Optometric and Eyeglass Services Manual
Printing the manual material found at this website for long-term use is not advisable. Department Policy material is updated periodically and it is the responsibility of the users to check and make sure that the policy they are researching or applying has the correct effective date for their circumstances.
If you experience any difficulty opening a section or link from this page, please email the webmaster.
How to Search this manual:
This edition has three search options.
- Search the whole manual. Open the Complete Manual pane. From your keyboard press the Ctrl and F keys at the same time. A search box will appear. Type in a descriptive or key word (for example "Denials". The search box will show all locations where denials discussed in the manual.
- Search by Chapter. Open any Chapter tab (for example the "Billing Procedures" tab). From your keyboard press the Ctrl and F keys at the same time. A search box will appear. Type in a descriptive or key word (for example "Denials". The search box will show where denials discussed in just that chapter.
- Site Search. Search the manual as well as other documents related to a particular search term on the Montana Healthcare Programs Site Specific Search page.
Prior manuals may be located through the provider website archives.
Updated 04/12/2022
Optometric and Eyeglass Services Manual
To print this manual, right click your mouse and choose "print". Printing the manual material found at this website for long-term use is not advisable. Department Policy material is updated periodically and it is the responsibility of the users to check and make sure that the policy they are researching or applying has the correct effective date for their circumstances.
Update Log
Publication History
This publication supersedes all previous Optometric and Eyeglass Services provider handbooks. Published by the Montana Department of Public Health & Human Services, March 2003.
Updated July 2003, April 2004, January 2005, April 2005, August 2005, October 2005, April 2006, April 2010, May 2010, July 2014, May 2015, January 2016, April 2017,October 2017, March 2018, June 2018, January 2020, and April 2022.
CPT codes, descriptions and other data only are copyright 1999 American Medical Association (or such other date of publication of CPT). All Rights Reserved. Applicable FARS/DFARS Apply.
Update Log
04/12/2022
- Removed Nurse First Advice Line references.
- Updated Index to Search Options.
01/01/2020
- Cost Share references removed from Covered Services, Billing Procedures, and Submitting A Claim Chapters.
- Term "medicaid " replaced with "Montana Healthcare Programs" throughout the manual.
- Terms "client" and "patient" replaced with "member".
06/04/2018
Removed commercial resource references.
03/30/2018
Updated Covered Services and Billing Procedures chapters with new time requirements for services.
10/18/2017
Optometric and Eyeglass Services Manual converted to an HTML format and adapted to 508 Accessibility Standards.
04/10/2017
Optometric and Eyeglass Services, April 2017
In summary, the manual was updated to include current cost share language and co-pays and basic accessibility changes were made as approved by the Manuals Committee in September 2016.
12/31/2015
Optometric and Eyeglass Services, January 2016: HELP Plan-Related Updates and Others
06/24/2015
Optometric and Eyeglass Services, June 2015: Entire Manual
(Note: There are pages that have no text changes; however, the page layout is different than the previous manual due to changes on previous pages.)
08/11/2014
Entire Optometric and Eyeglass Services Manual
Information contained in the General Information for Providers manual or found elsewhere on the website has been removed, and links to those sources are included.
05/19/2010
Key Contacts and Prior Authorization
04/25/2006
Covered Services Information for Initial/New Prescriptions for Eyeglasses
10/12/2005
Covered Services Information for Initial/New Prescriptions
09/09/2005
Eyeglass Service Modifiers, New Place of Service Codes
04/18/2005
Clarification for Lens Add-Ons and Updated Key Contacts
01/19/2005
Rule References Added
04/29/2004
Updates for HIPAA, Covered Services, and Billing Procedures
07/09/2003
Covered Services
End of Update Log Chapter
Table of Contents
Key Websites
Introduction
Manual Organization
Manual Maintenance
Rule References
Claim Review (MCA 53-6-111, ARM 37.85.406)
Getting Questions Answered
Other Department Programs
Covered Services
General Coverage Principles
- Services within scope of practice (ARM 37.85.401)
- Licensing
- Services for children (ARM 37.86.2201 - 2221)
Noncovered Services (ARM 37.85.207)
Coverage of Specific Services
Verifying Coverage
Prior Authorization
Coordination of Benefits
When members Have Other Coverage
Identifying Additional Coverage
When a member Has Medicare
- Medicare Part B crossover claims
When a member Has TPL (ARM 37.85.407)
- Exceptions to billing third party first
- Requesting an exemption
- When the third party pays or denies a service
- When the third party does not respond
Billing Procedures
Claim Forms
Timely Filing Limits (ARM 37.85.406)
- Tips to avoid timely filing denials
When to Bill Montana Healthcare Programs members (ARM 37.85.406)
Member Cost Sharing (ARM 37.85.204)
When members Have Other Insurance
Billing for Retroactively Eligible members
Usual and Customary Charge (ARM 37.85.406)
Coding
Using the Montana Healthcare Programs Fee Schedule
Using Modifiers
The Most Common Billing Errors and How to Avoid Them
Submitting a Claim
Electronic Claims
Billing Electronically with Paper Attachments
Paper Claims
Member Has Montana Healthcare Programs Coverage Only
Member Has Montana Healthcare Programs and Third Party Liability Coverage
CMS-1500 Agreement
Remittance Advices and Adjustments
The Remittance Advice
- Electronic Remittance Advice
- Paper RA
Sample Remittance Advice
- Credit balance claims
Rebilling and Adjustments
- How long do I have to rebill or adjust a claim?
- Rebilling Montana Healthcare Programs
- When to rebill Montana Healthcare Programs
- How to rebill
- Adjustments
- When to request an adjustment
- Completing an Adjustment Request Form
- Mass adjustments
Payment and the RA
How Payment Is Calculated
Overview
How Payment is Calculated on TPL Claims
How Payment is Calculated on Medicare Crossover Claims
Other Factors That May Affect Payment
Appendix A: Forms
Claim Inquiry Form
Individual Adjustment Request
Paperwork Attachment Cover Sheet
Appendix B: Place of Service Codes
Definitions and Acronyms
Index
End of Table of Contents Chapter
Key Contacts
Hours for contacts are 8 a.m. to 5 p.m. Monday through Friday (Mountain Time), unless otherwise stated. The phone numbers designated only “In-state” will not work outside Montana. For additional contacts and a list of key websites, choose the Contact Us link in the left menu on the Provider Information website.
Eyeglass Contractor
Classic Optical Laboratories is contracted with DPHHS to provide eyeglasses to Montana Healthcare Programs members and
HMK members. Providers should call Classic Optical to verify the member is eligible for eyeglasses.
Classic’s contact information is:
Classic Optical Customer Service
3710 Belmont Avenue
P.O. Box 1341 (44501)
Youngstown, OH 44505
(888) 522-2020 Phone
Ext: 1316 - customer service
(888) 522-2022 Fax
HMK Eyeglass Services
HMK Eyeglass Services
P.O. Box 202951
Helena, MT 59620-2951
(877) 543-7669 Toll-free in-state
(406) 444-7045 Phone
(406) 444-1861 Fax
hmk@mt.gov
HMK Optometric Services
Blue Cross and Blue Shield of Montana processes optometric services for HMK members. For more information or a billing manual, contact:
Healthy Montana Kids
Blue Cross and Blue Shield of Montana
P.O. Box 4309
Helena, MT 59604
(800) 447-7828, X8647
(406) 447-8647
Optometric Program Officers
Providers should refer to their specific provider manual for prior authorization instructions.
Contact Montana Provider Relations to verify the member is eligible for eye exams.
Contact DPHHS for prior authorization for transition lenses, tints other than Rose 1 and Rose 2, UV and scratch resistant coating, polycarbonate lenses, and deluxe frames for Montana Healthcare Programs and HMK members
For Montana Healthcare Programs members:
(406) 444-4066 Phone
(406) 444-1861 Fax
Optometric Program Officer
Allied Health Services Bureau
P.O. Box 202951
Helena, MT 59620-2951
For HMK members:
877-543-7669 Toll-free, in-state callers
406-444-7045 Phone
406-444-1861 Fax
hmk@mt.gov
HMK Eyeglass Services
P.O. Box 202951
Helena, MT 59620-2951
End of Key Contacts Chapter
Introduction
Thank you for your willingness to serve members of the Montana Healthcare Program and other medical assistance programs administered by the Department of Public Health and Human Services.
Manual Organization
This manual provides information specifically for optometrists, opticians, and ophthalmologists. Other information for ophthalmologists is included in the Physician-Related Services manual.
Most chapters have a section titled Other Programs that includes information about other Department programs such as the Mental Health Services Plan (MHSP) and the Healthy Montana Kids Program (HMK). Other essential information for providers is contained in the separate General Information for Providers manual. Each provider is asked to review both the general manual and the specific manual for his/her provider type.
A table of contents and an index allow you to quickly find answers to most questions. The margins contain important notes with extra space for writing notes. There is a list of contacts at the beginning of this manual and on the Contact Us page on the Provider Information website. There is space on the inside of the front cover to record your NPI and HMK provider ID numbers for quick reference when calling Provider Relations.
Manual Maintenance
Manuals must be kept current. Changes are provided through provider notices and replacement pages, which are available on the Provider Information website. When replacing a page in a manual, file the old pages in the back of the manual for use with claims that originated under the old policy.
