same procedures for locating third party sources for Montana Healthcare Programs members as for their non-Montana Healthcare Programs members. Providers cannot refuse service because of a third party payer or potential third party payer.
When a Member Has Medicare
Medicare claims are processed and paid differently than other non-Montana Healthcare Programs claims. The other sources of coverage are called third party liability or TPL, but Medicare is not.
Medicare Part B Crossover Claims
Orientation and mobility specialist services may be covered under Medicare Part B. The Department has an agreement with the Medicare Part B carrier for Montana (Noridian) and the Durable Medical Equipment Regional Carrier [DMERC]) under which the carriers provide the Department with claims for members who have both Medicare and Montana Healthcare Programs coverage. Providers must tell Medicare that they want their claims sent to Montana Healthcare Programs automatically, and must have their Medicare provider number on file with Montana Healthcare Programs.
To avoid confusion and paperwork, submit Medicare Part B crossover claims to Montana Healthcare Programs only when necessary.
When members have both Medicare and Montana Healthcare Programs covered claims, and have made arrangements with both Medicare and Montana Healthcare Programs, Part B services need not be submitted to Montana Healthcare Programs. When a crossover claim is submitted only to Medicare, Medicare will process the claim, submit it to Montana Healthcare Programs, and send the provider an Explanation of Medicare Benefits (EOMB). Providers must check the EOMB for the statement indicating that the claim has been referred to Montana Healthcare Programs for further processing. It is the provider’s responsibility to follow up on crossover claims and make sure they are correctly billed to Montana Healthcare Programs within the timely filing limit (See the Billing Procedures chapter in this manual).
All Part B crossover claims submitted to Montana Healthcare Programs before the 45-day Medicare response time will be returned to the provider.
Providers should submit Medicare crossover claims to Montana Healthcare Programs only when:
- The referral to Montana Healthcare Programs statement is missing. In this case, submit a claim and a copy of the Medicare EOMB to Montana Healthcare Programs for processing.
- The referral to Montana Healthcare Programs statement is present, but the provider does not hear from Montana Healthcare Programs within 45 days of receiving the Medicare EOMB. Submit a claim and a copy of the Medicare EOMB to Montana Healthcare Programs for processing.
- Medicare denies the claim, you may submit the claim to Montana Healthcare Programs with the EOMB and denial explanation (as long as the claim has not automatically crossed over from Medicare).
When submitting electronic claims with paper attachments, see the Billing Electronically with Paper Attachments section of the Submitting a Claim chapter in this manual.
When submitting a Medicare crossover claim to Montana Healthcare Programs, use Montana Healthcare Programs billing instructions and codes; they may not be the same as Medicare’s.
When submitting a claim with the Medicare EOMB, use Montana Healthcare Programs billing instructions and codes. Medicare’s instructions, codes, and modifiers may not be the same as Montana Healthcare Programs’s. The claim must also include the Montana Healthcare Programs provider number and Montana Healthcare Programs member ID number. It is the provider’s responsibility to follow up on crossover claims and make sure they are correctly billed to Montana Healthcare Programs within the timely filing limit (See the Billing Procedures chapter in this manual).
When a Member Has TPL (ARM 37.85.407)
When a Montana Healthcare Programs member has additional medical coverage (other than Medicare), it is often referred to as third party liability or TPL. In most cases, providers must bill other insurance carriers before billing Montana Healthcare Programs.
Providers are required to notify their members that any funds the member receives from third party payers (when the services were billed to Montana Healthcare Programs) must be turned over to the Department. The following words printed on the member’s statement will fulfill this obligation: “When services are covered by Montana Healthcare Programs and another source, any payment the member receives from the other source must be turned over to Montana Healthcare Programs.”
Exceptions to Billing Third Party First
In a few cases, providers may bill Montana Healthcare Programs first:
- When a Montana Healthcare Programs member is also covered by Indian Health Service (IHS) or Crime Victim Compensation, providers must bill Montana Healthcare Programs first. These are not considered a third party liability.
- When a member has Montana Healthcare Programs eligibility and Mental Health Services Plan (MHSP) eligibility for the same month, Montana Healthcare Programs must be billed before MHSP.
- If the third party has only potential liability, such as automobile insurance, the provider may bill Montana Healthcare Programs first. Do not indicate the potential third party on the claim. Instead, notify the Department of the potential third party by sending the claim and notification directly to the Third Party Liability Unit (See Key Contacts).
Requesting an Exemption
Providers may request to bill Montana Healthcare Programs first under certain circumstances. In each of these cases, the claim and required information should be sent directly to the Third Party Liability Unit (See Key Contacts).
- When a provider is unable to obtain a valid assignment of benefits, the provider should submit the claim with documentation that the provider attempted to obtain assignment and certification that the attempt was unsuccessful.
- When the provider has billed the third party insurance and has received a non-specific denial (e.g., no member name, date of service, amount billed), submit the claim with a copy of the denial and a letter of explanation.
- When the Child Support Enforcement Division has required an absent parent to have insurance on a child, the claim can be submitted to Montana Healthcare Programs when the following requirements are met:
- The third party carrier has been billed, and 30 days or more have passed since the date of service.
- The claim is accompanied by a certification that the claim was billed to the third party carrier, and payment or denial has not been received.
- If another insurance has been billed, and 90 days have passed with no response, submit the claim with a note explaining that the insurance company has been billed, or attach a copy of the letter sent to the insurance company. Include the date the claim was submitted to the insurance company and certification that there has been no response.
When the Third Party Pays or Denies a Service
When a third party payer is involved (excluding Medicare) and the other payer:
- Pays the claim, indicate the amount paid when submitting the claim to Montana Healthcare Programs for processing.
- Allows the claim, and the allowed amount went toward the member’s deductible, include the insurance explanation of benefits (EOB) when billing Montana Healthcare Programs.
- Denies the claim, submit the claim and a copy of the denial (including the reason explanation) to Montana Healthcare Programs.
- Denies a line on the claim, bill the denied line on a separate claim and submit to Montana Healthcare Programs. Include the EOB from the other payer as well as an explanation of the reason for denial (e.g., definition of denial codes).
If the provider receives a payment from a third party after the Department has paid the provider, the provider must return the lower of the two payments to the Department within 60 days.
When the Third Party Does Not Respond
If another insurance has been billed, and 90 days have passed with no response, bill Montana Healthcare Programs as follows:
- Submit the claim and a note explaining that the insurance company has been billed, or attach a copy of the letter sent to the insurance company.
- Include the date the claim was submitted to the insurance company.
- Send this information to the Third Party Liability Unit (See Key Contacts).
End of Coordination of Benefits Chapter
Billing Procedures
Claim Forms
Services provided by orientation and mobility specialist services providers must be billed either electronically or on a CMS-1500 claim form. CMS-1500 forms are available from various publishing companies; they are not available from the Department or Provider Relations.
Timely Filing Limits (ARM 37.85.406)
Providers must submit clean claims to Montana Healthcare Programs within:
- Twelve months from whichever is later:
- the date of service
- the date retroactive eligibility or disability is determined
- For claims involving Medicare or TPL, if the 12-month time limit has passed, providers must submit clean claims to Montana Healthcare Programs:
- Medicare crossover claims: Six months from the date on the Medicare explanation of benefits approving the service (if the Medicare claim was timely filed and the member was eligible for Medicare at the time the Medicare claim was filed).
- Claims involving other third party payers (excluding Medicare): Six months from the date on an adjustment notice from a third party payer who has previously processed the claim for the same service, and the adjustment notice is dated after the periods described above.
Clean claims are claims that can be processed without additional information or action from the provider. All problems with claims must be resolved within this 12-month period.
Tips to Avoid Timely Filing Denials
- Correct and resubmit denied claims promptly (See the Remittance Advices and Adjustments chapter in this manual).
- If a claim submitted to Montana Healthcare Programs does not appear on the remittance advice within 30 days, contact Provider Relations for claim status (See Key Contacts).
- If another insurer has been billed and 90 days have passed with no response, you can bill Montana Healthcare Programs (See the Coordination of Benefits chapter in this manual for more information).
- To meet timely filing requirements for Medicare/Montana Healthcare Programs crossover claims, see the Coordination of Benefits chapter in this manual.
When to Bill Montana Healthcare Programs Members (ARM 37.85.406)
In most circumstances, providers may not bill Montana Healthcare Programs members for services covered under Montana Healthcare Programs. T
More specifically, providers cannot bill members directly:
- For the difference between charges and the amount Montana Healthcare Programs paid.
- When the provider bills Montana Healthcare Programs for a covered service, and Montana Healthcare Programs denies the claim because of billing errors.
- When a third party payer does not respond.
- When a member fails to arrive for a scheduled appointment. Montana Healthcare Programs may not be billed for no-show appointments.
- When services are free to the member. Montana Healthcare Programs may not be billed for those services either.
Under certain circumstances, providers may need a signed agreement in order to bill a Montana Healthcare Programs member (see the following table).
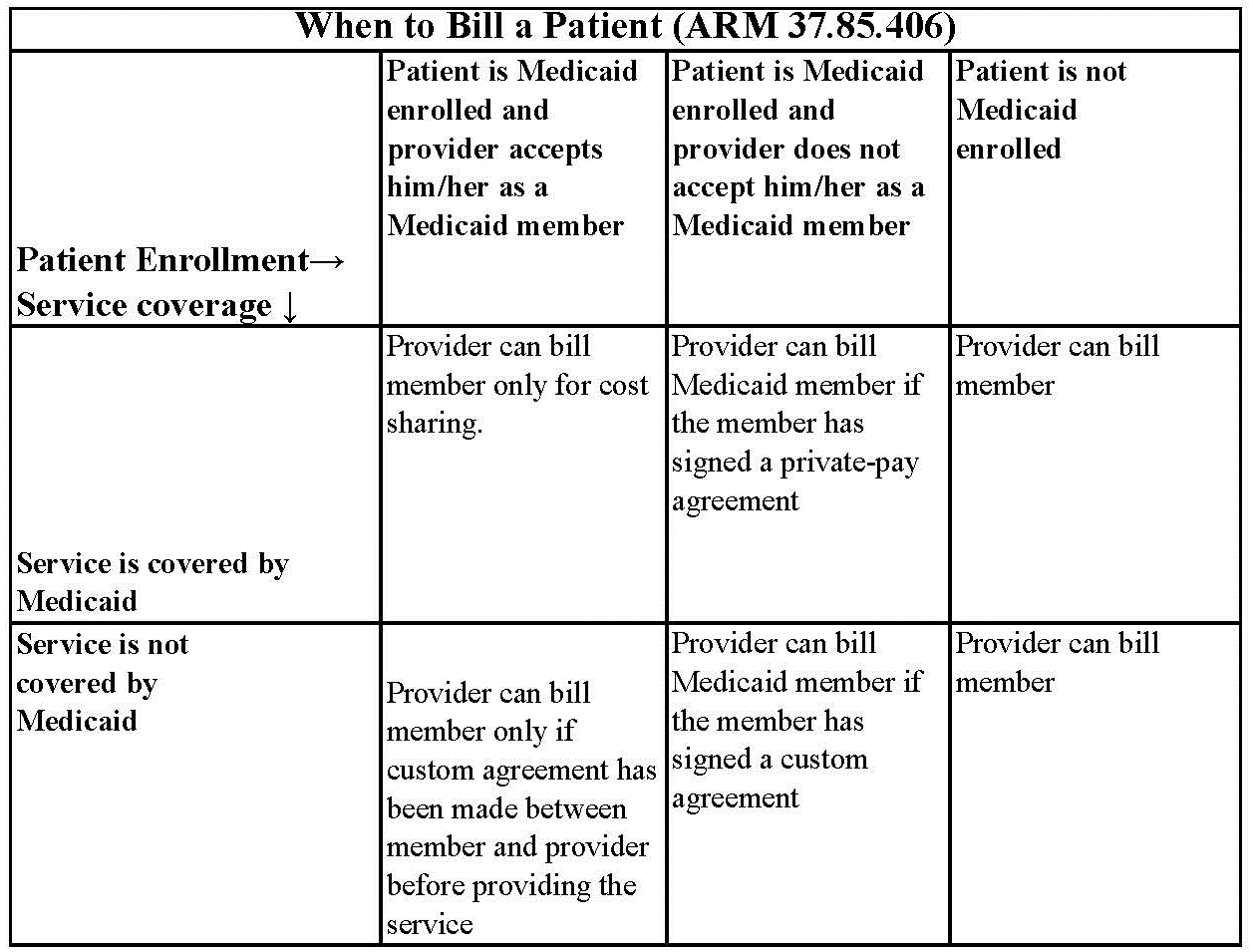
If a provider bills Montana Healthcare Programs and the claim is denied because the member is not eligible, the provider may bill the member directly.
Routine Agreement: This may be a routine agreement between the provider and member which states that the member is not accepted as a Montana Healthcare Programs member, and then he/she must pay for the services received.
Custom Agreement: This agreement lists the service the member is receiving and states that the service is not covered by Montana Healthcare Programs and that the member will pay for it.
When Members Have Other Insurance
If a Montana Healthcare Programs member is also covered by Medicare, has other insurance, or some other third party is responsible for the cost of the member’s health care, see the Coordination of Benefits chapter in this manual.
Billing for Retroactively Eligible Members
When a member becomes retroactively eligible for Montana Healthcare Programs, the provider has 12 months from the date retroactive eligibility was determined to bill for those services. When submitting claims for retroactively eligible members, attach a copy of the FA-455 (eligibility determination letter) to the claim if the date of service is more than 12 months earlier than the date the claim is submitted.
When a provider chooses to accept the member from the date retroactive eligibility was effective, and the member has made a full or partial payment for services, the provider must refund the member’s payment for the services before billing Montana Healthcare Programs for the services.
For more information on retroactive eligibility, see the General Information for Providers manual, Member Eligibility and Responsibilities chapter.
Usual and Customary Charge (ARM 37.85.406)
Providers should bill Montana Healthcare Programs their usual and customary charge for each service; that is, the same charge that is made to other payers for that service.
Coding
Standard use of medical coding conventions is required when billing Montana Healthcare Programs. Provider Relations or the Department cannot suggest specific codes to be used in billing for services. For coding assistance and resources, see the Coding Resources table on the following page. The following suggestions may help reduce coding errors and unnecessary claim denials:
- Use current CPT, HCPCS, and ICD coding books.
- Always read the complete description and guidelines in the coding books. Relying on short descriptions can result in inappropriate billing.
- Attend classes on coding offered by certified coding specialists.
- Use the correct units measurement on the claim.
Coding Resources
Please note that the Department does not endorse the products of any particular publisher.
CPT
Description:
CPT codes and definitions.
Updated each January.
Contact:
American Medical Association
(800) 621-8335
https://commerce.ama-assn.org/store/
CPT Assistant
Description:
A newsletter on CPT coding issues.
Contacts:
American Medical Association
(800) 621-8335
https://commerce.ama-assn.org/store/
HCPCS Level II
Description:
HCPCS codes and definitions.
Updated each January and throughout the year.
Contact:
Available through various publishers and bookstores or from CMS at www.cms.gov.
ICD
Description:
ICD diagnosis and procedure code definitions.
Updated each October.
Contact:
Available through various publishers and bookstores.
Miscellaneous
Various newsletters and other coding resources are available in the commercial marketplace.
NCCI Policy and Edits Manual
Description:
Contains National Correct Coding Initiative (NCCI) policy and edits, which are pairs of CPT or HCPCS codes that are not separately payable except under certain circumstances. The edits are applied to services billed by the same provider for the same member on the same date of service.
Contact:
National Technical Information Service
(800) 363-2068
(703) 605-6060
https://www.cms.gov/Medicare/Coding/NationalCorrectCodInitEd/index.html
Using the Montana Healthcare Programs Fee Schedule
When billing Montana Healthcare Programs, it is important to use the Department’s fee schedule for your provider type in conjunction with the detailed coding descriptions listed in the current CPT and HCPCS coding books.
In addition to covered services and payment rates, fee schedules often contain helpful information such as appropriate modifiers and prior authorization indicators. Department fee schedules are updated each January and July. Fee schedules are available on the provider type pages on the Provider Information website.
Using Modifiers
- Review the guidelines for using modifiers in the CPT, HCPCS, or other helpful resources.
- Always read the complete description for each modifier; some modifiers are described in the CPT manual while others are in the HCPCS book.
- The Montana Healthcare Programs claims processing system recognizes three pricing modifiers and one informational modifier per claim line. Providers are asked to place any modifiers that affect pricing in the first three modifier fields.
- Modifier 52 must be used when billing for a partial EPSDT well-child screen.
Billing Tips for Specific Providers
Orientation and Mobility Specialist Services
Montana Healthcare Programs reimburses orientation and mobility specialist services in 15-minute units. Four units equal one hour of service. Montana Healthcare Programs will pay up to the rate on the fee schedule for each unit of service billed in the Days or Units field of the claim form. Montana Healthcare Programs will not reimburse for two services that duplicate one another on the same day.
The Most Common Billing Errors and How to Avoid Them
Paper claims are often returned to the provider before they can be processed, and many other claims (both paper and electronic) are denied. To avoid unnecessary returns and denials, double-check each claim to confirm the following items are included and are accurate.
Common Billing Errors
Reasons for Returns or Denials:
Provider’s NPI and/or taxonomy missing or invalid
How to Prevent Returned or Denied Claims:
The provider number is a 10-digit number assigned to the provider during Montana Healthcare Programs enrollment. Verify the correct NPI and taxonomy are on the claim.
Reasons for Returns or Denials:
Authorized signature missing
How to Prevent Returned or Denied Claims:
Each claim must have an authorized signature belonging to the provider, billing clerk, or office personnel. The signature may be typed, stamped, or handwritten.
Reasons for Returns or Denials:
Signature date missing
How to Prevent Returned or Denied Claims:
Each claim must have a signature date.
Reasons for Returns or Denials:
Incorrect claim form used
How to Prevent Returned or Denied Claims:
The claim must be the correct form for the provider type. Services covered in this manual require a CMS-1500 claim form.
Reasons for Returns or Denials:
Information on claim form not legible
How to Prevent Returned or Denied Claims:
Information on the claim form must be legible. Use dark ink and center the information in the field. Information must not be obscured by lines.
Reasons for Returns or Denials:
member number not on file, or member was not eligible on date of service
How to Prevent Returned or Denied Claims:
Before providing services to the member:
- View the member’s eligibility information at each visit; Montana Healthcare Programs eligibility may change monthly.
- Verify member eligibility by using one of the methods described in the member Eligibility and Responsibilities chapter of the General Information for Providers manual.
Reasons for Returns or Denials:
Procedure requires Passport provider referral – No Passport provider number on claim
How to Prevent Returned or Denied Claims:
A Passport provider number must be on the claim form when a referral is required. See the Passport chapter in this manual.
Reasons for Returns or Denials:
Duplicate claim
How to Prevent Returned or Denied Claims:
Check all remittance advices (RAs) for previously submitted claims before resubmitting.
When making changes to previously paid claims, submit an adjustment form rather than a new claim form (see Remittance Advices and Adjustments in this manual).
Allow 45 days for the Medicare/Montana Healthcare Programs Part B crossover claim to appear on the RA before submitting the claim directly to Montana Healthcare Programs.
Reasons for Returns or Denials:
Prior authorization number is missing
How to Prevent Returned or Denied Claims:
Prior authorization (PA) is required for certain services, and the PA number must be on the claim form (see the Prior Authorization chapter in this manual).
Reasons for Returns or Denials:
TPL on file and no credit amount on claim
How to Prevent Returned or Denied Claims:
If the member has any other insurance (or Medicare), bill the other carrier before Montana Healthcare Programs. See the Coordination of Benefits chapter in this manual.
If the member’s TPL coverage has changed, providers must notify the TPL Unit (see Key Contacts) before submitting a claim.
Reasons for Returns or Denials:
Claim past 365-day filing limit
How to Prevent Returned or Denied Claims:
The Claims Processing Unit must receive all clean claims and adjustments within the timely filing limits described in this chapter.
To ensure timely processing, claims and adjustments must be mailed to Claims Processing at the address shown in Key Contacts.
Reasons for Returns or Denials:
Missing Medicare EOMB
How to Prevent Returned or Denied Claims:
All Medicare crossover claims on CMS-1500 forms must have an EOMB attached.
Reasons for Returns or Denials:
Provider is not eligible during dates of services, or provider number terminated
How to Prevent Returned or Denied Claims:
Out-of-state providers must update enrollment early to avoid denials. If enrollment has lapsed, claims submitted with a date of service after the expiration date will be denied until the provider updates his or her enrollment.
New providers cannot bill for services provided before Montana Healthcare Programs enrollment begins.
If a provider is terminated from the Montana Healthcare Programs, claims submitted with a date of service after the termination date will be denied.
Reasons for Returns or Denials:
Type of service/procedure is not allowed for provider type
How to Prevent Returned or Denied Claims:
Provider is not allowed to perform the service.
Verify the procedure code is correct using current HCPCS and CPT billing manuals.
Check the Montana Healthcare Programs fee schedule to verify the procedure code is valid for your provider type.
End of Billing Procedures Chapter
Submitting a Claim
Electronic Claims
Professional and institutional claims submitted electronically are referred to as ANSI ASC X12N 837 transactions. Providers who submit claims electronically experience fewer errors and quicker payment. Claims may be submitted electronically by the following methods:
- WINASAP 5010. This free software is available for providers to create and submit claims to Montana Healthcare Programs, MHSP, and HMK (dental and eyeglasses only) and FQHC/RHC. It does not support submissions to Medicare or other payers, and creates an 837 transaction, but does not accept an 835 transaction back from the Department.
- Conduent EDI Solutions Clearinghouse. Providers can send claims to Conduent EDI Solutions (previously EDI Gateway) clearinghouse in X12 837 format using a dial-up connection. Electronic submitters are required to certify their 837 transactions as HIPAA-compliant before sending their transactions through EDI Solutions. EDIFECS certifies the 837 HIPAA transactions at no cost to the provider. EDIFECS certification is completed through EDI Solutions.
- Clearinghouse. Providers can contract with a clearinghouse and send claims to the clearinghouse in whatever format they accept. The provider's clearinghouse then sends the in the X12 837 format. The provider’s clearinghouse also needs to have their 837 transactions certified through EDIFECS before submitting claims. EDIFECS certification is completed through EDI Solutions. For information on electronic claims submission, contact Provider Relations (See Key Contacts).
- Montana Access to Health (MATH) web portal. Providers can upload and download electronic transactions 7 days a week through the web portal. This availability is subject to scheduled and unscheduled host downtime.
- B2B Gateway SFTP/FTPS site. Providers can use this method to send electronic transactions through this secure FTP process. This is typically encountered with high volume/high-frequency submitters.
- MOVEit DMZ. Providers can use this secure transmission protocol and secure storage landing zone (intermediate storage) for the exchange of files between trading partners and Xerox. Its use is intended for those trading partners/submitters who will be submitting a larger volume of physical files (in excess of 20 per day) or whose physical file sizes regularly exceed 2 MB.
Providers should be familiar with the federal rules and regulations on preparing electronic transactions.
Billing Electronically with Paper Attachments
When submitting claims that require additional supporting documentation, the Attachment Control Number field must be populated with an identifier. Identifier formats can be designed by software vendors or clearinghouses, but the preferred method is the provider’s Montana Healthcare Programs ID number followed by the member’s ID number and the date of service, each separated by a dash:

The supporting documentation must be submitted with a Paperwork Attachment Cover Sheet (See the Forms page of the Provider Information website). The number in the paper Attachment Control Number field must match the number on the cover sheet. For more information on attachment control numbers and submitting electronic claims, contact Provider Relations (See Key Contacts).
Paper Claims
The services described in this manual are billed on CMS-1500 claim forms. Claims submitted with all of the necessary information are referred to as clean and are usually paid in a timely manner. (See the Billing Procedures chapter in this manual.)
Claims are completed differently for the different types of coverage a member has (e.g., Montana Healthcare Programs only, Montana Healthcare Programs and Third Party Liability).
When completing a claim, remember the following:
- Required fields are indicated by “*”.
- Fields that are required if the information is applicable to the situation or member are indicated by “**”.
- Field 24h, EPSDT/Family Planning, is used to override copayment and Passport authorization requirements for certain members or services.
The following are accepted codes:
EPSDT/Family Planning Overrides
Code: 1 member/ Service: EPSDT
Purpose: Overrides some benefit limits for member under age 21.
Code: 2 member/ Service: Family planning
Purpose: Overrides the Montana Healthcare Programs Passport authorization on the line.
Code: 3 member/ Service: EPSDT and family planning
Purpose: Overrides Montana Healthcare Programs cost sharing and Passport authorization for persons under the age of 21.
Code: 5 member/ Service: Nursing facility member
Purpose: Overrides the Medicare edit for oxygen services on the line.
Unless otherwise stated, all paper claims are mailed to:
Claims Processing
P.O. Box 8000
Helena, MT 59604
All Montana Healthcare Programs claims must be submitted on Department approved claim forms. CMS-1500 forms are available from various publishing companies; they are not available from the Department or Provider Relations.
CMS-1500 Agreement
Your signature on the CMS-1500 constitutes your agreement to the terms presented on the back of the form. This form is subject to change by the Centers for Medicare and Medicaid Services (CMS).
Claim Inquiries
Claim inquiries can be obtained electronically through ANSI ASC X12N 276/277 transactions or by contacting Provider Relations. Providers may contact Provider Relations for questions regarding payments, denials, and other claim questions (See Key Contacts).
Avoiding Claim Errors
Claims are often denied or even returned to the provider before they can be processed. To avoid denials and returns, double-check each claim form to confirm the following items are accurate. For more information on returned and denied claims, see the Billing Procedures chapter in this manual.
Common Claim Errors
Claim Error: Required field is blank
Prevention: Check the claim instructions earlier in this chapter for required fields (indicated by * or **). If a required field is blank, the claim may either be returned or denied.
Claim Error: member ID number missing or invalid
Prevention: This is a required field (Field 10d); verify that the member’s Montana Healthcare Programs ID number is listed as it appears on the member’s eligibility information.
Claim Error: member name missing
Prevention: This is a required field (Field 2); check that it is correct.
Claim Error: NPI/API missing or invalid
Prevention: The NPI is a 10-digit number (API is a 7-digit) assigned to the provider. Verify the correct NPI/API is on the claim.
Claim Error: Referring or Passport provider name and ID number missing
Prevention: When a provider refers a member to another provider, include the referring provider’s name and ID number or Passport number (see the Passport chapter in this manual).
Claim Error: Prior authorization number missing
Prevention: When prior authorization (PA) is required for a service, the PA number must be on the claim (see the Prior Authorization chapter in this manual).
Claim Error: Not enough information regarding other coverage
Prevention: Fields 1a and 11d are required fields when a member has other coverage (see examples earlier in this chapter).
Claim Error: Authorized signature missing
Prevention: Each claim must have an authorized signature belonging to the provider, billing clerk, or office personnel. The signature may be typed, stamped, or handwritten.
Claim Error: Signature date missing
Prevention: Each claim must have a signature date.
Claim Error: Incorrect claim form used
Prevention: Services covered in this manual require a CMS-1500 claim form.
Claim Error: Information on claim form not legible
Prevention: Information on the claim form must be legible. Use dark ink and center the information in the field. Information must not be obscured by lines.
Claim Error: Medicare EOMB not attached
Prevention: When Medicare is involved in payment on a claim, the Medicare EOMB must be submitted with the claim or it will be denied.
End of Submitting a Claim Chapter
Remittance Advices and Adjustments
Electronic Remittance Advice
The Remittance Advice (RA) is the best tool providers have for determining the status of a claim. RAs accompany payment for services rendered. Beginning July 1, 2013, new providers were required to register for electronic funds transfer (EFT) and electronic RAs. Existing Montana Healthcare Programs providers will transition to electronic payment and RAs over time.
Providers must complete the EDI Trading Partner Agreement, must have registered for the Montana Access to Health (MATH) web portal, and must have Internet access.
The verification process also requires a provider ID, a submitter ID, and a tax ID number. Each provider must complete a Trading Partner Agreement, but if there are several providers in one location who are under one tax ID number, they can use one submitter number. These providers should enter the submitter ID in both the provider number and submitter ID fields. Otherwise, enter the provider number in the provider number field.
After these forms have been processed, the provider will receive a user ID and password that he/she can use to log onto the MATH web portal.
Electronic RAs are available for only 90 days on the web portal.
RAs are available in PDF format. Providers can read, print, or download PDF files using Adobe Acrobat Reader, which is available on the MATH web portal home page. Due to space limitations, each RA is only available for 90 days. Providers should save/print RAs for later reference.
If a claim was denied, read the reason and remark code description before taking any action on the claim.
The RA is divided into the following sections: RA Notice, Paid Claims, Denied Claims, Pending Claims, Credit Balance Claims, Gross Adjustments, and Reason and Remark Codes/Descriptions.
The RA provides details of all transactions that have occurred during the previous RA cycle. Providers are paid weekly. Each line of the RA represents all or part of a claim and explains whether the claim or service has been paid, denied, or suspended (also referred to as pending). If the claim was suspended or denied, the RA also shows the reason.
The pending claims section of the RA is informational only. Do not take any action on claims shown here.
Credit Balance Claims
Credit balances occur when claim adjustments reduce original payments causing the provider to owe money to the Department. These claims are considered in process and continue to appear on the RA until the credit has been satisfied.
The Credit Balance section is informational only. Do not post from credit balance statements.
Credit balances can be resolved in two ways:
- By working off the credit balance. Remaining credit balances can be deducted from future claims. These claims will continue to appear on consecutive RAs until the credit has been paid.
- By sending a check payable to DPHHS for the amount owed. This method is required for providers who no longer submit claims to Montana Healthcare Programs. Attach a note stating that the check is to pay off a credit balance and include your provider number. Send the check to the attention of the Third Party Liability address in Key Contacts.
Rebilling and Adjustments
Rebillings and adjustments are important steps in correcting any billing problems you may experience. Knowing when to use the rebilling process versus the adjustment process is important.