Rule References
Providers must be familiar with all current rules and regulations governing the Montana Healthcare Program. Provider manuals are to assist providers in billing Montana Healthcare Programs; they do not contain all Montana Healthcare Programs rules and regulations. Rule citations in the text are a reference tool; they are not a summary of the entire rule. In the event that a manual conflicts with a rule, the rule prevails. Links to rules are available on the Provider Information website and paper copies of rules are available through the Secretary of State’s office. (See the Contact Us page on the Provider Information website.)
Providers are responsible for knowing and following current Montana Healthcare Programs rules and regulations.
In addition to the Montana Healthcare Programs rules outlined in the General Information for Providers manual, the following rules and regulations are also applicable to the optometric and eyeglass programs:
- Code of Federal Regulations (CFR)
- 42 CFR 440.60 Montana Healthcare Programs or Other Remedial Care Provided by Licensed Practitioners
- 42 CFR 440.120 Prescribed Drugs, Dentures, Prosthetic Devices and Eyeglasses
- Montana Codes Annotated (MCA)
- MCA 37-10-101 through MCA 37-10-313 Optometry
- Administrative Rules of Montana (ARM)
- ARM 37.86.2001 through ARM 37.86.2005 Optometric
- ARM 37.86.2101 through ARM 37.86.2105 Eyeglasses
Claims Review (MCA 53-6-111 and ARM 37.85.406)
The Department is committed to paying Montana Healthcare Programs providers’ claims as quickly as possible. Montana Healthcare Programs claims are electronically processed and usually are not reviewed by medical experts prior to payment to determine if the services provided were appropriately billed. Although the computerized system can detect and deny some erroneous claims, there are many erroneous claims which it cannot detect. For this reason, payment of a claim does not mean that the service was correctly billed or the payment made to the provider was correct. Periodic retrospective reviews are performed which may lead to the discovery of incorrect billing or incorrect payment. If a claim is paid and the Department later discovers that the service was incorrectly billed or paid or the claim was erroneous in some other way, the Department is required by federal regulation to recover any overpayment, regardless of whether the incorrect payment was the result of Department or provider error or other cause.
Getting Questions Answered
The provider manuals are designed to answer most questions; however, questions may arise that require a call to a specific group (such as Provider Relations or a prior authorization unit). The list of at the front of this manual has important phone numbers and addresses pertaining to this manual. Additional contacts and websites are on the Contact Us page of the website. Providers should also read the monthly Claim Jumper newsletter for Montana Healthcare Programs updates and changes. Montana Healthcare Programs provider manuals, provider notices, replacement pages, fee schedules, forms, and more are available on the Provider Information website.
End of Introduction Chapter
Covered Services
General Coverage Principles
This chapter provides covered services information that applies specifically to optometrists, opticians, and ophthalmologists. It also covers information for the prescription of corrective lenses. Like all healthcare services received by Montana Healthcare Programs members, services provided by these practitioners must also meet the general requirements listed in the Provider Requirements chapter of the General Information for Providers manual. Ophthalmologists should also be familiar with the Physician-Related Services manual.
Services within Scope of Practice (ARM 37.85.401 and ARM 37.86.2001)
Services are covered when they are within the scope of the provider’s practice.
Dispensing Services (ARM 37.86.2102)
Dispensing services may be provided by ophthalmologists, optometrists, and opticians. Employees may also dispense if the provider complies with laws, rules, and licensing requirements regarding supervision and assistants or aides.
Services for Members with Limited Montana Healthcare Programs Coverage
Montana Healthcare Programs generally does not cover eye exams or eyeglasses for members with QMB only coverage. Always check member eligibility before providing services. For limits, see the General Information for Providers manual, Member Eligibility chapter; and Eye Exams and Eyeglass Services in this chapter. Montana Healthcare Programs may cover eye exams for members with QMB only coverage under the following conditions.
- Following cataract surgery. Members who have QMB only coverage are only eligible for eyeglasses following cataract surgery when Medicare approves the eyeglasses claim. Montana Healthcare Programs considers the Medicare coinsurance and deductible for this claim. Eyeglasses for these members are not provided through the Department’s eyeglass contractor but through Medicare’s purchasing plan. See the Coordination of Benefits chapter in this manual for more information.
- Diabetic diagnosis. Montana Healthcare Programs covers eye exams once every 365 days for members who have a diabetic diagnosis.
- Some optometric diagnostic conditions may be billed to Montana Healthcare Programs first. In these cases, Montana Healthcare Programs will “pay-and-chase” or recover payment itself from the third party payer.
Services for Children (ARM 37.86.2201–2235)
The Early and Periodic Screening, Diagnostic, and Treatment (EPSDT) Services program is a comprehensive approach to healthcare for Montana Healthcare Programs members age 20 and under. It is designed to prevent, identify, and then treat health problems before they become disabling. Under EPSDT, Montana Healthcare Programs eligible children may receive any medically necessary covered service, including all eye exam and eyeglass services described in this manual. All applicable Passport to Health and prior authorization requirements apply.
Non-Covered Services (ARM 37.85.206, ARM 37.85.207, ARM 37.85.406)
Some services not covered by Montana Healthcare Programs include the following:
- Services considered experimental or investigational
- Dispensing fees for a member who is not eligible for lenses and/or frames within the 760-day time period
- Services that the provider did not personally provide. The main exception is that the dispensing service may be performed by the provider’s employee when it is allowed by law.
Importance of Fee Schedules
The easiest way to verify coverage for a specific service is to check the Department’s fee schedule. Fee schedules list Montana Healthcare Programs covered codes and provide clarification of indicators such as whether a code requires prior authorization, can be applied to a co-surgery, can be billed bilaterally, etc. All services provided must also meet the coverage criteria listed in the Provider Requirements chapter of the General Information for Providers manual and in this chapter. Use the fee schedule in conjunction with the more detailed coding descriptions listed in the current CPT and HCPCS coding books. Take care to use the fee schedule and coding books that pertain to the date of service. Fee schedules are available on the Provider Information website.
Retroactive Eligibility
Montana Healthcare Programs does not cover eyeglasses for members who become retroactively eligible for Montana Healthcare Programs when the eyeglasses were purchased before retroactive eligibility was determined. However, Montana Healthcare Programs does cover eye exams for retroactively eligible members. For example, suppose that a member had an eye exam and purchased eyeglasses on July 15. On September 1, the Department determined the member was eligible for Montana Healthcare Programs retroactive to July 1. Montana Healthcare Programs would pay for the eye exam but not for the eyeglasses.
Use the current fee schedule for your provider type to verify coverage for specific services.
Coverage of Specific Services
The following are coverage rules for specific services provided by optometrists, opticians, and ophthalmologists. Due to limits on exams and eyeglasses, before providing these services, the provider should contact Provider Relations to verify the member is currently eligible for an exam, and contact the eyeglass contractor to verify the member is eligible for eyeglasses. Montana Healthcare Programs will only pay for eyeglasses and frames purchased through the Department’s eyeglass contractor. All services are subject to post payment review and payment recovery if they are not medically necessary. (See the Surveillance and Utilization Review chapter in the General Information for Providers manual.)
Montana Healthcare Programs will only pay for eyeglasses and frames purchased through the Department’s eyeglass contractor.
Contact Lenses
Contact lenses are covered only when medically necessary and not for cosmetic reasons. Dispensing providers must obtain prior authorization for all contact fitting, contact lenses and dispensing fees. (See the Prior Authorization chapter in this manual.) The same limits that apply to eyeglasses and repairs also apply to contacts. Contact lenses are not provided by the eyeglass contractor and therefore may be provided by other providers. Montana Healthcare Programs covers them when the member has one the following conditions:
- Keratoconus
- Sight that cannot be corrected to 20/40 with eyeglasses
- Aphakia
- Anisometropia of 2 diopters or more
Eye Exams
Before providing an eye exam, verify that the member is eligible for an exam by contacting Provider Relations. Montana Healthcare Programs members age 21 or over are limited to one eye examination for determining refractive state every 730 days. Montana Healthcare Programs members ages 20 or under are limited to one eye examination for determining refractive state every 365 days. See Eyeglass Services in the Billing Procedures chapter of this manual for details on how to bill.
The Department allows exceptions to these limits when one of the following conditions exists:
- Following cataract surgery, when more than one exam during the respective period is necessary.
- A screening shows a loss of one line acuity with present eyeglasses.
- Adult diabetic members may have exams every 365 days.
If a provider does not check member eligibility prior to an exam, and the claim is denied because the member’s exam limit was exceeded, the provider cannot bill Montana Healthcare Programs or the member.
Eyeglass Services
Before providing eyeglasses to a member, verify that the member is eligible by contacting Montana Provider Relations for exam and eyeglass frequency. Adults ages 21 or older are eligible for eyeglasses every 730 days. If the member has a diagnosed medical condition that prohibits the use of bifocals, Montana Healthcare Programs may cover two pairs of single vision eyeglasses every 365 days. Prior authorization is not required, but the provider must document the member’s inability to use bifocals and request a verbal approval from the Department Program Office. Children age 20 or under are eligible for eyeglasses every 365 days. If one of the following circumstances exists for one eye, within the respective time limits, lenses only will be replaced.
Adults (age 21 and older) are limited to one eye exam and one pair of eyeglasses every 730 days. Children (ages 20 and under) are limited to one eye exam and one pair of eyeglasses every 365 days.