Montana Healthcare Programs does not accept any claim for resubmission or adjustment after 12 months from the date of service. (See Timely Filing Limits in the Billing Procedures chapter.)
Timeframe for Rebilling or Adjusting a Claim
- Providers may resubmit, modify, or adjust any initial claim within the timely filing limits described in the Billing Procedures chapter of this manual.
- The time periods do not apply to overpayments that the provider must refund to the Department. After the 12-month time period, a provider may not refund overpayments to the Department by completing a claim adjustment. The provider may refund overpayments by issuing a check, or request Provider Relations to complete a gross adjustment.
Rebilling Montana Healthcare Programs
Rebilling is when a provider submits a claim to Montana Healthcare Programs that was previously submitted for payment but was either returned or denied. Claims are often returned to the provider before processing because key information such as Montana Healthcare Programs provider number or authorized signature and date are missing or unreadable. For tips on preventing returned or denied claims, see the Billing Procedures chapter in this manual.
When to Rebill Montana Healthcare Programs
- Claim Denied. Providers may rebill Montana Healthcare Programs when a claim is denied. Check the Reason and Remark Codes, make the appropriate corrections, and resubmit the claim. Do not use and adjustment form.
- Line denied. When an individual line is denied on a multiple-line claim, correct any errors and submit only the denied line to Montana Healthcare Programs. For CMS-1500 claims, do not use an adjustment form.
- Claim returned. Rebill Montana Healthcare Programs when the claim is returned under separate cover. Occasionally, Montana Healthcare Programs is unable to process the claim and will return it to the provider with a letter stating that additional information is needed to process the claim. Correct the information as directed and resubmit the claim.
How to Rebill
- Check any Reason and Remark Code listed and make corrections on a copy of the claim, or produce a new claim with the correct information.
- When making corrections on a copy of the claim, remember to line out or omit all lines that have already been paid.
- Submit insurance information with the corrected claim.
Rebill denied claims only after appropriate corrections have been made.
Adjustments
If a provider believes that a claim has been paid incorrectly, the provider may call Provider Relations. Once an incorrect payment has been verified, the provider should submit an Individual Adjustment Request form to Provider Relations. If incorrect payment was the result of a Conduent Services keying error, contact Provider Relations.
When adjustments are made to previously paid claims, the Department recovers the original payment and issues appropriate repayment. The result of the adjustment appears on the provider’s RA as two transactions. The original payment will appear as a credit transaction. The replacement claim reflecting the corrections will be listed as a separate transaction and may or may not appear on the same RA as the credit transaction. The replacement transaction will have nearly the same ICN number as the credit transaction, except the 12th digit over will be a 2, indicating an adjustment. Adjustments are processed in the same time frame as claims.
When to Request an Adjustment
- Request an adjustment when the claim was overpaid or underpaid.
- Request an adjustment when the claim was paid but the information on the claim was incorrect (e.g., member ID, provider number, date of service, procedure code, diagnoses, units).
How to Request an Adjustment
To request an adjustment, download the Montana Health Care Programs Individual Adjustment Request form from the Provider Information website. A copy is also in Appendix A: Forms. The requirements for adjusting a claim are as follows:
- Adjustments can only be submitted on paid claims; denied claims cannot be adjusted.
- Claims Processing must receive individual claim adjustments within 12 months from the date of service. (See Timely Filing in the Billing Procedures chapter of this manual.) After this time, gross adjustments are required (see the Definitions and Acronyms chapter).
- Use a separate adjustment request form for each ICN.
- If you are correcting more than one error per ICN, use only one adjustment request form, and include each error on the form.
- If more than one line of the claim needs to be adjusted, indicate which lines and items need to be adjusted in the Reason and Remarks section.
Completing an Adjustment Request Form
- Download the Individual Adjustment Request form from the Provider Information website. Complete Section A first with provider and member information and the claim’s ICN number (see following table).
- Complete Section B with information about the claim. Remember to fill in only the items that need to be corrected (see following table):
- Enter the date of service or the line number in the Date of Service or Line Number column.
- Enter the information from the claim form that was incorrect in the Information on Statement column.
- Enter the correct information in the column labeled Corrected Information.
- Attach copies of the RA and a corrected claim if necessary.
- If the original claim was billed electronically, a copy of the RA will suffice.
- If the RA is electronic, attach a screen print of the RA.
- Verify the adjustment request has been signed and dated.
- Send the adjustment request to Claims Processing (See Key Contacts).
Completing an Individual Adjustment Request Form
Section A
Field: 1. Provider Name and Address
Description: Provider’s name and address (and mailing address if different).
Field: 2. Recipient Name
Description: The member’s name.
Field: 3.* Internal Control Number (ICN)
Description: There can be only one ICN per Adjustment Request form. When adjusting a claim that has been previously adjusted, use the ICN of the most recent claim.
Field: 4*. Provider number
Description: The provider’s Montana Healthcare Programs ID number.
Field: 5*. Recipient Montana Healthcare Programs Number
Description: member’s Montana Healthcare Programs ID number.
Field: 6. Date of Payment
Description: Date claim was paid found on Remittance Advice Field 5 (see the sample RA earlier in this chapter).
Field: 7. Amount of Payment
Description: The amount of payment from the Remittance Advice Field 19 (see the sample RA earlier in this chapter.).
Section B
Field: 1. Units of Service
Description: If a payment error was caused by an incorrect number of units, complete this line.
Field: 2. Procedure Code/NDC/Revenue Code
Description: If the procedure code, NDC, or revenue code are incorrect, complete this line.
Field: 3. Dates of Service (DOS)
Description: If the date of service is incorrect, complete this line.
Field: 4. Billed Amount
Description: If the billed amount is incorrect, complete this line.
Field: 5. Personal Resource (Nursing Facility)
Description: If the member’s personal resource amount is incorrect, complete this line.
Field: 6. Insurance Credit Amount
Description: If the member’s insurance credit amount is incorrect, complete this line.
Field: 7. Net (Billed - TPL or Medicare Paid)
Description: If the payment error was caused by a missing or incorrect insurance credit, complete this line. Net is billed amount minus the amount TPL or Medicare paid.
Field: 8. Other/Remarks
Description: If none of the above items apply, or if you are unsure what caused the payment error, complete this line.
*Indicates a required field
- If an original payment was an underpayment by Montana Healthcare Programs, the adjustment results in the provider receiving the additional payment amount allowed.
- If an original payment was an overpayment by Montana Healthcare Programs, the adjustment results in recovery of the overpaid amount from the provider. This can be done in 2 ways: by the provider issuing a check to the Department or by maintaining a credit balance until it has been satisfied with future claims (See Credit Balance in this chapter).
- Any questions regarding claims or adjustments should be directed to Provider Relations (See Key Contacts).
Mass Adjustments
Mass adjustments are done when it is necessary to reprocess multiple claims. They generally occur when:
- Montana Healthcare Programs has a change of policy or fees that is retroactive. In this case federal laws require claims affected by the changes to be mass adjusted.
- A system error that affected claims processing is identified.
Providers are informed of mass adjustments on the first page of the remittance advice (RA Notice section), the monthly Claim Jumper newsletter, or provider notice. Mass adjustment claims shown on the RA have an ICN that begins with a 4.
Payment and the RA
Providers receive their Montana Healthcare Programs payment via electronic funds transfer (EFT) their remittance advice electronically. Direct deposit is another name for EFT. To participate in EFT, providers must complete a Direct Deposit Sign-Up Form (Standard Form 1199A) (see the following table). One form must be completed for each provider number.
With EFT, the Department deposits the funds directly to the provider’s bank account. If the scheduled deposit day is a holiday, funds will be available on the next business day. Electronic RAs will also be available the next business day.
Once electronic transfer testing shows payment to the provider’s account, all Montana Healthcare Programs payments will be made through EFT (See Direct Deposit Arrangements under Key Contacts).
End of Remittance Advices and Adjustments Chapter
How Payment Is Calculated
Overview
Though providers do not need the information in this chapter in order to submit claims to the Department, the information allows providers to understand how payment is calculated and to predict approximate payment for particular claims. These examples are for July 2013 and these rates may not apply at other times.
How Payment is Calculated on TPL Claims
When a member has coverage from both Montana Healthcare Programs and another insurance company, the other insurance company is often referred to as third party liability or TPL. In these cases, the other insurance is the primary payer (as described in the Coordination of Benefits chapter in this manual), and Montana Healthcare Programs makes a payment as the secondary payer. For example, a member receives one visit of EPSDT orientation and mobility services (97533). The third party insurance is billed first and pays $15.00. The Montana Healthcare Programs allowed amount for this service totals $29.21. The amount the insurance paid ($15.00) is subtracted from the Montana Healthcare Programs allowed amount ($29.21), leaving a balance of $14.21, which Montana Healthcare Programs will pay on this claim.
Many Montana Healthcare Programs payment methods are based on Medicare, but there are differences. In these cases, the Montana Healthcare Programs method prevails.
How Payment is Calculated on Medicare Crossover Claims
When a member has coverage from both Montana Healthcare Programs and Medicare, Medicare is the primary payer as described in the Coordination of Benefits chapter of this manual. Montana Healthcare Programs then makes a payment as the secondary payer. For the provider types covered in this manual, Montana Healthcare Programs’s payment is calculated so that the total payment to the provider is either the Montana Healthcare Programs allowed amount less the Medicare paid amount or the sum of the Medicare coinsurance and deductible, whichever is lower. This method is sometimes called “lower of” pricing.
Other Factors That May Affect Payment
When Montana Healthcare Programs payment differs from the fee schedule, consider the following:
- The Department pays the lower of the established Montana Healthcare Programs fee or the provider’s charge
- The member may have an incurment amount that must be met before Montana Healthcare Programs will pay for services. (See the General Information for Providers manual, Member Eligibility and Responsibilities chapter, Coverage for the Medically Needy section.)
- Date of service; fees for services may change over time.
- Cost sharing, Medicare, and/or TPL payments, which are shown on the remittance advice.
End of How Payment Is Calculated Chapter
Appendix A: Forms
- Montana Health Care Programs Montana Healthcare Programs/MHSP/HMK Individual Adjustment Request
- Paperwork Attachment Cover Sheet
End of Appendix A: Forms Chapter
Definitions and Acronyms
This section contains definitions, abbreviations, and acronyms used in this manual.
270/271 Transactions
The X12N eligibility inquiry (270) and response (271) transactions.
276/277 Transactions
The X12N claim status request (276) and response (277) transactions.
278 Transactions
The X12N request for services review and response used for prior authorization.
835 Transactions
The X12N payment and remittance advice (explanation of benefits) transaction.
837 Transactions
The X12N professional, institutional, and dental claim transactions.
Accredited Standards Committee X12, Insurance Subcommittee (ASC X12N)
The ANSI-accredited standards development organization and one of the 6 Designated Standards Maintenance Organizations (DSMO) that created and is tasked with maintaining the administrative and financial transactions standards adopted under HIPAA for all health plans, clearinghouses, and providers who use electronic transactions.
Adjustment
A transaction that changes any payment or other claim information on a previously paid claim.
Administrative Review
Administrative reviews are the Department’s effort to resolve a grievance about a Department decision in order to avoid a hearing. The review includes an informal conference with the Department to review facts, legal authority, and circumstances involved in the adverse action by the Department.
Administrative Rules of Montana (ARM)
The rules published by the executive departments and agencies of the state government.
Assignment of Benefits
A voluntary decision by the member to have insurance benefits paid directly to the provider rather than to the member. The act requires the signing of a form for the purpose. The provider is not obligated to accept an assignment of benefits. However, the provider may require assignment in order to protect the provider’s revenue.
Audit
A formal or periodic verification of accounts.
Authorization
An official approval for action taken for, or on behalf of, a Montana Healthcare Programs member. This approval is only valid if the member is eligible on the date of service.
Basic Montana Healthcare Programs
members with Basic Montana Healthcare Programs have limited Montana Healthcare Programs services. See the General Information for Providers manual, Montana Healthcare Programs Covered Services chapter.
Carrier
A private insurance company.
Centers for Medicare and Medicaid (CMS)
Administers the Medicare program and oversees the state Montana Healthcare Programs s.
Claims Clearinghouse
When a provider contracts with a clearinghouse, the clearinghouse supplies the provider with software that electronically transmits claims to the clearinghouse. The clearinghouse then transmits the claims to the appropriate payers.
Clean Claim
A claim that can be processed without additional information or documentation from or action by the provider of the service.
Coinsurance
The member's financial responsibility for a medical bill as assigned Medicare (usually a percentage). Medicare coinsurance is usually 20% of the Medicare allowed amount.
Cosmetic
Serving to modify or improve the appearance of a physical feature, defect, or irregularity.
Cost Sharing
The member’s financial responsibility for a medical bill assessed by flat fee or percentage of charges.
Credit Balance Claims
Adjusted claims that reduce original payments, causing the provider to owe money to the Department. These claims are considered in process and continue to appear on the remittance advice until the credit has been satisfied.
Crossovers
Claims for members who have both Medicare and Montana Healthcare Programs. These claims may come electronically from Medicare or directly from the provider.
Current Procedural Terminology (CPT)
Physicians’ Current Procedural Terminology contains procedure codes which are used by medical practitioners in billing for services rendered. The book is published by the American Medical Association.
DPHHS, State Agency
The Montana Department of Public Health and Human Services (DPHHS or the Department) is the designated State Agency that administers the Montana Health Care Programs. The Department’s legal authority is contained in Title 53, Chapter 6 MCA. At the federal level, the legal basis for the program is contained in Title XIX of the Social Security Act and Title 42 of the Code of Federal Regulations (CFR). The program is administered in accordance with the Administrative Rules of Montana (ARM), Title 37, Chapter 86.
Early & Periodic Screening, Diagnosis, and Treatment (EPSDT)
This program provides Montana Healthcare Programs-covered children with comprehensive health screenings, diagnostic services, and treatment of health problems.
Electronic Data Interchange (EDI)
The communication of information in a stream of data from one party’s computer system to another party’s computer system.
Electronic Funds Transfer (EFT)
Payment of medical claims that are deposited directly to the provider’s bank account.
Emergency Services
A service is reimbursed as an emergency if one of the following criteria is met: The service is billed with CPT code 99284 or 99285; the member has a qualifying emergency diagnosis code. A list of emergency diagnosis codes is available on the Provider Information website; the services did not meet one of the previous two requirements, but the hospital believes an emergency existed. In this case, the claim and documentation supporting the emergent nature of the service must be mailed to the emergency department review contractor. (See Key Contacts on your provider type page or in your provider manual.)
Explanation of Benefits (EOB) Codes
A 3-digit code which prints on Montana Healthcare Programs remittance advice (RA) that explains why a claim was denied or suspended. The explanation of the EOB codes is found at the end of the RA.
Explanation of Medicare Benefits (EOMB)
A notice sent to providers informing them of the services which have been paid by Medicare.
Fair Hearing
Providers may request a fair hearing when the provider believes the Department’s administrative review determination fails to comply with applicable laws, regulations, rules or policies. Fair hearings include a hearings officer, attorneys, and witnesses for both parties.