- .50 diopter change in correction in sphere
- .75 diopter change in cylinder
- .5 prism diopter change in vertical prism
- .50 diopter change in the near reading power
- A minimum of a 5 degree change in axis of any cylinder less than or equal to 3.00 diopters
- A minimum of a 3 degree change in axis of any cylinder greater than 3.00 diopters
- Any 1 prism diopter or more change in lateral prism
If any one of these changes is in one eye, Montana Healthcare Programs will cover that lens only. Montana Healthcare Programs will not cover a new frame at the time of a prescription change within the respective time limits.
Eyeglasses are covered for an initial/new prescription when the member has at least one of the following circumstances in one or both eyes:
- Cataract surgery
- .50 diopter correction in sphere
- .75 diopter correction in cylinder
- .5 prism diopter correction in vertical prism
- .50 diopter correction in near reading power
- Any 1 prism diopter or more correction in lateral prism
Frame Services
The eyeglass contractor will provide a list of Montana Healthcare Programs-covered frames to dispensing providers. Montana Healthcare Programs members have the option of using their existing frames and Montana Healthcare Programs will cover lenses. The existing frame is a frame that the member owns or purchases. When a member chooses to use an existing frame, the following apply:
- Dispensing providers will evaluate existing frames to ensure lenses can be inserted.
- The eyeglass contractor will decide if the existing frame can be used for Montana Healthcare Programs covered lenses. If the existing frame cannot be used, the eyeglass contractor will inform the dispensing provider.
- If the existing frame breaks (after lenses are dispensed to the member), Montana Healthcare Programs will pay for a contract frame but not new lenses. The member can choose to pay privately for new lenses or find a contract frame that the lenses will fit. New lenses are not covered in this case.
Lens Add-Ons
Lens Feature: Photochromic - plastic (i.e., transition)
Children: Yes - if medically necessary
Adults: No
Charge: $18.00
Lens Feature: Photochromic - glass (i.e., photogray, photobrown)
Children: Yes - if medically necessary
Adults: No
Charge: $18.00
Lens Feature: Progressive - no line
Children: No
Adults: No
Charge: $27.00
Lens Feature: Polycarbonate lenses (Single vision, bifocal, or trifocal lenses)
Children: Yes - if member is monocular
Adults: Yes - if member is monocular
Charge: $4.00
Lens Feature: Tints Rose 1 and Rose 2 (applicable to CR-39 and Polycarbonate lenses only)
Children: Yes
Adults: Yes
Charge: No charge
Lens Feature: Deluxe Frames
Children: Yes - if medically necessary
Adults: No
Charge: $30.00
Lens Feature: Round bifocal/plastic only
Children: Yes - if medically necessary
Adults: No
Charge: $7.70
Lens Feature: Tints other than Rose 1 and Rose 2 (applicable to CR-39 and Polycarbonate lenses only)
Children: Yes - if medically necessary
Adults: No
Charge: $2.00
Lens Feature: UV and scratch-resistant coatings
Children: Yes - if medically necessary
Adults: No
Charge: $1.00
Children qualify as ages 20 and under.
Any lens style, lens material, tint, coating lens enhancement (polished edge, etc.) not specifically noted above or within this manual will be billed to the dispensing provider at the eyeglass contractor’s normal and customary charges. The Department requests that providers bill members the Classic Optical Montana Healthcare Programs rate for scratch guard and polycarbonate lenses. For other add-ons noted above that are not covered by Montana Healthcare Programs, payment is a private arrangement between the member and the provider, and the provider may charge the usual private-pay rate or the Classic Optical Montana Healthcare Programs rate to the member.
Lens Styles and Materials
All eyeglass lenses fabricated by the eyeglass contractor for Montana Healthcare Programs members must be in the edged form, edged to shape and size for a specific frame and returned to the dispensing provider as lenses only, or edged and mounted into a specific frame and returned to the dispensing provider as complete Rx order. Orders for uncut lenses are not accepted.
Montana Healthcare Programs covers the following lens styles:
- Single vision
- Flattop segments 25, 28, 35
- Flattop trifocals 7 x 25, 7 x 28, 8 x 35
- Round bifocals 22 and 34
- Executive style bifocals
Montana Healthcare Programs covers the following lens materials (no high index):
- Glass
- CR-39
- Polycarbonate for monocular members only. Montana Healthcare Programs members who are not monocular can choose polycarbonate lenses and pay the difference as an add-on. (See previous table titled Lens Add-Ons.)
Replacement Lenses and Frames
All frames provided by the Montana Healthcare Programs contractor carry a 12-month manufacturer warranty on replacement fronts and temples. Montana Healthcare Programs members must bring their broken frames into the dispensing provider for the contractor to repair. No new frame style or color can replace the broken frame.
If an adult (ages 21 and older) loses his/her eyeglasses within the 12 months, Montana Healthcare Programs will not cover another pair. If an adult’s lenses are broken or unusable, the member is eligible for replacement lenses (not frames) within the first 12 months after the initial dispensing of contract eyeglasses.
If a Montana Healthcare Programs/HMK child (ages 20 and under) loses or breaks the first pair of eyeglasses, and the damage is not covered by the warranty, Montana Healthcare Programs will replace one pair of eyeglasses within the 365 day period. Additional replacement requests must be reviewed by the Department Program Officer. Parents/guardians may purchase additional replacement eyeglasses at the Montana Healthcare Programs contract rate. If a HMK/CHIP (18 & under) member loses or break a pair of eyeglasses, and the damage is not covered by the warranty, HMK will NOT replace the eyeglasses. However, if there is a prescription change that meets criteria amount of change, lenses only will be replaced and not the frame. Members can purchase frames through Classic Optical at the contract price or the dispending providers usual and customary charge.
Eyeglass Ordering Procedures
The Montana contracted provider, Classic Optical, offers an online ordering system to order eyeglasses for Montana Healthcare Programs and HMK members. Dispensing providers need to be signed up with Classic Optical and the website and log-on information will be provided from Classic Optical. The contact phone number for Classic Optical is located in “Key Contacts” at the front of this manual.
When the date of service is near the end of the month, order online or fax orders to the eyeglasses contractor.
Tips for Completing the Classic Optical online order form:
- The date of service for dispensing eyeglasses (measuring, verifying, and fitting) is the date the eyeglasses are ordered from the contractor.
- The date of service for eyeglass materials is the date the order is received by the eyeglass contractor.
- Encounters with the member on and after the date the glasses are dispensed are considered follow-up and are covered within the measuring, verifying, and fitting fee.
- When the date of service is near the end of the month, please complete online or fax orders to the contractor. This will help ensure the member is eligible for eyeglasses since eligibility can change monthly. If you experience any difficulty faxing the contractor, contact the contractor manager immediately. (See Key Contacts.)
- When an order requires a Prior Authorization number from the department and one has been issued, the number needs to be on the order form. The order along with the department’s document of the Prior Authorization number will be faxed to Classic Optical.
- Check the EPSDT box when the Montana Healthcare Programs member is age 20 or under.
- 2nd PR S.V. is used when ordering two pairs of single vision eyeglasses (one for distance and one for reading) when a Montana Healthcare Programs member cannot wear multi-focal eyeglasses. An ophthalmologist or optometrist must keep documentation of the member’s inability to wear multi-focal eyeglasses.
Submitting the Montana Healthcare Programs Rx Form
- Place the order online with Classic Optical or fax or mail the order form to the eyeglass contractor. (See Key Contacts.) Phone orders are not accepted. To ensure orders will be processed accurately and on time, all sections of the order form must be completed.
- Errors in the fabrication of eyeglasses made by the eyeglass contractor will be corrected by the contractor at no additional charge.
- If the dispensing provider makes a mistake on a prescription, the eyeglass contractor will correct the error (but not cover the cost of the remaking of the eyeglasses). The dispensing provider will order the correct prescription and return the incorrect eyewear to Classic Optical. Classic Optical will charge the dispensing provider full price for the eyeglasses that were originally made. When the return eyewear arrives at Classic Optical, the dispensing provider will be reimbursed 50% of the cost of the first eyeglasses that were made incorrectly.
Other Programs
This is how the information in this chapter applies to Department programs other than Montana Healthcare Programs.
Healthy Montana Kids Program (HMK)/CHIP
Eyeglass services are covered by HMK/Montana Provider Relations, but optometric services are covered by Blue Cross and Blue Shield of Montana/CHIP. Most of the eyeglass services information in this chapter applies to HMK members. The exceptions are as follows:
- HMK members are eligible for eyeglasses every 365 days.
- HMK members do not receive retroactive eligibility.
- HMK members are not eligible for replacement lenses or frames that are not covered under manufacturer’s warranty or are lost or stolen.
- HMK members are 18 years of age or under.
- HMK members are not eligible for contact lenses or contacts lens exams.
Additional information regarding HMK is available on the HMK website at https://dphhs.mt.gov/HMK.
Mental Health Services Plan (MHSP)
Eye exams and eyeglasses are not covered under the Mental Health Services Plan (MHSP). See the mental health manual on the Provider Information website.
End of Covered Services Chapter
Prior Authorization
What Are Prior Authorization and the Team Care Program?
Although Passport to Health requirements do not apply to optometric, ophthalmologist and eyeglass services, prior authorization is required for some services, and the member may be part of the Team Care Program.