Fiscal Agent
Conduent Healthcare LLC, is the fiscal agent for the State of Montana and processes claims at the Department's direction and in accordance with ARM 37.86 et seq.
Full Montana Healthcare Programs
members with Full Montana Healthcare Programs have a full scope of Montana Healthcare Programs benefits. See the General Information for Providers manual, Montana Healthcare Programs Covered Services chapter.
Gross Adjustment
A lump sum debit or credit that is not claim specific made to a provider.
HCPCS
Coding System, and is pronounced “hick-picks.” There are two types of HCPCS codes:
- Level 1 includes the CPT codes.
- Level 2 includes the alphanumeric codes A–V which CMS maintains for a wide range of services from ambulance trips to hearing aids which are not addressed by CPT coding.
Health Improvement Program (HIP)
A service provided under the Passport to Health program for members who have one or more chronic health conditions. Care management focuses on helping members improve their health outcomes through education, help with social services, and coordination with the member’s medical providers.
Health Insurance Portability and Accountability Act (HIPAA)
A federal plan designed to improve efficiency of the health care system by establishing standards for transmission, storage, and handling of data.
Healthy Montana Kids (HMK)
HMK offers low-cost or free health care coverage for low-income children younger than 19. Children must be uninsured U.S. citizens or qualified aliens, Montana residents who are not eligible for Montana Healthcare Programs. DPHHS administers the program with Blue Cross and Blue Shield of Montana (BCBSMT). For eligibility and enrollment information, contact HMK at 1 (877) 543-7669 (toll-free, follow menu) or 1 (855) 258-3489 (toll-free, direct). For information about medical benefits, contact BCBSMT at 1 (406) 447-8647 (Helena) or 1 (800) 447-7828 (toll-free). HMK dental and eyeglasses benefits are provided by DPHHS through the same contractor (Conduent State Healthcare, LLC) that handles Montana Healthcare Programs provider relations and claims processing.
Indian Health Service (IHS)
IHS provides federal health services to American Indians and Alaska Natives.
Internal Control Number (ICN)
The unique number assigned to each claim transaction that is used for tracking.
International Classification of Diseases (ICD)
The International Classification of Diseases contains the diagnosis codes used in coding claims and the procedure codes used in billing for services performed in a hospital setting.
Mass Adjustment
Adjustments made to multiple claims at the same time. They generally occur when the Department has a change of policy or fees that is retroactive, or when a system error that affected claims processing is identified.
Montana Healthcare Programs/HMK Plus
A program that provides health care coverage to specific populations, especially low-income families with children, pregnant women, disabled people and the elderly. Montana Healthcare Programs is administered by state governments under broad federal guidelines.
Medically Necessary
A term describing a requested service which is reasonably calculated to prevent, diagnose, correct, cure, alleviate or prevent worsening of conditions in the member. These conditions must be classified as one of the following: endanger life, cause suffering or pain, result in an illness or infirmity, threaten to cause or aggravate a handicap, or cause physical deformity or malfunction. There must be no other equally effective, more conservative or substantially less costly course of treatment available or suitable for the member requesting the service. For the purpose of this definition, course of treatment may include mere observation or, when appropriate, no treatment at all.
Medicare
The federal health insurance program for certain aged or disabled members.
Member
An individual enrolled in a Department medical assistance program.
Mental Health Services Plan (MHSP)
This plan is for individuals who have a severe disabling mental illness (SDMI), are ineligible for Montana Healthcare Programs, and have a family income that does not exceed an amount established by the Department.
Passport Referral Number
This is a 7-digit number assigned to Passport providers. When a Passport provider refers a member to another provider for services, this number is given to the other provider and is required when processing the claim.
Passport to Health
The Montana Healthcare Programs medical home program where the member selects a primary care provider who manages the member’s health care needs.
Pay-and-Chase
Montana Healthcare Programs pays a claim and then recovers payment from the third party carrier that is financially responsible for all or part of the claim.
Pending Claim
These claims have been entered into the system, but have not reached final disposition. They require either additional review or are waiting for member eligibility information.
Potential Third Party Liability
Any entity that may be liable to pay all or part of the medical cost of care for a Montana Healthcare Programs/HMK Plus, MHSP, or HMK member.
Prior Authorization (PA)
The approval process required before certain services or supplies are paid by Montana Healthcare Programs. Prior authorization must be obtained before providing the service or supply.
Provider or Provider of Service
An institution, agency, or person having a signed agreement with the Department to furnish medical care, goods and/or services to members, and who is eligible to receive payment from the Department.
Qualified Individual
For these members, Montana Healthcare Programs pays the Medicare premium only. They are not eligible for other Montana Healthcare Programs benefits, and they must pay their own Medicare insurance and deductibles.
Qualified Medicare Beneficiary (QMB)
QMB members are members for whom Montana Healthcare Programs pays their Medicare premiums and some or all of their Medicare coinsurance and deductibles.
Rebilling
When a provider submits a claim that was previously submitted for payment but was either returned or denied.
Referral
When providers refer members to other Montana Healthcare Programs providers for medically necessary services that they cannot provide.
Remittance Advice (RA)
The results of claims processing (including paid, denied, and pending claims) are listed on the RA.
Remittance Advice Notice
The first page of the RA that contains important messages for providers.
Retroactive Eligibility
When a member is determined to be eligible for Montana Healthcare Programs effective prior to the current date.
Taxonomy
Taxonomy codes are used to identify and code an external provider table that would be able to standardize provider types and provider areas of specialization for medical-related providers.
Team Care
A restricted services program that is part of Passport to Health. Restricted services programs are designed to assist members in making better health care decisions so that they can avoid overutilizing health services. Team Care members are joined by a team assembled to assist them in accessing health care. The team consists of the member, the PCP, a pharmacy, the Department, and the Department's quality improvement organization. The team may also include a community-based care manager from the Department’s Health Improvement Program.
Third Party Liability (TPL)
Any entity that is liable to pay all or part of the medical cost of care for a Montana Healthcare Programs/HMK Plus, MHSP, or HMK member.
Timely Filing
Providers must submit clean claims (claims that can be processed without additional information or documentation from or action by the provider) to Montana Healthcare Programs within:
- 12 months from whichever is later:
- The date of service.
- The date retroactive eligibility or disability is determined.
- 6 months from the date on the Medicare explanation of benefits approving the service.
- 6 months from the date on an adjustment notice from a third party payer who has previously processed the claim for the same service, and the adjustment notice is dated after the periods described above.
Usual and Customary
The fee that the provider most frequently charges the general public for a service or item.
End of Definitions and Acronyms Chapter
Search Options
Previous editions of this manual contained an index.
This edition has three search options.
- Search the whole manual. Open the Complete Manual pane. From your keyboard press the Ctrl and F keys at the same time. A search box will appear. Type in a descriptive or key word (for example "Denials". The search box will show all locations where denials discussed in the manual.
- Search by Chapter. Open any Chapter tab (for example the "Billing Procedures" tab). From your keyboard press the Ctrl and F keys at the same time. A search box will appear. Type in a descriptive or key word (for example "Denials". The search box will show where denials discussed in just that chapter.
- Site Search. Search the manual as well as other documents related to a particular search term on the Montana Healthcare Programs Site Specific Search page.
End of Search Options Chapter
End of Orientation and Mobility Specialist Services Manual
Update Log
Orientation and Mobility Specialist Services Manual
To print this manual, right click your mouse and choose "print". Printing the manual material found at this website for long-term use is not advisable. Department Policy material is updated periodically and it is the responsibility of the users to check and make sure that the policy they are researching or applying has the correct effective date for their circumstances.
Publication History
This publication supersedes all previous Orientation and Mobility Specialist Services handbooks. Published by the Montana Department of Public Health & Human Services, January 2005.
Updated January 2011, December 2011, March 2012, October 2016, April 2017, June 2017, June 2018, January 2020, and April 2022.
CPT codes, descriptions and other data only are copyright 2014 American Medical Association (or such other date of publication of CPT). All Rights reserved. Applicable FARS/DFARS Apply.
Update Log
04/14/2022
- Removed Nurse First Advice Line references.
- Removed HIP references.
- Updated Index to Search Options.
01/01/2020
- Cost Share references removed from Billing Procedures, and Submitting A Claim Chapters.
- Term "Medicaid" replaced with "Montana Healthcare Programs" throughout the manual.
06/04/2018
Removed commercial resource references.
06/20/2017
Orientation and Mobility Specialist Services Manual converted to an HTML format and adapted to 508 Accessibility Standards.
End Update Log Chapter
Table of Contents
Key Contacts
Key Websites
Introduction
Manual Organization
Manual Maintenance
Rule References
Claims Review (MCA 53-6-111, ARM 37.85.406)
Getting Questions Answered
Othe Department Programs
Covered Services
General Coverage Principles
- Services within Scope of Practice (ARM 37.86.2235)
- Certification
- EPSDT (ARM 37.86.2201-2235)
Noncovered Services (ARM 37.85.207)
Coverage of Specific Services
Verifying Coverage
Passport and Prior Authorization
What Is Passport to Health? (ARM 37.85.5101-5120, ARM 37.86.5303 and 37.86.5201-5206)
- Passport to Health Primary Care Case Management (ARM 37.86.5101-5120)
- Team Care (ARM 37.86.5303)
Prior Authorization
Coordination of Benefits
When Members Have Other Coverage
Identifying Additional Coverage
When a Member Has Medicare
- Medicare Part B Crossover Claims
When a Member Has TPL (ARM 37.85.407)
- Exceptions to Billing Third Party First
- Requesting an Exemption
- When the Third Party Pays or Denies a Service
- When the Third Party Does Not Respond
Billing Procedures
Claim Forms
Timely Filing Limits (ARM 37.85.406)
- Tips to Avoid Timely Filing Denials
When to Bill Montana Healthcare Members (ARM 37.85.406)
Member Co-Payments (ARM 37.85.204)
When Members Have Other Insurance
Billing for Retroactively Eligible Members
Usual and Customary Charge (ARM 37.85.406)
Coding
Using the Montana Healthcare Programs Fee Schedule
Using Modifiers
Billing Tips for Specific Providers
- Orientation and Mobility Specialist Services
The Most Common Billing Errors and How to Avoid Them
Submitting a Claim
Electronic Claims
Billing Electronically with Paper Attachments
Paper Claims
CMS-1500 Agreement
Claim Inquiries
Avoiding Claim Errors
Remittance Advices and Adjustments
Electronic Remittance Advice
- Credit Balance Claims
Rebilling and Adjustments
- Timeframe for Rebilling or Adjusting a Claim
- Rebilling Montana Healthcare Programs
- How to Rebill
- Adjustments
- When to Request an Adjustment
- How to Request an Adjustment
- Completing an Adjustment Request Form
- Mass Adjustments
Payment and the RA
How Payment Is Calculated
Overview
How Payment is Calculated on TPL Claims
How Payment is Calculated on Medicare Crossover Claims
Other Factors That May Affect Payment
Appendix A: Forms
Individual Adjustment Request
Paperwork Attachment Cover Sheet
Definitions and Acronyms
Index
End of Table of Contents Chapter
Key Contacts
Hours for Key Contacts are 8:00 a.m. to 5:00 p.m. Monday through Friday (Mountain Time), unless otherwise stated. The phone numbers designated “In state” will not work outside Montana.
Direct Deposit Arrangements
Providers who need to enroll in electronic funds transfer (EFT) and register for electronic remittance advices (RAs) should contact Provider Relations for assistance. Providers should mail or fax their completed documentation to Provider Relations:
Provider Relations
P.O. Box 4936
Helena, MT
1 (800) 624-3958 or (406) 442-4402
(406) 442-4402 Fax
EDI Solutions Help Desk
For questions regarding electronic claims submission:
(800) 987-6719 In/Out of state
(406) 442-1837 Helena
(850) 385-1705 Fax
Send e-mail inquiries to:
Mail to:
EDI Solutions Montana
P.O. Box 4936
Helena, MT 59604
Member Eligibility
There are several methods for verifying member eligibility. The most commonly used methods are below. For additional methods and details on each, see the Member Eligibility and Responsibilities chapter in the General Information for Providers manual.
FaxBack: (800) 714-0075 (24 hours)
Voice Response System: (800) 362-8312 (24 hours)
Montana Access to Health Web Portal: https://mtaccesstohealth.portal.conduent.com/mt/general/home.d
Medifax EDI: (800) 444-4336 Ext. 2072 (24 hours)
Orientation and Mobility Specialist Services
(406) 444-4066 In/Out of state
(406) 444-1861 Fax
Send written inquiries to:
O&M Specialist Program Officer
DPHHS
P.O. Box 202951
Helena, MT 59620-2951
Paper Claims
Send paper claims to:
Claims Processing Unit
P.O. Box 8000
Helena, MT 59604
Parents Let’s Unite for Kids (PLUK)
PLUK
516 North 32nd Street
Billings, MT 59101-6003
(406) 255-0540 Phone
(800) 222-7585 Phone
(406) 255-0523 Fax
E-mail: info@pluk.org
Website: http://www. pluk.org/
Provider Relations
For questions about eligibility, payments, denials, or general claims questions, or questions about Montana Healthcare Programs or Passport provider enrollment, address or phone number changes:
(800) 624-3958 In/Out of state
(406) 442-1837 Helena
Send e-mail inquiries to: MTPRHelpdesk@conduent.com
Send written inquiries to:
Provider Enrollment Unit
P.O. Box 4936
Helena, MT 59604
Provider’s Policy Questions
For policy questions, contact the appropriate division of the Department of Public Health and Human Services; see the Introduction chapter in the General Information for Providers manual.
Secretary of State
The Secretary of State’s office publishes the most current version of the Administrative Rules of Montana (ARM).
(406) 444.2055 Phone
Send written inquiries to:
Secretary of State
P.O. Box 202801
Helena, MT 59620-2801
Team Care
For questions about the Team Care program:
(406) 444-4540 Phone
(406) 444-1861 Fax
Send written inquiries to:
Team Care Program Officer
Managed Care Bureau
DPHHS
P.O. Box 202951
Helena, MT 59620-2951
Third Party Liability
For questions about private insurance, Medicare or other third party liability:
(800) 624-3958 In/Out of state
(406) 442-1837 Helena
(406) 442-4402 Fax
Send written inquiries to:
Third Party Liability Unit
P.O. Box 5838
Helena, MT 59604
End of Key Contacts Chapter
Key Websites
EDI Gateway - https://edisolutionsmmis.portal.conduent.com/gcro/
Gateway is Montana’s HIPAA clearinghouse. Visit this website for more information on:
- EDI support
- Enrollment
- Manuals
- Provider services
- Software
Health Resources Division
- Big Sky Rx: Helps Medicare members pay for Medicare-approved prescription drug insurance premiums.
- Electronic Billing: How to submit Montana Healthcare Programs claims electronically.
- Healthy Montana Kids: Information on HMK. See website below.
- Montana Healthcare Programs member: Montana Healthcare Programs services for adults and children.
- Montana Healthcare Programs Provider Information: See Montana Access to Health (MATH) Web Portal and Provider Information Website below.
- Montana Healthcare Programs Fraud and Abuse Reporting: Provides telephone numbers to call if you have concerns about Montana Healthcare Programs fraud or abuse.
- Montana Healthcare Programs:
- Passport to Health: Information and enrollment forms for the Passport to Health primary care case management program.
- Prescription Assistance Programs: Summary of information on the programs designed to make prescription drugs more affordable.
- Team Care: Information and enrollment information for the Team Care program.
Provider Information Website
https://medicaidprovider.mt.gov/
- Fee schedules
- Forms
- Frequently asked questions (FAQs)
- HIPAA update
- Key contacts
- Links to other websites and more
- Montana Healthcare Programs news
- Newsletters
- Provider enrollment
- Provider manuals, notices and manual replacement pages
- Remittance advice notices
- Upcoming events
End of Key Websites Chapter
Introduction
Thank you for your willingness to serve members of the Montana Healthcare Programs and other medical assistance Programs administered by the Department of Public Health and Human Services.
Manual Organization
This manual provides information specifically for providers of orientation and mobility specialist services. Additional essential information for providers is contained in the separate General Information for Providers manual. Each provider is asked to review both manuals.
A table of contents and an index allow you to quickly find answers to most questions. The margins contain important notes with extra space for writing notes. Each manual contains a list of Key Contacts. We have also included a space on the back of the front cover to record your NPI/API for quick reference when calling Provider Relations.
Manual Maintenance
In order to remain accurate, manuals must be kept current. Changes to manuals are provided through notices and replacement pages, which are posted on the Provider Information website. (See Key Websites.) When replacing a page in a paper manual, file the old pages and notices in the back of the manual for use with claims that originated under the old policy.
Rule References
Providers must be familiar with all current rules and regulations governing the Montana Healthcare Programs. Provider manuals are to assist providers in billing Montana Healthcare programs; they do not contain all Montana Healthcare programs rules and regulations. Rule citations in the text are a reference tool; they are not a summary of the entire rule. In the event that a manual conflicts with a rule, the rule prevails. Links to rules are available on the Provider Information website (See Key Websites). Paper copies of rules are available through the Secretary of State’s office (See Key Contacts).
Providers are responsible for knowing and following current laws and regulations.
In addition to the Montana Healthcare programs rules outlined in the General Information for Providers manual, the following rules and regulations are also applicable to the orientation and mobility specialist Programs:
- Code of Federal Regulations (CFR)
- 42 CFR 441 Subpart B
- Montana Code Annotated (MCA)
- MCA 53-6-101
- Administrative Rules of Montana (ARM)
- ARM 37.86.2201–37.86.2235
Claims Review (MCA 53-6-111, ARM 37.85.406)
The Department is committed to paying Montana Healthcare programs providers’ claims as quickly as possible. Montana Healthcare programs claims are electronically processed and usually are not reviewed by medical experts prior to payment to determine if the services provided were appropriately billed. Although the computerized system can detect and deny some erroneous claims, there are many erroneous claims which it cannot detect. For this reason, payment of a claim does not mean that the service was correctly billed or the payment made to the provider was correct. The Department performs periodic retrospective reviews, which may lead to the discovery of incorrect billing or incorrect payment. If a claim is paid, and the Department later discovers that the service was incorrectly billed or paid or the claim was erroneous in some other way, the Department is required by federal regulation to recover any overpayment, regardless of whether the incorrect payment was the result of Department or provider error or other cause.
Getting Questions Answered
The provider manuals are designed to answer most questions; however, questions may arise that require a call to a specific group (such as a prior authorization contractor or Provider Relations). The list of Key Contacts at the front of this manual has important phone numbers and addresses pertaining to this manual. The Introduction chapter in the General Information for Providers manual also has a list of contacts for specific Programs policy information. Montana Healthcare programs manuals, provider notices, replacement pages, fee schedules, forms, and much more are available on the Provider Information website (See Key Websites).
Other Department programs
The Montana Healthcare programs orientation and mobility specialist services in this manual are not benefits of the Mental Health Services Plan (MHSP), so the information in this manual does not apply to MHSP. For more information on MHSP, see the mental health manual available on the Provider Information website (See Key Websites).
The Montana Healthcare programs orientation and mobility specialist services in this manual are not covered benefits of Healthy Montana Kids (HMK). Additional information regarding HMK benefits is available by contacting Blue Cross and Blue Shield of Montana at 1 (800) 447-7828, or by visiting the HMK website (See Key Websites).
End of Introduction Chapter
Covered Services
General Coverage Principles
This chapter provides covered services information that applies specifically to services provided by orientation and mobility specialists. Like all health care services received by Montana Healthcare Programs members, services rendered by these providers must also meet the general requirements listed in the General Information for Providers manual, Provider Requirements chapter.
Services within Scope of Practice (ARM 37.86.2235)
Services are covered only when they are within the scope of the provider’s certification. As a condition of participation in the Montana Healthcare Program all providers must comply with all applicable state and federal statutes, rules and regulations, including but not limited to federal regulations and statutes found in Title 42 of the Code of Federal Regulations and the United States Code governing the Montana Healthcare Program and all applicable Montana statutes and rules governing licensure and certification.
Certification
A provider of EPSDT blind and low vision services, or orientation and mobility specialist, must be certified in accordance with the established organizations outlined in ARM 37.86.2235. These include the Academy for Certification of Vision Rehabilitation and Education Professionals (ACVREP) or a National Orientation and Mobility Certification (NOMC) offered by the National Blindness Professional Certification Board (NBPCB).
EPSDT (ARM 37.86.2201–2235)
The Early and Periodic Screening, Diagnosis, and Treatment (EPSDT) program is a comprehensive approach to health care for Montana Healthcare Programs members under age 21. It is designed to prevent, identify, and then treat health problems before they become disabling. Under EPSDT, Montana Healthcare Programs-eligible children may receive any medically necessary covered service, including all orientation and mobility specialist services described in this manual.
Noncovered Services (ARM 37.85.207)
Montana Healthcare Programs does not cover the following services:
- Services provided to Montana Healthcare Programs members who are absent from the state, with the following exceptions:
- Medical emergency;
- Required medical services are not available in Montana. Prior authorization may be required; see the fee schedule on the provider type page of the website.
- If the Department has determined that the general practice for members in a particular area of Montana is to use providers in another state;
- When out-of-state medical services and all related expenses are less costly than in-state services; or
- When Montana makes adoption assistance or foster care maintenance payments for a member who is a child residing in another state.
Coverage of Specific Services
EPSDT blind and low vision services are included as a component under the EPSDT program.
Children with blind or low vision problems may be referred to a certified orientation and mobility specialist for services. The Montana Healthcare Programs blind and low vision services program covers the following services for children under age 21 through the EPSDT program:
- Assessment of the child’s visual status
- Children with blind or low vision needs may be referred to a certified orientation and mobility specialist for services.
- The Montana Healthcare Programs EPSDT blind and low vision services program covers these services for children:
- Sensory integrative techniques to enhance sensory processing and promote adaptive responses to environmental demands.
- Self-care/home management training in activities of daily living (ADLs), instruction in use of assistive/adaptive equipment.
Verifying Coverage
The easiest way to verify coverage for a specific service is to check the Department’s fee schedule for your provider type. In addition to being listed on the fee schedule, all services provided must also meet the coverage criteria listed in this chapter and in the Provider Requirements chapter of the General Information for Providers manual.
Use the fee schedule in conjunction with the more detailed coding descriptions listed in the current CPT and HCPCS coding books. Fee schedules are available on your provider type page on the Provider Information website (See Key Websites).
End of Covered Services Chapter
Passport and Prior Authorization
What Is Passport to Health? (ARM 37.86.5101–5120, ARM 37.86.5303, and ARM 37.86.5201–5206)
Passport to Health is the managed care program for Montana Healthcare Programs and Healthy Montana Kids (HMK) Plus members. The four Passport programs encourage and support Montana Healthcare Programs and HMK Plus members and providers in establishing a medical home and in ensuring the appropriate use of Montana Healthcare Programs and HMK Plus services:
- Passport to Health Primary Care Case Management
- Team Care
Montana Healthcare Programs does not pay for services when prior authorization or Passport requirements are not met.
Montana Healthcare Programs and HMK Plus members who are eligible for Passport must enroll in the program (about 70% of Montana Healthcare Programs and HMK Plus members are eligible). Each enrollee has a designated Passport provider who is typically a physician, midlevel practitioner, or primary care clinic.
Passport to Health Primary Care Case Management (ARM 37.86.5101–5120)
The Passport provider provides primary care case management (PCCM) services to their members. This means he/she provides or coordinates the member’s care and makes referrals to other Montana Healthcare Programs and HMK Plus providers when necessary. Under Passport, Montana Healthcare Programs and HMK Plus members choose one primary care provider (PCP) and develop an ongoing relationship that provides a medical home. The medical home is a concept that encourages a strong doctor-member relationship. An effective medical home is accessible, continuous, comprehensive, coordinated, and operates within the context of family and community.
With some exceptions, all services to Passport members must be provided or approved by the member’s Passport provider or Montana Healthcare Programs/HMK Plus will not reimburse for those services. (See Services That Do Not Require Passport Approval later in this chapter.) The member’s Passport provider is also referred to as the PCP.
Different codes are issued for Passport approval and prior authorization, and both must be recorded on the claim form.
Team Care (ARM 37.86.5303)
Team Care is designed to educate members to effectively access medical care. Members with a history of using services at an amount or frequency that is not medically necessary are enrolled in Team Care. Members enrolled in Team Care are also enrolled in Passport. Team Care follows the same Passport rules and guidelines for referrals, enrollment/disenrollment, prior authorization, and billing processes. However, while Passport members can change providers without cause, as often as once a month, Team Care members are locked in to one provider and one pharmacy. Providers are encouraged to make a referral to the Team Care Program Officer if they feel one of their members is appropriate for the program. A Passport provider receives an enhanced case management fee of $6 per member per month for Team Care members. When checking Montana Healthcare Programs or HMK Plus eligibility on the MATH web portal (See Key Websites). A Team Care member’s provider and pharmacy will be listed. Write all Montana Healthcare Programs and HMK Plus prescriptions to the designated pharmacy.
In practice, providers will most often encounter Montana Healthcare Programs and HMK Plus members who are enrolled in Passport. Specific services may also require prior authorization (PA) even if the member is a Passport enrollee. Passport referral and approval requirements and PA requirements are described in the General Information for Providers manual. Specific PA requirements can be found in the provider fee schedules.
Prior Authorization
Orientation and mobility specialist services that are a covered service of Montana Healthcare Programs generally do not require prior authorization. Refer to the Montana Healthcare Programs fee schedule for your provider type for PA requirements.
End of Passport and Prior Authorization Chapter
Coordination of Benefits
When Members Have Other Coverage
Montana Healthcare Programs members often have coverage through Medicare, workers’ compensation, employment-based coverage, individually purchased coverage, etc. Coordination of benefits is the process of determining which source of coverage is the primary payer in a particular situation. In general, providers should bill other carriers before billing Montana Healthcare Programs, but there are some exceptions (See the Exceptions to Billing Third Party First section in this chapter). Medicare is processed differently than other sources of coverage.
Identifying Additional Coverage
The member’s Montana Healthcare Programs eligibility verification may identify other payers such as Medicare or other third party payers. (See the General Information for Providers manual, Member Eligibility and Responsibilities chapter.) If a member has Medicare, the Medicare ID number is provided. If a member has additional coverage, the carrier is shown. Some examples of third party payers include:
- Private health insurance
- Employment-related health insurance
- Workers’ compensation insurance*
- Health insurance from an absent parent
- Automobile insurance*
- Court judgments and settlements*
- Long-term care insurance
*These third party payers (and others) may not be listed on the member’s Montana Healthcare Programs eligibility verification.
Providers should use the same procedures for locating third party sources for Montana Healthcare Programs members as for their non-Montana Healthcare Programs members. Providers cannot refuse service because of a third party payer or potential third party payer.
When a Member Has Medicare
Medicare claims are processed and paid differently than other non-Montana Healthcare Programs claims. The other sources of coverage are called third party liability or TPL, but Medicare is not.
Medicare Part B Crossover Claims
Orientation and mobility specialist services may be covered under Medicare Part B. The Department has an agreement with the Medicare Part B carrier for Montana (Noridian) and the Durable Medical Equipment Regional Carrier [DMERC]) under which the carriers provide the Department with claims for members who have both Medicare and Montana Healthcare Programs coverage. Providers must tell Medicare that they want their claims sent to Montana Healthcare Programs automatically, and must have their Medicare provider number on file with Montana Healthcare Programs.
To avoid confusion and paperwork, submit Medicare Part B crossover claims to Montana Healthcare Programs only when necessary.
When members have both Medicare and Montana Healthcare Programs covered claims, and have made arrangements with both Medicare and Montana Healthcare Programs, Part B services need not be submitted to Montana Healthcare Programs. When a crossover claim is submitted only to Medicare, Medicare will process the claim, submit it to Montana Healthcare Programs, and send the provider an Explanation of Medicare Benefits (EOMB). Providers must check the EOMB for the statement indicating that the claim has been referred to Montana Healthcare Programs for further processing. It is the provider’s responsibility to follow up on crossover claims and make sure they are correctly billed to Montana Healthcare Programs within the timely filing limit (See the Billing Procedures chapter in this manual).
All Part B crossover claims submitted to Montana Healthcare Programs before the 45-day Medicare response time will be returned to the provider.
Providers should submit Medicare crossover claims to Montana Healthcare Programs only when:
- The referral to Montana Healthcare Programs statement is missing. In this case, submit a claim and a copy of the Medicare EOMB to Montana Healthcare Programs for processing.
- The referral to Montana Healthcare Programs statement is present, but the provider does not hear from Montana Healthcare Programs within 45 days of receiving the Medicare EOMB. Submit a claim and a copy of the Medicare EOMB to Montana Healthcare Programs for processing.
- Medicare denies the claim, you may submit the claim to Montana Healthcare Programs with the EOMB and denial explanation (as long as the claim has not automatically crossed over from Medicare).
When submitting electronic claims with paper attachments, see the Billing Electronically with Paper Attachments section of the Submitting a Claim chapter in this manual.
When submitting a Medicare crossover claim to Montana Healthcare Programs, use Montana Healthcare Programs billing instructions and codes; they may not be the same as Medicare’s.
When submitting a claim with the Medicare EOMB, use Montana Healthcare Programs billing instructions and codes. Medicare’s instructions, codes, and modifiers may not be the same as Montana Healthcare Programs’s. The claim must also include the Montana Healthcare Programs provider number and Montana Healthcare Programs member ID number. It is the provider’s responsibility to follow up on crossover claims and make sure they are correctly billed to Montana Healthcare Programs within the timely filing limit (See the Billing Procedures chapter in this manual).
When a Member Has TPL (ARM 37.85.407)
When a Montana Healthcare Programs member has additional medical coverage (other than Medicare), it is often referred to as third party liability or TPL. In most cases, providers must bill other insurance carriers before billing Montana Healthcare Programs.