Team Care (ARM 37.86.5303)
Team Care is a restricted services program that is part of Passport to Health. Restricted services programs are designed to assist members in making better healthcare decisions so that they can avoid over utilizing health services. Team Care members are joined by a team assembled to assist them in accessing healthcare. The team consists of the member, the PCP, a pharmacy, and the Department. The team may also include a community-based care manager from the Department's Health Improvement Program.
Prior Authorization
Some services require prior authorization before providing them. If a service requires prior authorization, the requirement exists for all Montana Healthcare Programs members.
When seeking prior authorization, keep in mind the following:
- The referring provider should initiate all authorization requests.
- Always refer to the Montana Healthcare Programs fee schedule for prior authorization requirements on specific services.
- Eyeglasses have some services that are add-on features that require prior authorization. These features are not part of the contract of covered items with the eyeglass supplier and are listed as needing prior authorization on the Eyeglasses Fee Schedule, available on the Provider Information website.
- Have all required documentation that may be needed before submitting for prior authorization. For documentation requirements, see the Prior Authorization Criteria for Specific Services table.
Prior Authorization Criteria for Specific Services
Services: Dispensing and fitting of contact lenses
PA Contact:
DPHHS Optometric Program Officer
P.O. Box 202951
Helena, MT 59620
Phone: (406) 444-4066
Fax: (406) 444-1861
Documentation Required:
- Prior authorization is required for contact lenses and dispensing fees.
- Diagnosis must be one of the following:
- Keratoconus
- Aphakia
- Sight cannot be corrected to 20/40 with eyeglasses
- Anisometropia of 2 diopters or more
Services: Transition lenses, Tints other than Rose 1 and Rose 2 (including photochromic tints), UV and scratch resistant coating, Polycarbonate lenses, Round bifocals, and Deluxe frames.
PA Contact:
Optometric Program
Health Resources Division
P.O. Box 202951
Helena, MT 59620-2951
Fax: (406) 444-1861
Documentation Required:
- Requests for prior authorization must:
- Be submitted by fax or mailed to the Department.
- Include diagnosis and sufficient documentation from the optometrist or ophthalmologist that transition lenses, tints, UV and scratch resistant coating, or deluxe frames are medically necessary.
- For polycarbonate lenses, include documentation verifying member is monocular.
Services: Eye Prosthesis
PA Contact:
Mountain-Pacific Quality Health
3404 Cooney Drive
Helena, MT 59602
Phone: (877) 443-4021, Long-distance
(406) 457-3060 Local
Fax: (877) 443-2580 Long-distance
(406) 513-1923 Local
For HMK members, BCBSMT case managers review requests for durable medical equipment. If the cost is greater than $500, prior authorization is required.
Documentation Required:
- Documentation that supports medical necessity
- Documentation regarding the member’s ability to comply with any required after care
- Letters of justification from referring physician
- Documentation should be provided at least two weeks prior to the procedure date.
Other Programs
The prior authorization requirements apply to Healthy Montana Kids (HMK) eyeglass services. Optometric services are covered under the HMK plan of Blue Cross and Blue Shield of Montana (BCBSMT). Eye exams and eyeglasses are not covered under the Mental Health Services Plan (MHSP). Refer to the mental health services manual on the Provider Information website.
End of Prior Authorization Chapter
Coordination of Benefits
When Members Have Other Coverage
Montana Healthcare Programs members often have coverage through Medicare, workers’ compensation, employment-based coverage, individually purchased coverage, etc. Coordination of benefits is the process of determining which source of coverage is the primary payer in a particular situation. In general, providers must bill other carriers before billing Montana Healthcare Programs, but there are some exceptions. (See Exceptions to Billing Third Party First later in this chapter.) Medicare coverage is processed differently than other sources of coverage.
Identifying Other Sources of Coverage
The member’s Montana Healthcare Programs ID card may list other payers such as Medicare or other third party payers. (See Member Eligibility and Responsibilities in the General Information for Providers manual.) If a member has Medicare, the Medicare ID number is listed on the card. If a member has other coverage (excluding Medicare), it will be shown under the TPL section of the ID card. Some examples of third party payers include:
- Private health insurance
- Employment-related health insurance
- Workers’ compensation insurance*
- Health insurance from an absent parent
- Automobile insurance*
- Court judgments and settlements*
- Long-term care insurance
*These third party payers (and others) may not be listed on the member’s ID card.
Medicare claims are processed differently than other sources of coverage.
Providers must use the same procedures for locating third party sources for Montana Healthcare Programs members as for their non-Montana Healthcare Programs members. Providers cannot refuse service because of a third party payer or potential third party payer.
When a Member Has Medicare
Medicare claims are processed and paid differently than claims involving other payers. The other sources of coverage are referred to as third party liability (TPL), but Medicare is not.
Medicare Part A Claims
Medicare Part A covers inpatient hospital care, skilled nursing care and other services. Medicare Part A services are covered in more detail in specific program manuals where the providers bill for Part A services.
Medicare Part B Crossover Claims
Medicare Part B covers physician care, eye exams, and other services. The Department has an agreement with Medicare Part B carriers for Montana (Noridian) and the Durable Medical Equipment Regional Carrier (DMERC). Under this agreement, the carriers provide the Department with a magnetic tape of CMS-1500 claims for members who have both Medicare and Montana Healthcare Programs coverage. For claims to automatically cross over from Medicare to Montana Healthcare Programs, providers must:
- Accept Medicare assignment (otherwise payment and the Explanation of Medicare Benefits (EOMB) go directly to the member and will not cross over).
- Submit their Medicare and Montana Healthcare Programs provider numbers to Provider Relations.
In these situations, providers need not submit Medicare Part B crossover claims to Montana Healthcare Programs. Medicare will process the claim, submit it to Montana Healthcare Programs, and send the provider an EOMB. Providers must check the EOMB for the statement indicating that the claim has been referred to Montana Healthcare Programs for further processing. It is the provider’s responsibility to follow up on crossover claims and make sure they are correctly billed to Montana Healthcare Programs within the timely filing limit. (See Billing Procedures.)
When submitting electronic claims with paper attachments, see the Billing Electronically with Paper Attachments section of the Billing Procedures chapter in this manual.
When Medicare Pays or Denies a Service
- When Medicare pays an eye exam claim for a provider that is set up for automatic crossover, the claim should automatically cross over to Montana Healthcare Programs for processing, so the provider does not need to submit these claims to Montana Healthcare Programs. Providers that are not set up for automatic crossover should submit a claim to Montana Healthcare Programs after Medicare pays, and Montana Healthcare Programs will consider the claim for payment. If Medicare denies an eye exam claim, submit the claim to Montana Healthcare Programs. (See Submitting Medicare Claims to Montana Healthcare Programs later in this chapter.)
- Members who have Medicare/QMB or Medicare/Montana Healthcare Programs coverage must choose whether to access their Medicare or Montana Healthcare Programs benefits for eyeglasses. If a member chooses to use Medicare, do not bill Montana Healthcare Programs, and any claims that cross over from Medicare will be denied.
- For members who have QMB only coverage, the provider bills Medicare first for eyeglass claims, and if Medicare pays the claim, Montana Healthcare Programs will consider the claim for payment. If Medicare denies the claim, Montana Healthcare Programs will also deny the claim. For more information on QMB, see the General Information for Providers manual, Member Eligibility and Responsibilities chapter.
All Part B crossover claims submitted to Montana Healthcare Programs before Medicare’s 45-day response time will be returned to the provider.
When Montana Healthcare Programs Does Not Respond to Crossover Claims
When Montana Healthcare Programs does not respond within 45 days of the provider receiving the Medicare EOMB, submit a claim, with a copy of the Medicare EOMB, to Montana Healthcare Programs for processing.
Submitting Medicare Claims to Montana Healthcare Programs
When submitting a paper claim to Montana Healthcare Programs, attach the Medicare EOMB and use Montana Healthcare Programs billing instructions and codes. Medicare’s instructions, codes, and modifiers may not be the same as Montana Healthcare Programs’s. The claim must also include the provider’s NPI and Montana Healthcare Programs member ID number.
Remember to submit Medicare crossover claims to Montana Healthcare Programs only:
- When the referral to Montana Healthcare Programs statement is missing from the provider’s EOMB.
- When the provider does not hear from Montana Healthcare Programs within 45 days of receiving the Medicare EOMB.
When a Member Has TPL (ARM 37.85.407)
When a Montana Healthcare Programs member has additional medical coverage (other than Medicare), it is often referred to as third party liability (TPL). In most cases, providers must bill other insurance carriers before billing Montana Healthcare Programs.
Providers are required to notify their members that any funds the member receives from third party payers (when the services were billed to Montana Healthcare Programs) must be turned over to the Department. The following words printed on the member’s statement will fulfill this requirement: When services are covered by Montana Healthcare Programs and another source, any payment the member receives from the other source must be turned over to Montana Healthcare Programs.
It is the provider’s responsibility to follow up on TPL claims and make sure they are billed correctly to Montana Healthcare Programs within the 12-month timely filing period.
Exceptions to Billing Third Party First
In a few cases, providers may bill Montana Healthcare Programs first.
- When a Montana Healthcare Programs member is also covered by Indian Health Service (IHS) or the Montana Crime Victim Compensation Fund, providers must bill Montana Healthcare Programs before IHS or Crime Victims. These are not considered third party liability.