Providers are required to notify their members that any funds the member receives from third party payers (when the services were billed to Montana Healthcare Programs) must be turned over to the Department. The following words printed on the member’s statement will fulfill this obligation: “When services are covered by Montana Healthcare Programs and another source, any payment the member receives from the other source must be turned over to Montana Healthcare Programs.”
Exceptions to Billing Third Party First
In a few cases, providers may bill Montana Healthcare Programs first:
- When a Montana Healthcare Programs member is also covered by Indian Health Service (IHS) or Crime Victim Compensation, providers must bill Montana Healthcare Programs first. These are not considered a third party liability.
- When a member has Montana Healthcare Programs eligibility and Mental Health Services Plan (MHSP) eligibility for the same month, Montana Healthcare Programs must be billed before MHSP.
- If the third party has only potential liability, such as automobile insurance, the provider may bill Montana Healthcare Programs first. Do not indicate the potential third party on the claim. Instead, notify the Department of the potential third party by sending the claim and notification directly to the Third Party Liability Unit (See Key Contacts).
Requesting an Exemption
Providers may request to bill Montana Healthcare Programs first under certain circumstances. In each of these cases, the claim and required information should be sent directly to the Third Party Liability Unit (See Key Contacts).
- When a provider is unable to obtain a valid assignment of benefits, the provider should submit the claim with documentation that the provider attempted to obtain assignment and certification that the attempt was unsuccessful.
- When the provider has billed the third party insurance and has received a non-specific denial (e.g., no member name, date of service, amount billed), submit the claim with a copy of the denial and a letter of explanation.
- When the Child Support Enforcement Division has required an absent parent to have insurance on a child, the claim can be submitted to Montana Healthcare Programs when the following requirements are met:
- The third party carrier has been billed, and 30 days or more have passed since the date of service.
- The claim is accompanied by a certification that the claim was billed to the third party carrier, and payment or denial has not been received.
- If another insurance has been billed, and 90 days have passed with no response, submit the claim with a note explaining that the insurance company has been billed, or attach a copy of the letter sent to the insurance company. Include the date the claim was submitted to the insurance company and certification that there has been no response.
When the Third Party Pays or Denies a Service
When a third party payer is involved (excluding Medicare) and the other payer:
- Pays the claim, indicate the amount paid when submitting the claim to Montana Healthcare Programs for processing.
- Allows the claim, and the allowed amount went toward the member’s deductible, include the insurance explanation of benefits (EOB) when billing Montana Healthcare Programs.
- Denies the claim, submit the claim and a copy of the denial (including the reason explanation) to Montana Healthcare Programs.
- Denies a line on the claim, bill the denied line on a separate claim and submit to Montana Healthcare Programs. Include the EOB from the other payer as well as an explanation of the reason for denial (e.g., definition of denial codes).
If the provider receives a payment from a third party after the Department has paid the provider, the provider must return the lower of the two payments to the Department within 60 days.
When the Third Party Does Not Respond
If another insurance has been billed, and 90 days have passed with no response, bill Montana Healthcare Programs as follows:
- Submit the claim and a note explaining that the insurance company has been billed, or attach a copy of the letter sent to the insurance company.
- Include the date the claim was submitted to the insurance company.
- Send this information to the Third Party Liability Unit (See Key Contacts).
End of Coordination of Benefits Chapter
Billing Procedures
Claim Forms
Services provided by orientation and mobility specialist services providers must be billed either electronically or on a CMS-1500 claim form. CMS-1500 forms are available from various publishing companies; they are not available from the Department or Provider Relations.
Timely Filing Limits (ARM 37.85.406)
Providers must submit clean claims to Montana Healthcare Programs within:
- Twelve months from whichever is later:
- the date of service
- the date retroactive eligibility or disability is determined
- For claims involving Medicare or TPL, if the 12-month time limit has passed, providers must submit clean claims to Montana Healthcare Programs:
- Medicare crossover claims: Six months from the date on the Medicare explanation of benefits approving the service (if the Medicare claim was timely filed and the member was eligible for Medicare at the time the Medicare claim was filed).
- Claims involving other third party payers (excluding Medicare): Six months from the date on an adjustment notice from a third party payer who has previously processed the claim for the same service, and the adjustment notice is dated after the periods described above.
Clean claims are claims that can be processed without additional information or action from the provider. All problems with claims must be resolved within this 12-month period.
Tips to Avoid Timely Filing Denials
- Correct and resubmit denied claims promptly (See the Remittance Advices and Adjustments chapter in this manual).
- If a claim submitted to Montana Healthcare Programs does not appear on the remittance advice within 30 days, contact Provider Relations for claim status (See Key Contacts).
- If another insurer has been billed and 90 days have passed with no response, you can bill Montana Healthcare Programs (See the Coordination of Benefits chapter in this manual for more information).
- To meet timely filing requirements for Medicare/Montana Healthcare Programs crossover claims, see the Coordination of Benefits chapter in this manual.
When to Bill Montana Healthcare Programs Members (ARM 37.85.406)
In most circumstances, providers may not bill Montana Healthcare Programs members for services covered under Montana Healthcare Programs. T
More specifically, providers cannot bill members directly:
- For the difference between charges and the amount Montana Healthcare Programs paid.
- When the provider bills Montana Healthcare Programs for a covered service, and Montana Healthcare Programs denies the claim because of billing errors.
- When a third party payer does not respond.
- When a member fails to arrive for a scheduled appointment. Montana Healthcare Programs may not be billed for no-show appointments.
- When services are free to the member. Montana Healthcare Programs may not be billed for those services either.
Under certain circumstances, providers may need a signed agreement in order to bill a Montana Healthcare Programs member (see the following table).

If a provider bills Montana Healthcare Programs and the claim is denied because the member is not eligible, the provider may bill the member directly.
Routine Agreement: This may be a routine agreement between the provider and member which states that the member is not accepted as a Montana Healthcare Programs member, and then he/she must pay for the services received.
Custom Agreement: This agreement lists the service the member is receiving and states that the service is not covered by Montana Healthcare Programs and that the member will pay for it.
When Members Have Other Insurance
If a Montana Healthcare Programs member is also covered by Medicare, has other insurance, or some other third party is responsible for the cost of the member’s health care, see the Coordination of Benefits chapter in this manual.
Billing for Retroactively Eligible Members
When a member becomes retroactively eligible for Montana Healthcare Programs, the provider has 12 months from the date retroactive eligibility was determined to bill for those services. When submitting claims for retroactively eligible members, attach a copy of the FA-455 (eligibility determination letter) to the claim if the date of service is more than 12 months earlier than the date the claim is submitted.
When a provider chooses to accept the member from the date retroactive eligibility was effective, and the member has made a full or partial payment for services, the provider must refund the member’s payment for the services before billing Montana Healthcare Programs for the services.
For more information on retroactive eligibility, see the General Information for Providers manual, Member Eligibility and Responsibilities chapter.
Usual and Customary Charge (ARM 37.85.406)
Providers should bill Montana Healthcare Programs their usual and customary charge for each service; that is, the same charge that is made to other payers for that service.
Coding
Standard use of medical coding conventions is required when billing Montana Healthcare Programs. Provider Relations or the Department cannot suggest specific codes to be used in billing for services. For coding assistance and resources, see the Coding Resources table on the following page. The following suggestions may help reduce coding errors and unnecessary claim denials:
- Use current CPT, HCPCS, and ICD coding books.
- Always read the complete description and guidelines in the coding books. Relying on short descriptions can result in inappropriate billing.
- Attend classes on coding offered by certified coding specialists.
- Use the correct units measurement on the claim.
Coding Resources
Please note that the Department does not endorse the products of any particular publisher.
CPT
Description:
CPT codes and definitions.
Updated each January.
Contact:
American Medical Association
(800) 621-8335
https://commerce.ama-assn.org/store/
CPT Assistant
Description:
A newsletter on CPT coding issues.
Contacts:
American Medical Association
(800) 621-8335
https://commerce.ama-assn.org/store/
HCPCS Level II
Description:
HCPCS codes and definitions.
Updated each January and throughout the year.
Contact:
Available through various publishers and bookstores or from CMS at www.cms.gov.
ICD
Description:
ICD diagnosis and procedure code definitions.
Updated each October.
Contact:
Available through various publishers and bookstores.
Miscellaneous
Various newsletters and other coding resources are available in the commercial marketplace.
NCCI Policy and Edits Manual
Description:
Contains National Correct Coding Initiative (NCCI) policy and edits, which are pairs of CPT or HCPCS codes that are not separately payable except under certain circumstances. The edits are applied to services billed by the same provider for the same member on the same date of service.
Contact:
National Technical Information Service
(800) 363-2068
(703) 605-6060
https://www.cms.gov/Medicare/Coding/NationalCorrectCodInitEd/index.html
Using the Montana Healthcare Programs Fee Schedule
When billing Montana Healthcare Programs, it is important to use the Department’s fee schedule for your provider type in conjunction with the detailed coding descriptions listed in the current CPT and HCPCS coding books.
In addition to covered services and payment rates, fee schedules often contain helpful information such as appropriate modifiers and prior authorization indicators. Department fee schedules are updated each January and July. Fee schedules are available on the provider type pages on the Provider Information website.
Using Modifiers
- Review the guidelines for using modifiers in the CPT, HCPCS, or other helpful resources.
- Always read the complete description for each modifier; some modifiers are described in the CPT manual while others are in the HCPCS book.
- The Montana Healthcare Programs claims processing system recognizes three pricing modifiers and one informational modifier per claim line. Providers are asked to place any modifiers that affect pricing in the first three modifier fields.
- Modifier 52 must be used when billing for a partial EPSDT well-child screen.
Billing Tips for Specific Providers
Orientation and Mobility Specialist Services
Montana Healthcare Programs reimburses orientation and mobility specialist services in 15-minute units. Four units equal one hour of service. Montana Healthcare Programs will pay up to the rate on the fee schedule for each unit of service billed in the Days or Units field of the claim form. Montana Healthcare Programs will not reimburse for two services that duplicate one another on the same day.
The Most Common Billing Errors and How to Avoid Them
Paper claims are often returned to the provider before they can be processed, and many other claims (both paper and electronic) are denied. To avoid unnecessary returns and denials, double-check each claim to confirm the following items are included and are accurate.
Common Billing Errors
Reasons for Returns or Denials:
Provider’s NPI and/or taxonomy missing or invalid
How to Prevent Returned or Denied Claims:
The provider number is a 10-digit number assigned to the provider during Montana Healthcare Programs enrollment. Verify the correct NPI and taxonomy are on the claim.
Reasons for Returns or Denials:
Authorized signature missing
How to Prevent Returned or Denied Claims:
Each claim must have an authorized signature belonging to the provider, billing clerk, or office personnel. The signature may be typed, stamped, or handwritten.
Reasons for Returns or Denials:
Signature date missing
How to Prevent Returned or Denied Claims:
Each claim must have a signature date.
Reasons for Returns or Denials:
Incorrect claim form used
How to Prevent Returned or Denied Claims:
The claim must be the correct form for the provider type. Services covered in this manual require a CMS-1500 claim form.
Reasons for Returns or Denials:
Information on claim form not legible
How to Prevent Returned or Denied Claims:
Information on the claim form must be legible. Use dark ink and center the information in the field. Information must not be obscured by lines.
Reasons for Returns or Denials:
member number not on file, or member was not eligible on date of service
How to Prevent Returned or Denied Claims:
Before providing services to the member:
- View the member’s eligibility information at each visit; Montana Healthcare Programs eligibility may change monthly.
- Verify member eligibility by using one of the methods described in the member Eligibility and Responsibilities chapter of the General Information for Providers manual.
Reasons for Returns or Denials:
Procedure requires Passport provider referral – No Passport provider number on claim
How to Prevent Returned or Denied Claims:
A Passport provider number must be on the claim form when a referral is required. See the Passport chapter in this manual.
Reasons for Returns or Denials:
Duplicate claim
How to Prevent Returned or Denied Claims:
Check all remittance advices (RAs) for previously submitted claims before resubmitting.
When making changes to previously paid claims, submit an adjustment form rather than a new claim form (see Remittance Advices and Adjustments in this manual).
Allow 45 days for the Medicare/Montana Healthcare Programs Part B crossover claim to appear on the RA before submitting the claim directly to Montana Healthcare Programs.
Reasons for Returns or Denials:
Prior authorization number is missing
How to Prevent Returned or Denied Claims:
Prior authorization (PA) is required for certain services, and the PA number must be on the claim form (see the Prior Authorization chapter in this manual).
Reasons for Returns or Denials:
TPL on file and no credit amount on claim
How to Prevent Returned or Denied Claims:
If the member has any other insurance (or Medicare), bill the other carrier before Montana Healthcare Programs. See the Coordination of Benefits chapter in this manual.
If the member’s TPL coverage has changed, providers must notify the TPL Unit (see Key Contacts) before submitting a claim.
Reasons for Returns or Denials:
Claim past 365-day filing limit
How to Prevent Returned or Denied Claims:
The Claims Processing Unit must receive all clean claims and adjustments within the timely filing limits described in this chapter.
To ensure timely processing, claims and adjustments must be mailed to Claims Processing at the address shown in Key Contacts.
Reasons for Returns or Denials:
Missing Medicare EOMB
How to Prevent Returned or Denied Claims:
All Medicare crossover claims on CMS-1500 forms must have an EOMB attached.
Reasons for Returns or Denials:
Provider is not eligible during dates of services, or provider number terminated
How to Prevent Returned or Denied Claims:
Out-of-state providers must update enrollment early to avoid denials. If enrollment has lapsed, claims submitted with a date of service after the expiration date will be denied until the provider updates his or her enrollment.
New providers cannot bill for services provided before Montana Healthcare Programs enrollment begins.
If a provider is terminated from the Montana Healthcare Programs, claims submitted with a date of service after the termination date will be denied.
Reasons for Returns or Denials:
Type of service/procedure is not allowed for provider type
How to Prevent Returned or Denied Claims:
Provider is not allowed to perform the service.
Verify the procedure code is correct using current HCPCS and CPT billing manuals.
Check the Montana Healthcare Programs fee schedule to verify the procedure code is valid for your provider type.
End of Billing Procedures Chapter
Submitting a Claim
Electronic Claims
Professional and institutional claims submitted electronically are referred to as ANSI ASC X12N 837 transactions. Providers who submit claims electronically experience fewer errors and quicker payment. Claims may be submitted electronically by the following methods:
- WINASAP 5010. This free software is available for providers to create and submit claims to Montana Healthcare Programs, MHSP, and HMK (dental and eyeglasses only) and FQHC/RHC. It does not support submissions to Medicare or other payers, and creates an 837 transaction, but does not accept an 835 transaction back from the Department.
- Conduent EDI Solutions Clearinghouse. Providers can send claims to Conduent EDI Solutions (previously EDI Gateway) clearinghouse in X12 837 format using a dial-up connection. Electronic submitters are required to certify their 837 transactions as HIPAA-compliant before sending their transactions through EDI Solutions. EDIFECS certifies the 837 HIPAA transactions at no cost to the provider. EDIFECS certification is completed through EDI Solutions.