- If the third party has only potential liability, such as automobile insurance, the provider may bill Montana Healthcare Programs first. Do not indicate the potential third party on the claim. Instead, notify the Department of the potential third party by sending the claim and a note to Third Party Liability. (See the Contact Us page on the Provider Information website.)
Requesting an Exemption
- Providers may request to bill Montana Healthcare Programs first under certain circumstances. In each of these cases, the claim and required information must be sent directly to the Third Party Liability. See the Contact Us page on the Provider Information website.
- When a provider is unable to obtain a valid assignment of benefits, the provider must submit the claim with documentation that the provider attempted to obtain assignment and certification that the attempt was unsuccessful.
- When the Child Support Enforcement Division has required an absent parent to have insurance on a child, the claim can be submitted to Montana Healthcare Programs when the following requirements are met:
- The third party carrier has been billed, and 30 days or more have passed since the date of service.
- The claim is accompanied by a certification that the claim was billed to the third party carrier, and payment or denial has not been received.
- If another insurance has been billed, and 90 days have passed with no response, attach a note to the claim explaining that the insurance company has been billed or attach a copy of the letter sent to the insurance company Include the date the claim was submitted to the insurance company and certification that there has been no response.
- When the provider has billed the third party insurance and has received a non-specific denial (e.g., no member name, date of service, amount billed), submit the claim with a copy of the denial and a letter of explanation directly to Third Party Liability to avoid missing the timely filing deadline.
When the Third Party Pays or Denies a Service
When a third party payer is involved (excluding Medicare) and the other payer:
- Pays the claim. Indicate the amount paid in the Amount Paid field of the claim when submitting to Montana Healthcare Programs for processing. These claims may be submitted either electronically or on paper.
- Allows the claim, and the allowed amount went toward the member’s deductible. Include the insurance Explanation of Benefits (EOB) when billing Montana Healthcare Programs. These claims must be submitted on paper.
- Denies the claim. Include a copy of the denial (including the reason and the reason explanation) with the claim, and submit to Montana Healthcare Programs.
- Denies a line on the claim. Bill the denied lines together on a separate claim and submit to Montana Healthcare Programs. Include the explanation of benefits (EOB) from the other payer as well as an explanation of the reason for denial (e.g., definition of denial codes).
If the provider receives a payment from a third party after the Department has paid the provider, the provider must return the lower of the two payments to the Department within 60 days.
When the Third Party Does Not Respond
If another insurance has been billed, and 90 days have passed with no response, bill Montana Healthcare Programs as follows:
- Attach a note to the claim explaining that the insurance company has been billed, or attach a copy of the letter sent to the insurance company.
- Include the date the claim was submitted to the insurance company.
- Send this information to Third Party Liability. See the Contact Us page on the Provider Information website.
Other Programs
The information in this chapter does not apply to Healthy Montana Kids (HMK) or the Mental Health Services Plan (MHSP). The MHSP manual is available on the Provider Information website.
End of Coordination of Benefits Chapter
Billing Procedures
Claim Forms
Services provided by optometrists, opticians, and ophthalmologists must be billed either electronically on a Professional claim or on a CMS-1500 paper claim form. CMS-1500 forms are available from various publishing companies; they are not available from the Department or Provider Relations.
Timely Filing Limits (ARM 37.85.406)
Providers must submit clean claims to Montana Healthcare Programs within:
- Twelve months from whichever is later:
- The date of service
- The date retroactive eligibility or disability is determined
- Medicare Crossover Claims: Six months from the date on the Medicare explanation of benefits approving the service (if the Medicare claim was timely filed and the member was eligible for Medicare at the time the Medicare claim was filed).
- Claims involving other third party payers (excluding Medicare): Six months from the date on an adjustment notice from a third party payer who has previously processed the claim for the same service, and the adjustment notice is dated after the periods described above.
Clean claims are claims that can be processed without additional information or action from the provider. The submission date is defined as the date that the claim was received by the Department or the claims processing contractor. All problems with claims must be resolved within this 12-month period.
Tips to Avoid Timely Filing Denials
- Correct and resubmit denied claims promptly. (See the Remittance Advices and Adjustments chapter in this manual.)
- If a claim submitted to Montana Healthcare Programs does not appear on the remittance advice within 30 days, contact Provider Relations for claim status.
- If another insurer has been billed and 90 days have passed with no response, a provider can bill Montana Healthcare Programs. (See the Coordination of Benefits chapter in this manual for more information.)
- To meet timely filing requirements for Medicare/Montana Healthcare Programs crossover claims, see the Coordination of Benefits chapter in this manual.
When to Bill Montana Healthcare Programs Members (ARM 37.85.406)
In most circumstances, providers may not bill Montana Healthcare Programs members for services covered under Montana Healthcare Programs.
More specifically, providers cannot bill members directly:
- For the difference between charges and the amount Montana Healthcare Programs paid.
- For a covered service provided to a Montana Healthcare Programs-enrolled member who was accepted as a Montana Healthcare Programs member by the provider, even if the claim was denied.
- When a third party payer does not respond.
- When a member fails to arrive for a scheduled appointment. Montana Healthcare Programs may not be billed for no-show appointments either.
- When services are free to the member, such as in a public health clinic. Montana Healthcare Programs may not be billed for those services either.
Under certain circumstances, providers may need a signed agreement in order to bill a Montana Healthcare Programs member (see the following table).
If a provider bills Montana Healthcare Programs and the claim is denied because the member is not eligible, the provider may bill the member directly.
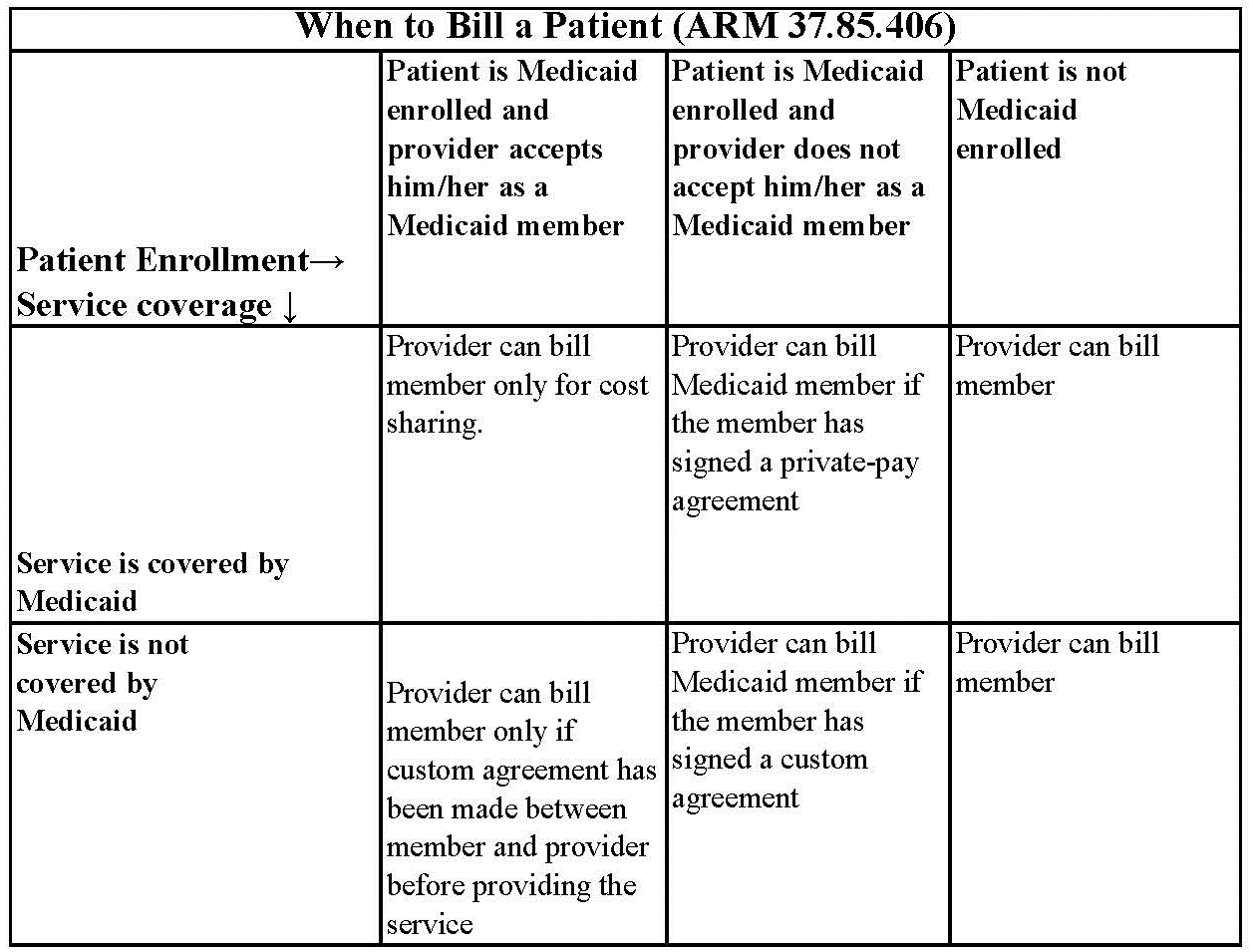
Routine Agreement: This may be a routine agreement between the provider and member which states that the member is not accepted as a Montana Healthcare Programs member, and that he/she must pay for the services received.