- Clearinghouse. Providers can contract with a clearinghouse and send claims to the clearinghouse in whatever format they accept. The provider's clearinghouse then sends the in the X12 837 format. The provider’s clearinghouse also needs to have their 837 transactions certified through EDIFECS before submitting claims. EDIFECS certification is completed through EDI Solutions. For information on electronic claims submission, contact Provider Relations (See Key Contacts).
- Montana Access to Health (MATH) web portal. Providers can upload and download electronic transactions 7 days a week through the web portal. This availability is subject to scheduled and unscheduled host downtime.
- B2B Gateway SFTP/FTPS site. Providers can use this method to send electronic transactions through this secure FTP process. This is typically encountered with high volume/high-frequency submitters.
- MOVEit DMZ. Providers can use this secure transmission protocol and secure storage landing zone (intermediate storage) for the exchange of files between trading partners and Xerox. Its use is intended for those trading partners/submitters who will be submitting a larger volume of physical files (in excess of 20 per day) or whose physical file sizes regularly exceed 2 MB.
Providers should be familiar with the federal rules and regulations on preparing electronic transactions.
Billing Electronically with Paper Attachments
When submitting claims that require additional supporting documentation, the Attachment Control Number field must be populated with an identifier. Identifier formats can be designed by software vendors or clearinghouses, but the preferred method is the provider’s Montana Healthcare Programs ID number followed by the member’s ID number and the date of service, each separated by a dash:

The supporting documentation must be submitted with a Paperwork Attachment Cover Sheet (See the Forms page of the Provider Information website). The number in the paper Attachment Control Number field must match the number on the cover sheet. For more information on attachment control numbers and submitting electronic claims, contact Provider Relations (See Key Contacts).
Paper Claims
The services described in this manual are billed on CMS-1500 claim forms. Claims submitted with all of the necessary information are referred to as clean and are usually paid in a timely manner. (See the Billing Procedures chapter in this manual.)
Claims are completed differently for the different types of coverage a member has (e.g., Montana Healthcare Programs only, Montana Healthcare Programs and Third Party Liability).
When completing a claim, remember the following:
- Required fields are indicated by “*”.
- Fields that are required if the information is applicable to the situation or member are indicated by “**”.
- Field 24h, EPSDT/Family Planning, is used to override copayment and Passport authorization requirements for certain members or services.
The following are accepted codes:
EPSDT/Family Planning Overrides
Code: 1 member/ Service: EPSDT
Purpose: Overrides some benefit limits for member under age 21.
Code: 2 member/ Service: Family planning
Purpose: Overrides the Montana Healthcare Programs Passport authorization on the line.
Code: 3 member/ Service: EPSDT and family planning
Purpose: Overrides Montana Healthcare Programs cost sharing and Passport authorization for persons under the age of 21.
Code: 5 member/ Service: Nursing facility member
Purpose: Overrides the Medicare edit for oxygen services on the line.
Unless otherwise stated, all paper claims are mailed to:
Claims Processing
P.O. Box 8000
Helena, MT 59604
All Montana Healthcare Programs claims must be submitted on Department approved claim forms. CMS-1500 forms are available from various publishing companies; they are not available from the Department or Provider Relations.
CMS-1500 Agreement
Your signature on the CMS-1500 constitutes your agreement to the terms presented on the back of the form. This form is subject to change by the Centers for Medicare and Medicaid Services (CMS).
Claim Inquiries
Claim inquiries can be obtained electronically through ANSI ASC X12N 276/277 transactions or by contacting Provider Relations. Providers may contact Provider Relations for questions regarding payments, denials, and other claim questions (See Key Contacts).
Avoiding Claim Errors
Claims are often denied or even returned to the provider before they can be processed. To avoid denials and returns, double-check each claim form to confirm the following items are accurate. For more information on returned and denied claims, see the Billing Procedures chapter in this manual.
Common Claim Errors
Claim Error: Required field is blank
Prevention: Check the claim instructions earlier in this chapter for required fields (indicated by * or **). If a required field is blank, the claim may either be returned or denied.
Claim Error: member ID number missing or invalid
Prevention: This is a required field (Field 10d); verify that the member’s Montana Healthcare Programs ID number is listed as it appears on the member’s eligibility information.
Claim Error: member name missing
Prevention: This is a required field (Field 2); check that it is correct.
Claim Error: NPI/API missing or invalid
Prevention: The NPI is a 10-digit number (API is a 7-digit) assigned to the provider. Verify the correct NPI/API is on the claim.
Claim Error: Referring or Passport provider name and ID number missing
Prevention: When a provider refers a member to another provider, include the referring provider’s name and ID number or Passport number (see the Passport chapter in this manual).
Claim Error: Prior authorization number missing
Prevention: When prior authorization (PA) is required for a service, the PA number must be on the claim (see the Prior Authorization chapter in this manual).
Claim Error: Not enough information regarding other coverage
Prevention: Fields 1a and 11d are required fields when a member has other coverage (see examples earlier in this chapter).
Claim Error: Authorized signature missing
Prevention: Each claim must have an authorized signature belonging to the provider, billing clerk, or office personnel. The signature may be typed, stamped, or handwritten.
Claim Error: Signature date missing
Prevention: Each claim must have a signature date.
Claim Error: Incorrect claim form used
Prevention: Services covered in this manual require a CMS-1500 claim form.
Claim Error: Information on claim form not legible
Prevention: Information on the claim form must be legible. Use dark ink and center the information in the field. Information must not be obscured by lines.
Claim Error: Medicare EOMB not attached
Prevention: When Medicare is involved in payment on a claim, the Medicare EOMB must be submitted with the claim or it will be denied.
End of Submitting a Claim Chapter
Remittance Advices and Adjustments
Electronic Remittance Advice
The Remittance Advice (RA) is the best tool providers have for determining the status of a claim. RAs accompany payment for services rendered. Beginning July 1, 2013, new providers were required to register for electronic funds transfer (EFT) and electronic RAs. Existing Montana Healthcare Programs providers will transition to electronic payment and RAs over time.
Providers must complete the EDI Trading Partner Agreement, must have registered for the Montana Access to Health (MATH) web portal, and must have Internet access.
The verification process also requires a provider ID, a submitter ID, and a tax ID number. Each provider must complete a Trading Partner Agreement, but if there are several providers in one location who are under one tax ID number, they can use one submitter number. These providers should enter the submitter ID in both the provider number and submitter ID fields. Otherwise, enter the provider number in the provider number field.
After these forms have been processed, the provider will receive a user ID and password that he/she can use to log onto the MATH web portal.
Electronic RAs are available for only 90 days on the web portal.
RAs are available in PDF format. Providers can read, print, or download PDF files using Adobe Acrobat Reader, which is available on the MATH web portal home page. Due to space limitations, each RA is only available for 90 days. Providers should save/print RAs for later reference.
If a claim was denied, read the reason and remark code description before taking any action on the claim.
The RA is divided into the following sections: RA Notice, Paid Claims, Denied Claims, Pending Claims, Credit Balance Claims, Gross Adjustments, and Reason and Remark Codes/Descriptions.
The RA provides details of all transactions that have occurred during the previous RA cycle. Providers are paid weekly. Each line of the RA represents all or part of a claim and explains whether the claim or service has been paid, denied, or suspended (also referred to as pending). If the claim was suspended or denied, the RA also shows the reason.
The pending claims section of the RA is informational only. Do not take any action on claims shown here.
Credit Balance Claims
Credit balances occur when claim adjustments reduce original payments causing the provider to owe money to the Department. These claims are considered in process and continue to appear on the RA until the credit has been satisfied.
The Credit Balance section is informational only. Do not post from credit balance statements.
Credit balances can be resolved in two ways:
- By working off the credit balance. Remaining credit balances can be deducted from future claims. These claims will continue to appear on consecutive RAs until the credit has been paid.
- By sending a check payable to DPHHS for the amount owed. This method is required for providers who no longer submit claims to Montana Healthcare Programs. Attach a note stating that the check is to pay off a credit balance and include your provider number. Send the check to the attention of the Third Party Liability address in Key Contacts.
Rebilling and Adjustments
Rebillings and adjustments are important steps in correcting any billing problems you may experience. Knowing when to use the rebilling process versus the adjustment process is important.
Montana Healthcare Programs does not accept any claim for resubmission or adjustment after 12 months from the date of service. (See Timely Filing Limits in the Billing Procedures chapter.)
Timeframe for Rebilling or Adjusting a Claim
- Providers may resubmit, modify, or adjust any initial claim within the timely filing limits described in the Billing Procedures chapter of this manual.
- The time periods do not apply to overpayments that the provider must refund to the Department. After the 12-month time period, a provider may not refund overpayments to the Department by completing a claim adjustment. The provider may refund overpayments by issuing a check, or request Provider Relations to complete a gross adjustment.
Rebilling Montana Healthcare Programs
Rebilling is when a provider submits a claim to Montana Healthcare Programs that was previously submitted for payment but was either returned or denied. Claims are often returned to the provider before processing because key information such as Montana Healthcare Programs provider number or authorized signature and date are missing or unreadable. For tips on preventing returned or denied claims, see the Billing Procedures chapter in this manual.
When to Rebill Montana Healthcare Programs
- Claim Denied. Providers may rebill Montana Healthcare Programs when a claim is denied. Check the Reason and Remark Codes, make the appropriate corrections, and resubmit the claim. Do not use and adjustment form.
- Line denied. When an individual line is denied on a multiple-line claim, correct any errors and submit only the denied line to Montana Healthcare Programs. For CMS-1500 claims, do not use an adjustment form.
- Claim returned. Rebill Montana Healthcare Programs when the claim is returned under separate cover. Occasionally, Montana Healthcare Programs is unable to process the claim and will return it to the provider with a letter stating that additional information is needed to process the claim. Correct the information as directed and resubmit the claim.
How to Rebill
- Check any Reason and Remark Code listed and make corrections on a copy of the claim, or produce a new claim with the correct information.
- When making corrections on a copy of the claim, remember to line out or omit all lines that have already been paid.
- Submit insurance information with the corrected claim.
Rebill denied claims only after appropriate corrections have been made.
Adjustments
If a provider believes that a claim has been paid incorrectly, the provider may call Provider Relations. Once an incorrect payment has been verified, the provider should submit an Individual Adjustment Request form to Provider Relations. If incorrect payment was the result of a Conduent Services keying error, contact Provider Relations.
When adjustments are made to previously paid claims, the Department recovers the original payment and issues appropriate repayment. The result of the adjustment appears on the provider’s RA as two transactions. The original payment will appear as a credit transaction. The replacement claim reflecting the corrections will be listed as a separate transaction and may or may not appear on the same RA as the credit transaction. The replacement transaction will have nearly the same ICN number as the credit transaction, except the 12th digit over will be a 2, indicating an adjustment. Adjustments are processed in the same time frame as claims.
When to Request an Adjustment
- Request an adjustment when the claim was overpaid or underpaid.
- Request an adjustment when the claim was paid but the information on the claim was incorrect (e.g., member ID, provider number, date of service, procedure code, diagnoses, units).
How to Request an Adjustment
To request an adjustment, download the Montana Health Care Programs Individual Adjustment Request form from the Provider Information website. A copy is also in Appendix A: Forms. The requirements for adjusting a claim are as follows:
- Adjustments can only be submitted on paid claims; denied claims cannot be adjusted.
- Claims Processing must receive individual claim adjustments within 12 months from the date of service. (See Timely Filing in the Billing Procedures chapter of this manual.) After this time, gross adjustments are required (see the Definitions and Acronyms chapter).
- Use a separate adjustment request form for each ICN.
- If you are correcting more than one error per ICN, use only one adjustment request form, and include each error on the form.
- If more than one line of the claim needs to be adjusted, indicate which lines and items need to be adjusted in the Reason and Remarks section.
Completing an Adjustment Request Form
- Download the Individual Adjustment Request form from the Provider Information website. Complete Section A first with provider and member information and the claim’s ICN number (see following table).
- Complete Section B with information about the claim. Remember to fill in only the items that need to be corrected (see following table):
- Enter the date of service or the line number in the Date of Service or Line Number column.
- Enter the information from the claim form that was incorrect in the Information on Statement column.
- Enter the correct information in the column labeled Corrected Information.
- Attach copies of the RA and a corrected claim if necessary.
- If the original claim was billed electronically, a copy of the RA will suffice.
- If the RA is electronic, attach a screen print of the RA.
- Verify the adjustment request has been signed and dated.
- Send the adjustment request to Claims Processing (See Key Contacts).
Completing an Individual Adjustment Request Form
Section A
Field: 1. Provider Name and Address
Description: Provider’s name and address (and mailing address if different).
Field: 2. Recipient Name
Description: The member’s name.
Field: 3.* Internal Control Number (ICN)
Description: There can be only one ICN per Adjustment Request form. When adjusting a claim that has been previously adjusted, use the ICN of the most recent claim.
Field: 4*. Provider number
Description: The provider’s Montana Healthcare Programs ID number.
Field: 5*. Recipient Montana Healthcare Programs Number
Description: member’s Montana Healthcare Programs ID number.
Field: 6. Date of Payment
Description: Date claim was paid found on Remittance Advice Field 5 (see the sample RA earlier in this chapter).
Field: 7. Amount of Payment
Description: The amount of payment from the Remittance Advice Field 19 (see the sample RA earlier in this chapter.).
Section B
Field: 1. Units of Service
Description: If a payment error was caused by an incorrect number of units, complete this line.
Field: 2. Procedure Code/NDC/Revenue Code
Description: If the procedure code, NDC, or revenue code are incorrect, complete this line.
Field: 3. Dates of Service (DOS)
Description: If the date of service is incorrect, complete this line.
Field: 4. Billed Amount
Description: If the billed amount is incorrect, complete this line.
Field: 5. Personal Resource (Nursing Facility)
Description: If the member’s personal resource amount is incorrect, complete this line.
Field: 6. Insurance Credit Amount
Description: If the member’s insurance credit amount is incorrect, complete this line.
Field: 7. Net (Billed - TPL or Medicare Paid)
Description: If the payment error was caused by a missing or incorrect insurance credit, complete this line. Net is billed amount minus the amount TPL or Medicare paid.
Field: 8. Other/Remarks
Description: If none of the above items apply, or if you are unsure what caused the payment error, complete this line.
*Indicates a required field
- If an original payment was an underpayment by Montana Healthcare Programs, the adjustment results in the provider receiving the additional payment amount allowed.
- If an original payment was an overpayment by Montana Healthcare Programs, the adjustment results in recovery of the overpaid amount from the provider. This can be done in 2 ways: by the provider issuing a check to the Department or by maintaining a credit balance until it has been satisfied with future claims (See Credit Balance in this chapter).
- Any questions regarding claims or adjustments should be directed to Provider Relations (See Key Contacts).
Mass Adjustments
Mass adjustments are done when it is necessary to reprocess multiple claims. They generally occur when:
- Montana Healthcare Programs has a change of policy or fees that is retroactive. In this case federal laws require claims affected by the changes to be mass adjusted.
- A system error that affected claims processing is identified.
Providers are informed of mass adjustments on the first page of the remittance advice (RA Notice section), the monthly Claim Jumper newsletter, or provider notice. Mass adjustment claims shown on the RA have an ICN that begins with a 4.