Custom Agreement: This agreement lists the service the member is receiving and states that the service is not covered by Montana Healthcare Programs and the member will pay for it.
Usual and Customary Charge (ARM 37.85.406)
Providers should bill Montana Healthcare Programs their usual and customary charge for each service; that is, the same charge that is made to other payers for that service.
Billing Members with Other Insurance
If a Montana Healthcare Programs member is also covered by Medicare, has other insurance, or some other third party is responsible for the cost of the members healthcare, see the Coordination of Benefits chapter in this manual.
Billing for Retroactively Eligible Members
When the provider accepts the member's retroactive eligibility, the provider has 12 months from the date retroactive eligibility was determined to bill for those services. When submitting claims for retroactively eligible members in which the date of service is more than 12 months earlier than the date the claim is submitted, attach a copy of the Notice of Retroactive Eligibility (Form 160-M). To obtain Form 160-M, the provider needs to contact the member's local Office of Public Assistance and request the form. For a list of local Offices of Public Assistance, see https://dphhs.mt.gov/hcsd/OfficeofPublicAssistance.
For more information on retroactive eligibility, see the Member Eligibility and Responsibilities chapter in the General Information for Providers manual.
Place of Service
Place of service must be entered correctly on each line. Montana Healthcare Programs typically reduces payment for services provided in hospitals and ambulatory surgical centers since these facilities typically bill Montana Healthcare Programs separately for facility charges. For a list of place of service codes, see the CMS website: http://cms.hhs.gov/Medicare/Coding/place-of-service-codes/index.html.
Multiple Visits on Same Date
Montana Healthcare Programs generally covers only one dispensing fee per member per day, unless two pairs of single vision eyeglasses are dispensed (distance/near).
When a member requires additional visits on the same day, use a modifier to describe the reason for multiple visits. When a modifier is not appropriate for the situation, attach documentation of medical necessity to the claim, and submit it to the Optometric program officer.
Coding Tips
Standard use of medical coding conventions is required when billing Montana Healthcare Programs. Provider Relations or the Department cannot suggest specific codes to be used in billing for services. For coding assistance and resources, see the table of Coding Resources on the following page. The following suggestions may help reduce coding errors and unnecessary claim denials:
- Use current CPT, HCPCS, and ICD diagnosis coding books.
- Always read the complete description and guidelines in the coding books. Relying on short descriptions can result in inappropriate billing.
- Attend classes on coding offered by certified coding specialists.
- Follow CPT guidelines on the difference between a new member and an established member.
- Bill for the appropriate level of service provided.
- Services covered within global periods for certain CPT procedures are not paid separately and must not be billed separately. Most surgical and some medical procedures include routine care before and after the procedure. Montana Healthcare Programs fee schedules show the global period for each CPT service.
- Use the correct number of units on CMS-1500 claims. In general, Montana Healthcare Programs follows the definitions in CPT and HCPCS coding manuals. Unless otherwise specified, one unit equals one visit or one procedure. For specific codes, however, one unit may be 15 minutes. Always check the long text of the code description.
- CPT codes that are billed based on the amount of time spent with the member must be billed with the code that is closest to the time spent.
Coding Resources
Please note that the Department does not endorse the products of any particular publisher.
CPT
Description:
CPT codes and definitions.
Updated each January.
Contact:
American Medical Association - https://commerce.ama-assn.org/store/
(800) 621-8335
CPT Assistant
Description:
A newsletter on CPT coding issues.
Contacts:
American Medical Association - https://commerce.ama-assn.org/store/
(800) 621-8335
HCPCS Level II
Description:
HCPCS codes and definitions.
Updated each January and throughout the year.
Contact:
Available through various publishers and bookstores or from CMS at www.cms.gov.
ICD
Description:
ICD diagnosis and procedure code definitions.
Updated each October .
Contact:
Available through various publishers and bookstores.
Miscellaneous Resources
Various newsletters and other coding resources are available in the commercial marketplace.
UB-04 National Uniform Billing Expert
Description:
National UB-04 billing instructions
Contact:
Available through various publishers and editors
Using the Montana Healthcare Programs Fee Schedule
When billing Montana Healthcare Programs, it is important to use the Department’s fee schedule for your provider type in conjunction with the detailed coding descriptions listed in CPT and HCPCS coding books. In addition to covered services and payment rates, fee schedules often contain helpful information such as global periods, if multiple surgery guidelines apply, if the procedure can be done bilaterally, if an assistant, co-surgeon, or team is allowed for the procedure, if the code is separately billable, if prior authorization is required, and more. Department fee schedules are updated each January and July; some also in April and October. Be aware of fee schedule publish dates. Fee schedules are available on the Provider Information website.
Using Modifiers
- Review the guidelines for using modifiers in the current CPT, HCPCS, or other helpful resources.
- Always read the complete description for each modifier; some modifiers are described in the CPT manual while others are in the HCPCS coding book.
- The Montana Healthcare Programs claims processing system recognizes three pricing modifiers and one informational modifier per claim line. Providers are asked to place any modifiers that affect pricing in the first two modifier fields.
- When billing with Modifier 50 for bilateral services, put all information on one line with one unit. You do not need to use modifiers for left and right, and do not bill on separate lines.
- Check the fee schedule to see if Montana Healthcare Programs allows the use of the following modifiers for a particular code: bilateral (50), multiple procedures (51), co-surgery (62), assistant at surgery (80, 81, 82, AS).
Billing Tips for Specific Services
Bundled Services
Certain services with CPT or HCPCS codes (e.g., tear duct plugs) are covered by Montana Healthcare Programs but have a fee of zero. This means that the service is typically “bundled” with an office visit or other service. Since the bundled service is covered by Montana Healthcare Programs, providers may not bill the member separately for it.
Contact Lenses
When billing Montana Healthcare Programs for contact lenses, include the prior authorization number on the claim.
Eye Exams
- A member may be eligible for an eye exam before the specified time limit expires if he/she meets the criteria described in the Covered Services chapter, Eye Exams section, of this manual. In this case, enter the reason for the exam on the claim.
- Medicare does not cover eye refraction but instructs providers to report this service as a separate line item from the other services performed. Montana Healthcare Programs covers this procedure, so providers can bill for the eye exam and the refraction.
- Children (age 20 or under for Montana Healthcare Programs or age 18 or under for HMK) may receive an additional exam before the 365-day limit has passed if they have had at least a one line acuity change resulting in prescribing replacement lenses that meet the criteria in the Eyeglass Services section of the Covered Services chapter in this manual. In this case, providers may bill Montana Healthcare Programs for the exam using EPSDT indicator 1 on the claim. See the Submitting a Claim chapter in this manual.
Eyeglass Services
- Adult members (ages 21 or older) may receive new lenses before the 730-day limit has passed if they meet the criteria described the Eyeglass Services and the Services for Children section of the Covered Services chapter in this manual. In this case, providers may bill Montana Healthcare Programs for a dispensing fee for new lenses using the appropriate modifiers with the dispensing fee procedure code. Adult members may be eligible for replacement lenses 12 months after the initial dispensing of contract eyeglasses if the lenses are broken or unusable.
- Children (age 20 or under for Montana Healthcare Programs or age 18 or under for HMK) may receive new lenses before the 365-day limit has passed if they meet the criteria in the Eyeglass Services section of the Covered Services chapter in this manual. In this case, providers may bill Montana Healthcare Programs for a dispensing fee for new lenses using EPSDT indicator 1 on the claim.
- If the adult Montana Healthcare Programs member (age 21 or over) is not eligible for lenses and/or frame within the 730-day period, the dispensing provider may not bill Montana Healthcare Programs for a dispensing fee. If the member chooses to purchase eyeglasses privately, the provider may bill the Montana Healthcare Programs member for dispensing services and eyeglass materials.
- The eyeglass contractor will bill Montana Healthcare Programs for the laboratory and material costs for lenses and frames.
- Bill HMK for eyeglass services and optometric services.
Frame Services
- When the Montana Healthcare Programs member uses an existing frame, the dispensing provider bills Montana Healthcare Programs for dispensing services, lenses only.
- Providers may not charge a dispensing fee for minor frame repairs that they provide themselves.
- If a member who is covered by Medicare and Montana Healthcare Programs chooses a frame outside the Montana Healthcare Programs contract, the provider cannot bill Montana Healthcare Programs for the dispensing fee. All charges must be billed to Medicare and the member.
Lens Add-Ons
The eyeglass contractor bills the dispensing provider their usual and customary charge for any lens style, lens material, tint, coating, lens enhancement (e.g., polished edge) not covered by Montana Healthcare Programs. It is the dispensing provider’s responsibility to bill the Montana Healthcare Programs member for these items. Do not bill Montana Healthcare Programs.
For example, FT7x35 Trifocal is billed to the dispensing provider at the contractor’s usual and customary price, not at a price which would reflect the difference between the contract price for 7x28, and the usual and customary 7x35 price. For FT 28 CR-39 with polished edges, only the polished edge price is billed to the dispensing provider at the contractor’s usual and customary charge.
Replacement Lenses and Frames
If a member has selected to use an existing frame, and the existing frame breaks after lenses were dispensed to the member, Montana Healthcare Programs will not cover new lenses. The Montana Healthcare Programs member may privately pay for new lenses or select a contract frame into which the existing lenses will fit. If a contract frame is selected, the dispensing provider may bill Montana Healthcare Programs for dispensing services, frame only.
Submitting Electronic Claims
Institutional claims submitted electronically are referred to as ANSI ASC X12N 837 transactions. Providers who submit claims electronically experience fewer errors and quicker payment. Providers should be familiar with federal rules and regulations regarding electronic transactions. Claims may be submitted electronically by the following methods:
- WINASAP 5010. Montana Provider Relations makes this free software available to providers who may use it to submit claims for Montana Healthcare Programs, MHSP, HMK (dental and eyeglasses only) and FQHC/RHC. It does not support submissions to Medicare or other payers. This software creates an 837 transaction, but does not accept an 835 transaction back from the Department.)
- Montana Access to Health (MATH) Web Portal. A secure website on which providers may view members’ medical history, verify member eligibility, submit electronic claims to Montana Healthcare Programs via a HIPAA-compliant X12 837 file, check the status of a claim, verify the status of a warrant, and download remittance advice reports.
- EDI Clearinghouse. Providers can send claims to the EDI clearinghouse (EDI Solutions) in X12 837 format. Electronic submitters are required to certify their 837 transactions as HIPAA-compliant before sending their transactions through the EDI clearinghouse. EDIFECS certifies the 837 HIPAA transactions at no cost to the provider. EDIFECS certification is completed through EDI Solutions.
- Clearinghouses. Providers can contract with a clearinghouse and send claims in whatever format the clearinghouse accepts. The provider’s clearinghouse then sends the claim to the EDI clearinghouse in the X12 837 format. The provider’s clearinghouse also needs to have their 837 transactions certified through EDIFECS before submitting claims to the EDI clearinghouse. EDIFECS certification is completed through EDI Solutions. For more information on electronic claims submission, contact the EDI Support Unit.
- MOVEit DMZ. Providers use this secure transmission protocol and secure storage landing zone (intermediate storage) for the exchange of files between trading partners and EDI. It is intended for trading partners/submitters who submit in excess of 20 files per day or whose physical file sizes regularly exceed 2 MB.
- B2B Gateway SFTP/FTPS Site. Providers use this method to send electronic transactions through the secure FTP process. This is typically encountered with high-volume/high-frequency submitters.
Billing Electronically with Paper Attachments
When submitting claims that require additional supporting documentation, the Attachment Control Number field must be populated with an identifier. Identifier formats can be designed by software vendors or clearinghouses, but the preferred method is the provider’s NPI followed by the member’s ID number and the date of service, each separated by a dash:

The supporting documentation must be submitted with a Paperwork Attachment Cover Sheet. (See the Forms page of the Provider Information website.) The number in the paper Attachment Control Number field must match the number on the cover sheet.
Submitting Paper Claims
For instructions on completing a paper claim, see the Submitting a Claim chapter in this manual. Unless otherwise stated, all paper claims must be mailed to:
Claims Processing
P.O. Box 8000
Helena, MT 59604
Claim Inquiries
If you have questions on a specific claim, contact Provider Relations. See the Contact Us page on the Provider Information website.
The Most Common Billing Errors and How to Avoid Them
Paper claims are often returned to the provider before they can be processed, and many other claims (both paper and electronic) are denied.
To avoid unnecessary returns and denials, double-check each claim to confirm the following items are included and accurate.
Common Billing Errors
Reasons for Return or Denial: Provider NPI missing or invalid
How to Prevent Returned or Denied Claims: The provider NPI is a 10-digit number assigned to the provider by the National Plan and Provider Enumeration System. Verify the correct provider NPI is on the claim.
Reasons for Return or Denial: Authorized signature missing
How to Prevent Returned or Denied Claims: Each claim must have an authorized signature belonging to the provider, billing clerk, or office personnel. The signature may be typed, stamped, or hand-written.
Reasons for Return or Denial: Signature date missing
How to Prevent Returned or Denied Claims: Each claim must have a signature date.
Reasons for Return or Denial: Incorrect claim form used
How to Prevent Returned or Denied Claims: The claim must be the correct form for the provider type. Services covered in this manual require a CMS-1500 claim form (or electronic Professional claim).
Reasons for Return or Denial: Information on claim form not legible
How to Prevent Returned or Denied Claims: Information on the claim form must be legible. Use dark ink and center the information in the field. Information must not be obscured by lines.
Reasons for Return or Denial: Member number not on file, or member was not eligible on date of service
How to Prevent Returned or Denied Claims: Before providing services to the member:
- View the member’s ID card at each visit. Montana Healthcare Programs eligibility may change monthly.
- Verify member eligibility by using one of the methods described in the Member Eligibility and Responsibilities chapter of the General Information for Providers manual.
Reasons for Return or Denial: Duplicate claim
How to Prevent Returned or Denied Claims:
- Check all remittance advices for previously submitted claims before resubmitting.
- When making changes to previously paid claims, submit an adjustment form rather than a new claim. (See Remittance Advices and Adjustments in this manual.)
- Allow 45 days for the Medicare/Montana Healthcare Programs Part B crossover claim to appear on the remittance advice before submitting the claim directly to Montana Healthcare Programs.
Reasons for Return or Denial: Medicare Part B crossover claims submitted before Medicare’s 45-day crossover limit
How to Prevent Returned or Denied Claims: Claims that cross over between Medicare Part B and Montana Healthcare Programs should not be billed on paper to Montana Healthcare Programs until 45 days after the Medicare Part B paid date. These claims will be returned to the provider.
Reasons for Return or Denial: Prior authorization number is missing
How to Prevent Returned or Denied Claims:
- Prior authorization is required for certain services, and the prior authorization number must be on the claim. (See the Prior Authorization chapter in this manual.)
- Mental Health Services Plan (MHSP) claims must be billed and services performed during the prior authorization span. The claim will be denied if it is not billed according to the spans on the authorization. See mental health services manual.
Reasons for Return or Denial: TPL on file and no credit amount on claim
How to Prevent Returned or Denied Claims:
- If the member has any other insurance (or Medicare), bill the other carrier before Montana Healthcare Programs. See Coordination of Benefits in this manual.
- If the member’s TPL coverage has changed, providers must notify TPL before submitting a claim. See the Contact Us page on the Provider Information website.
Reasons for Return or Denial: Claim past 365-day filing limit
How to Prevent Returned or Denied Claims:
- Claims Processing must receive all clean claims and adjustments within the timely filing limits described in this chapter.
- To ensure timely processing, claims and adjustments must be mailed to Claims Processing. See the Contact Us page on the Provider Information website.
Reasons for Return or Denial: Missing Medicare EOMB
How to Prevent Returned or Denied Claims: All Medicare crossover claims on CMS-1500 forms must have an Explanation of Medicare Benefits (EOMB) attached, and be billed to Montana Healthcare Programs on paper.
Reasons for Return or Denial: Provider is not eligible during dates of services, or provider NPI terminated
How to Prevent Returned or Denied Claims:
- Out-of-state providers must update enrollment early to avoid denials. If enrollment has lapsed, claims submitted with a date of service after the expiration date will be denied until the provider updates his/her enrollment.
- New providers cannot bill for services provided before Montana Healthcare Programs enrollment begins.
- If a provider is terminated from the Montana Healthcare Programs, claims submitted with a date of service after the termination date will be denied.
Reasons for Return or Denial: Type of service/procedure is not allowed for provider type
How to Prevent Returned or Denied Claims:
- Provider is not allowed to perform the service, or type of service is invalid.
- Verify the procedure code is correct using applicable CPT and HCPCS coding books.
- Check the Montana Healthcare Programs fee schedule to verify the procedure code is valid for your provider type.
Other Programs
Billing procedures for eyeglass services apply to Healthy Montana Kids (HMK); however, billing procedures for eye exams do not apply to HMK because optometric services are covered by Blue Cross and Blue Shield of Montana. These billing procedures do not apply to the Mental Health Services Plan (MHSP); that manual is available on the Provider Information website.
End of Billing Procedures Chapter
Submitting a Claim
The services described in this manual are billed either electronically on a Professional claim or on a paper CMS-1500 claim form. Claims submitted with all of the necessary information are referred to as clean and are usually paid in a timely manner. (See the Billing Procedures chapter in this manual.)
Claims are completed differently for the different types of coverage a member has. The following are accepted codes:
EPSDT/Family Planning Indicators
Code: 1 Member/Service: EPSDT
Purpose: Used when the member is under age 21.
Code: 2 Member/ Service: Family Planning
Purpose: Used when providing family planning services.
Code: 3 Member/ Service: EPSDT and Family Planning
Purpose: Used when the member is under age 21 and is receiving family planning services.
Code: 4 Member/ Service: Pregnancy (any service provided to a pregnant woman)
Purpose: Used when providing services to pregnant women.
Code: 6 Member/ Service: Nursing facility member
Purpose: Used when providing services to nursing facility residents.
Unless otherwise stated, all paper claims must be mailed to the following address:
Claims Processing
P.O. Box 8000
Helena, MT 59604
Avoiding Claim Errors
Claims are often denied or even returned to the provider before they can be processed. To avoid denials and returns, double-check each claim to confirm the items below are accurate. For more information on returned and denied claims, see the Billing Procedures chapter in this manual.
Common Claim Errors
Claim Error: Required field is blank
Prevention: Check the claim instructions earlier in this chapter for required fields (indicated by * or **). If a required field is blank, the claim may either be returned or denied.