Payment and the RA
Providers receive their Montana Healthcare Programs payment via electronic funds transfer (EFT) their remittance advice electronically. Direct deposit is another name for EFT. To participate in EFT, providers must complete a Direct Deposit Sign-Up Form (Standard Form 1199A) (see the following table). One form must be completed for each provider number.
With EFT, the Department deposits the funds directly to the provider’s bank account. If the scheduled deposit day is a holiday, funds will be available on the next business day. Electronic RAs will also be available the next business day.
Once electronic transfer testing shows payment to the provider’s account, all Montana Healthcare Programs payments will be made through EFT (See Direct Deposit Arrangements under Key Contacts).
End of Remittance Advices and Adjustments Chapter
How Payment Is Calculated
Overview
Though providers do not need the information in this chapter in order to submit claims to the Department, the information allows providers to understand how payment is calculated and to predict approximate payment for particular claims. These examples are for July 2013 and these rates may not apply at other times.
How Payment is Calculated on TPL Claims
When a member has coverage from both Montana Healthcare Programs and another insurance company, the other insurance company is often referred to as third party liability or TPL. In these cases, the other insurance is the primary payer (as described in the Coordination of Benefits chapter in this manual), and Montana Healthcare Programs makes a payment as the secondary payer. For example, a member receives one visit of EPSDT orientation and mobility services (97533). The third party insurance is billed first and pays $15.00. The Montana Healthcare Programs allowed amount for this service totals $29.21. The amount the insurance paid ($15.00) is subtracted from the Montana Healthcare Programs allowed amount ($29.21), leaving a balance of $14.21, which Montana Healthcare Programs will pay on this claim.
Many Montana Healthcare Programs payment methods are based on Medicare, but there are differences. In these cases, the Montana Healthcare Programs method prevails.
How Payment is Calculated on Medicare Crossover Claims
When a member has coverage from both Montana Healthcare Programs and Medicare, Medicare is the primary payer as described in the Coordination of Benefits chapter of this manual. Montana Healthcare Programs then makes a payment as the secondary payer. For the provider types covered in this manual, Montana Healthcare Programs’s payment is calculated so that the total payment to the provider is either the Montana Healthcare Programs allowed amount less the Medicare paid amount or the sum of the Medicare coinsurance and deductible, whichever is lower. This method is sometimes called “lower of” pricing.
Other Factors That May Affect Payment
When Montana Healthcare Programs payment differs from the fee schedule, consider the following:
- The Department pays the lower of the established Montana Healthcare Programs fee or the provider’s charge
- The member may have an incurment amount that must be met before Montana Healthcare Programs will pay for services. (See the General Information for Providers manual, Member Eligibility and Responsibilities chapter, Coverage for the Medically Needy section.)
- Date of service; fees for services may change over time.
- Cost sharing, Medicare, and/or TPL payments, which are shown on the remittance advice.
End of How Payment Is Calculated Chapter
Appendix A: Forms
- Montana Health Care Programs Medicaid/MHSP/HMK Individual Adjustment Request
- Paperwork Attachment Cover Sheet
End of Appendix A: Forms Chapter
Definitions and Acronyms
This section contains definitions, abbreviations, and acronyms used in this manual.
270/271 Transactions
The X12N eligibility inquiry (270) and response (271) transactions.
276/277 Transactions
The X12N claim status request (276) and response (277) transactions.
278 Transactions
The X12N request for services review and response used for prior authorization.
835 Transactions
The X12N payment and remittance advice (explanation of benefits) transaction.
837 Transactions
The X12N professional, institutional, and dental claim transactions.
Accredited Standards Committee X12, Insurance Subcommittee (ASC X12N)
The ANSI-accredited standards development organization and one of the 6 Designated Standards Maintenance Organizations (DSMO) that created and is tasked with maintaining the administrative and financial transactions standards adopted under HIPAA for all health plans, clearinghouses, and providers who use electronic transactions.
Adjustment
A transaction that changes any payment or other claim information on a previously paid claim.
Administrative Review
Administrative reviews are the Department’s effort to resolve a grievance about a Department decision in order to avoid a hearing. The review includes an informal conference with the Department to review facts, legal authority, and circumstances involved in the adverse action by the Department.
Administrative Rules of Montana (ARM)
The rules published by the executive departments and agencies of the state government.
Assignment of Benefits
A voluntary decision by the member to have insurance benefits paid directly to the provider rather than to the member. The act requires the signing of a form for the purpose. The provider is not obligated to accept an assignment of benefits. However, the provider may require assignment in order to protect the provider’s revenue.
Audit
A formal or periodic verification of accounts.
Authorization
An official approval for action taken for, or on behalf of, a Montana Healthcare Programs member. This approval is only valid if the member is eligible on the date of service.
Basic Montana Healthcare Programs
members with Basic Montana Healthcare Programs have limited Montana Healthcare Programs services. See the General Information for Providers manual, Montana Healthcare Programs Covered Services chapter.
Carrier
A private insurance company.
Centers for Medicare and Medicaid (CMS)
Administers the Medicare program and oversees the state Montana Healthcare Programs s.
Claims Clearinghouse
When a provider contracts with a clearinghouse, the clearinghouse supplies the provider with software that electronically transmits claims to the clearinghouse. The clearinghouse then transmits the claims to the appropriate payers.
Clean Claim
A claim that can be processed without additional information or documentation from or action by the provider of the service.
Coinsurance
The member's financial responsibility for a medical bill as assigned Medicare (usually a percentage). Medicare coinsurance is usually 20% of the Medicare allowed amount.
Cosmetic
Serving to modify or improve the appearance of a physical feature, defect, or irregularity.
Cost Sharing
The member’s financial responsibility for a medical bill assessed by flat fee or percentage of charges.
Credit Balance Claims
Adjusted claims that reduce original payments, causing the provider to owe money to the Department. These claims are considered in process and continue to appear on the remittance advice until the credit has been satisfied.
Crossovers
Claims for members who have both Medicare and Montana Healthcare Programs. These claims may come electronically from Medicare or directly from the provider.
Current Procedural Terminology (CPT)
Physicians’ Current Procedural Terminology contains procedure codes which are used by medical practitioners in billing for services rendered. The book is published by the American Medical Association.
DPHHS, State Agency
The Montana Department of Public Health and Human Services (DPHHS or the Department) is the designated State Agency that administers the Montana Health Care Programs. The Department’s legal authority is contained in Title 53, Chapter 6 MCA. At the federal level, the legal basis for the program is contained in Title XIX of the Social Security Act and Title 42 of the Code of Federal Regulations (CFR). The program is administered in accordance with the Administrative Rules of Montana (ARM), Title 37, Chapter 86.
Early & Periodic Screening, Diagnosis, and Treatment (EPSDT)
This program provides Montana Healthcare Programs-covered children with comprehensive health screenings, diagnostic services, and treatment of health problems.
Electronic Data Interchange (EDI)
The communication of information in a stream of data from one party’s computer system to another party’s computer system.
Electronic Funds Transfer (EFT)
Payment of medical claims that are deposited directly to the provider’s bank account.
Emergency Services
A service is reimbursed as an emergency if one of the following criteria is met: The service is billed with CPT code 99284 or 99285; the member has a qualifying emergency diagnosis code. A list of emergency diagnosis codes is available on the Provider Information website; the services did not meet one of the previous two requirements, but the hospital believes an emergency existed. In this case, the claim and documentation supporting the emergent nature of the service must be mailed to the emergency department review contractor. (See Key Contacts on your provider type page or in your provider manual.)
Explanation of Benefits (EOB) Codes
A 3-digit code which prints on Montana Healthcare Programs remittance advice (RA) that explains why a claim was denied or suspended. The explanation of the EOB codes is found at the end of the RA.
Explanation of Medicare Benefits (EOMB)
A notice sent to providers informing them of the services which have been paid by Medicare.
Fair Hearing
Providers may request a fair hearing when the provider believes the Department’s administrative review determination fails to comply with applicable laws, regulations, rules or policies. Fair hearings include a hearings officer, attorneys, and witnesses for both parties.
Fiscal Agent
Conduent Healthcare LLC, is the fiscal agent for the State of Montana and processes claims at the Department's direction and in accordance with ARM 37.86 et seq.
Full Montana Healthcare Programs
members with Full Montana Healthcare Programs have a full scope of Montana Healthcare Programs benefits. See the General Information for Providers manual, Montana Healthcare Programs Covered Services chapter.
Gross Adjustment
A lump sum debit or credit that is not claim specific made to a provider.
HCPCS
Coding System, and is pronounced “hick-picks.” There are two types of HCPCS codes:
- Level 1 includes the CPT codes.
- Level 2 includes the alphanumeric codes A–V which CMS maintains for a wide range of services from ambulance trips to hearing aids which are not addressed by CPT coding.
Health Improvement Program (HIP)
A service provided under the Passport to Health program for members who have one or more chronic health conditions. Care management focuses on helping members improve their health outcomes through education, help with social services, and coordination with the member’s medical providers.
Health Insurance Portability and Accountability Act (HIPAA)
A federal plan designed to improve efficiency of the health care system by establishing standards for transmission, storage, and handling of data.
Healthy Montana Kids (HMK)
HMK offers low-cost or free health care coverage for low-income children younger than 19. Children must be uninsured U.S. citizens or qualified aliens, Montana residents who are not eligible for Montana Healthcare Programs. DPHHS administers the program with Blue Cross and Blue Shield of Montana (BCBSMT). For eligibility and enrollment information, contact HMK at 1 (877) 543-7669 (toll-free, follow menu) or 1 (855) 258-3489 (toll-free, direct). For information about medical benefits, contact BCBSMT at 1 (406) 447-8647 (Helena) or 1 (800) 447-7828 (toll-free). HMK dental and eyeglasses benefits are provided by DPHHS through the same contractor (Conduent State Healthcare, LLC) that handles Montana Healthcare Programs provider relations and claims processing.
Indian Health Service (IHS)
IHS provides federal health services to American Indians and Alaska Natives.
Internal Control Number (ICN)
The unique number assigned to each claim transaction that is used for tracking.
International Classification of Diseases (ICD)
The International Classification of Diseases contains the diagnosis codes used in coding claims and the procedure codes used in billing for services performed in a hospital setting.
Mass Adjustment
Adjustments made to multiple claims at the same time. They generally occur when the Department has a change of policy or fees that is retroactive, or when a system error that affected claims processing is identified.
Montana Healthcare Programs/HMK Plus
A program that provides health care coverage to specific populations, especially low-income families with children, pregnant women, disabled people and the elderly. Montana Healthcare Programs is administered by state governments under broad federal guidelines.
Medically Necessary
A term describing a requested service which is reasonably calculated to prevent, diagnose, correct, cure, alleviate or prevent worsening of conditions in the member. These conditions must be classified as one of the following: endanger life, cause suffering or pain, result in an illness or infirmity, threaten to cause or aggravate a handicap, or cause physical deformity or malfunction. There must be no other equally effective, more conservative or substantially less costly course of treatment available or suitable for the member requesting the service. For the purpose of this definition, course of treatment may include mere observation or, when appropriate, no treatment at all.
Medicare
The federal health insurance program for certain aged or disabled members.
Member
An individual enrolled in a Department medical assistance program.
Mental Health Services Plan (MHSP)
This plan is for individuals who have a severe disabling mental illness (SDMI), are ineligible for Montana Healthcare Programs, and have a family income that does not exceed an amount established by the Department.
Passport Referral Number
This is a 7-digit number assigned to Passport providers. When a Passport provider refers a member to another provider for services, this number is given to the other provider and is required when processing the claim.
Passport to Health
The Montana Healthcare Programs medical home program where the member selects a primary care provider who manages the member’s health care needs.
Pay-and-Chase
Montana Healthcare Programs pays a claim and then recovers payment from the third party carrier that is financially responsible for all or part of the claim.
Pending Claim
These claims have been entered into the system, but have not reached final disposition. They require either additional review or are waiting for member eligibility information.
Potential Third Party Liability
Any entity that may be liable to pay all or part of the medical cost of care for a Montana Healthcare Programs/HMK Plus, MHSP, or HMK member.
Prior Authorization (PA)
The approval process required before certain services or supplies are paid by Montana Healthcare Programs. Prior authorization must be obtained before providing the service or supply.
Provider or Provider of Service
An institution, agency, or person having a signed agreement with the Department to furnish medical care, goods and/or services to members, and who is eligible to receive payment from the Department.
Qualified Individual
For these members, Montana Healthcare Programs pays the Medicare premium only. They are not eligible for other Montana Healthcare Programs benefits, and they must pay their own Medicare insurance and deductibles.
Qualified Medicare Beneficiary (QMB)
QMB members are members for whom Montana Healthcare Programs pays their Medicare premiums and some or all of their Medicare coinsurance and deductibles.
Rebilling
When a provider submits a claim that was previously submitted for payment but was either returned or denied.
Referral
When providers refer members to other Montana Healthcare Programs providers for medically necessary services that they cannot provide.
Remittance Advice (RA)
The results of claims processing (including paid, denied, and pending claims) are listed on the RA.
Remittance Advice Notice
The first page of the RA that contains important messages for providers.
Retroactive Eligibility
When a member is determined to be eligible for Montana Healthcare Programs effective prior to the current date.
Taxonomy
Taxonomy codes are used to identify and code an external provider table that would be able to standardize provider types and provider areas of specialization for medical-related providers.
Team Care
A restricted services program that is part of Passport to Health. Restricted services programs are designed to assist members in making better health care decisions so that they can avoid overutilizing health services. Team Care members are joined by a team assembled to assist them in accessing health care. The team consists of the member, the PCP, a pharmacy, the Department, and the Department's quality improvement organization. The team may also include a community-based care manager from the Department’s Health Improvement Program.
Third Party Liability (TPL)
Any entity that is liable to pay all or part of the medical cost of care for a Montana Healthcare Programs/HMK Plus, MHSP, or HMK member.
Timely Filing
Providers must submit clean claims (claims that can be processed without additional information or documentation from or action by the provider) to Montana Healthcare Programs within:
- 12 months from whichever is later:
- The date of service.
- The date retroactive eligibility or disability is determined.
- 6 months from the date on the Medicare explanation of benefits approving the service.
- 6 months from the date on an adjustment notice from a third party payer who has previously processed the claim for the same service, and the adjustment notice is dated after the periods described above.
Usual and Customary
The fee that the provider most frequently charges the general public for a service or item.
End of Definitions and Acronyms Chapter
Search Options
Previous editions of this manual contained an index.
This edition has three search options.
- Search the whole manual. Open the Complete Manual pane. From your keyboard press the Ctrl and F keys at the same time. A search box will appear. Type in a descriptive or key word (for example "Denials". The search box will show all locations where denials discussed in the manual.
- Search by Chapter. Open any Chapter tab (for example the "Billing Procedures" tab). From your keyboard press the Ctrl and F keys at the same time. A search box will appear. Type in a descriptive or key word (for example "Denials". The search box will show where denials discussed in just that chapter.
- Site Search. Search the manual as well as other documents related to a particular search term on the Montana Healthcare Programs Site Specific Search page.