Claim Error: member ID number missing or invalid
Prevention: This is a required field (Field 10d); verify that the member’s Montana Healthcare Programs ID number is listed as it appears on the member’s eligibility information.
Claim Error: member name missing
Prevention: This is a required field (Field 2); check that it is correct.
Claim Error: NPI/API missing or invalid
Prevention: The NPI is a 10-digit number (API is a 7-digit) assigned to the provider. Verify the correct NPI/API is on the claim.
Claim Error: Referring or Passport provider name and ID number missing
Prevention: When a provider refers a member to another provider, include the referring provider’s name and ID number or Passport number (see the Passport chapter in this manual).
Claim Error: Prior authorization number missing
Prevention: When prior authorization (PA) is required for a service, the PA number must be on the claim (see the Prior Authorization chapter in this manual).
Claim Error: Not enough information regarding other coverage
Prevention: Fields 1a and 11d are required fields when a member has other coverage (see examples earlier in this chapter).
Claim Error: Authorized signature missing
Prevention: Each claim must have an authorized signature belonging to the provider, billing clerk, or office personnel. The signature may be typed, stamped, or handwritten.
Claim Error: Signature date missing
Prevention: Each claim must have a signature date.
Claim Error: Incorrect claim form used
Prevention: Services covered in this manual require a CMS-1500 claim form.
Claim Error: Information on claim form not legible
Prevention: Information on the claim form must be legible. Use dark ink and center the information in the field. Information must not be obscured by lines.
Claim Error: Medicare EOMB not attached
Prevention: When Medicare is involved in payment on a claim, the Medicare EOMB must be submitted with the claim or it will be denied.
Other Programs
This chapter applies to claims completed for HMK eyeglass services. This chapter does not apply to HMK optometric services because they are covered by Blue Cross and Blue Shield of Montana.
End of Submitting a Claim Chapter
Remittance Advices and Adjustments
The Remittance Advice
The remittance advice is the best tool providers have to determine the status of a claim. Remittance advices accompany payment for services rendered and provide details of all transactions that have occurred during the previous remittance advice cycle.
Each line of the remittance advice represents all or part of a claim and explains whether the claim or service has been paid, denied, or suspended (also referred to as pending). If the claim was suspended or denied, the remittance advice shows the reason.
Providers may receive the remittance advice electronically as an ANSI ASC X12 835 transaction, or once registered with the Montana Access to Health (MATH) web portal, they may receive remittance advices through the web portal.
To register for the MATH web portal and receive electronic remittance advices (ERAs), providers must complete the Trading Partner Agreement available on the Provider Enrollment page of the Provider Information website.
After this form has been processed, you will receive a password. Entry into the system requires a valid provider or group number and password. Each provider or group number requires a unique password, so providers must complete a separate request form for each provider or group.
Remittance advices are available from the MATH web portal in PDF format.
Electronic remittance advices (ERAs) are available on the MATH web portal for 90 days.
Due to space limitations, ERAs are available for 90 days.
Credit Balance Claims
Credit balance claims are shown until the credit has been satisfied.
Credit balances occur when claim adjustments reduce original payments causing the provider to owe money to the Department. These claims are considered in process and continue to appear on the remittance advice until the credit has been satisfied.
Credit balances can be resolved in two ways:
- By working off” the credit balance. Remaining credit balances can be deducted from future claims. These claims continue to appear on consecutive remittance advices until the credit has been paid.
- By sending a check payable to DPHHS for the amount owed. This method is required for providers who no longer submit claims to Montana Healthcare Programs. Include your NPI and indicate that the check is to pay off a credit balance. Send to the Third Party Liability unit. See the Contact Us page on the Provider Information website.
Rebilling and Adjustments
Rebillings and adjustments are important steps in correcting any billing problems you may experience. Knowing when to use the rebilling process versus the adjustment process is important.
Timeframe for Rebilling or Adjusting a Claim
- Providers may resubmit or adjust any initial claim within the timely filing limits described in the Billing Procedures chapter of this manual.
- These time periods do not apply to overpayments that the provider must refund to the Department. After the 12-month time period, a provider may not refund overpayments to the Department by completing a claim adjustment. The provider may refund overpayments by issuing a check or requesting a gross adjustment be made.
Rebilling Montana Healthcare Programs
Rebilling occurs when a provider submits a claim/claim line to Montana Healthcare Programs that was previously submitted for payment but was returned/denied. Claims are often returned to the provider before processing because information (e.g., provider NPI, authorized signature, date) is missing or unreadable. (See the Billing Procedures and Submitting a Claim chapters.)
When to Rebill Montana Healthcare Programs
- Claim Denied. Providers can rebill Montana Healthcare Programs when a claim is denied in full, as long as the claim was denied for reasons that can be corrected. When the entire claim is denied, check the Explanation of Benefits (EOB) code, make the appropriate corrections, and resubmit the corrected claim on a CMS-1500 form (not the Individual Adjustment form).
- Line Denied. When an individual line is denied on a multiple-line claim, correct any errors and rebill Montana Healthcare Programs. Either submit the denied service on a new CMS-1500 form, or cross out paid lines and resubmit the form. Do not use an Individual Adjustment form.
- Claim Returned. Rebill Montana Healthcare Programs when the claim is returned under separate cover. Occasionally, Montana Healthcare Programs is unable to process the claim and returns it to the provider with a letter indicating additional information is needed to process the claim. Correct the claim as directed and resubmit it.
How to Rebill
- Check any EOB code listed and make your corrections on a copy of the claim, or produce a new claim with the correct information.
- When making corrections on a copy of the claim, remember to cross out or omit all lines that have already been paid. The claim must be neat and legible for processing.
- Enter any insurance (third party liability) information on the corrected claim, or attach insurance denial information to the corrected claim, and send it to the Claims unit. See the Contact Us page of the Provider Information website.
Adjustments
If a provider believes that a claim has been paid incorrectly, the provider may call Provider Relations. Once an incorrect payment has been verified, the provider should submit an Individual Adjustment Request form to Provider Relations. If incorrect payment was the result of a Claims keying error, contact Provider Relations.
When adjustments are made to previously paid claims, the Department recovers the original payment and issues appropriate repayment. The result of the adjustment appears on the provider’s remittance advice as two transactions. The original payment will appear as a credit transaction. The replacement claim reflecting the corrections will be listed as a separate transaction and may or may not appear on the same remittance advice as the credit transaction. The replacement transaction will have nearly the same ICN number as the credit transaction, except the 12th digit will be a 2, indicating an adjustment. Adjustments are processed in the same time frame as claims.
When to Request an Adjustment
- Request an adjustment when a claim was overpaid or underpaid.
- Request an adjustment when a claim was paid but the information (e.g., member ID, provider NPI, date of service, procedure code, diagnoses, units) on the claim was incorrect.
How to Request an Adjustment
To request an adjustment, use Individual Adjustment Request form on the Forms page of the Provider Information website. The requirements for adjusting a claim are as follows:
- Claims Processing must receive individual claim adjustment requests within 12 months from the date of service. (See Timely Filing Limits in the Billing Procedures chapter.) After this time, gross adjustments are required.
- Use a separate adjustment request form for each ICN.
- If you are correcting more than one error per ICN, use only one adjustment request form, and include each error on the form.
Payment and the Remittance Advice
Providers receive their Montana Healthcare Programs payment and remittance advices electronically. Payment is via electronic funds transfer (EFT). Direct deposit is another name for EFT. Remittance advices are available through the MATH web portal for 90 days.
With EFT, the Department deposits the funds directly to the provider’s bank account. If the scheduled deposit day is a holiday, payments and ERAs will be available on the next business day.
To participate in EFT and receive ERAs, providers must complete the Montana Healthcare Programs Electronic Funds Transfer (EFT) and Electronic Remittance Advice (ERA) Authorization Agreement. In addition, a letter from the provider’s financial institution is required, and Passport providers have additional requirements. Contact Provider Relations for assistance.
Once electronic transfer testing shows payment to the provider’s account, Montana Healthcare Programs payments will be made through EFT. Contact Montana Provider Relations if you have questions.
Required Forms for EFT and ERA
Form: Montana Healthcare Programs Electronic Funds Transfer (EFT) & Electronic Remittance Advice (ERA) Authorization Agreement
Purpose: Allows the Department to automatically deposit Montana Healthcare Programs payment into provider’s bank account.
Where to Get: Provider Information website.
Form: Trading Partner Agreement
Purpose: Allows provider to access their ERA on the Montana Access to Health web portal (must also include the form above).
Where to Get: Provider Information website.
Form: Letter from the provider’s financial institution verifying the account number and routing number. Do not send voided checks or deposit slips.
Purpose: Paperwork requirement.
Where to Get: Your financial institution.
All forms should be faxed to Provider Relations (406) 442-4402.
Other Programs
The information in this chapter applies to the Healthy Montana Kids Program (HMK) eyeglasses only. Optometric services are covered under the HMK plan of Blue Cross and Blue Shield of Montana.
End of Remittance Advices and Adjustments Chapter
How Payment Is Calculated
Overview
Though providers do not need the information in this chapter in order to submit claims to the Department, the information allows providers to understand how payment is calculated and to predict approximate payment for particular claims.
The RBRVS Fee Schedule
Most services provided by optometrists, opticians, and ophthalmologists are paid for using the Department’s Resource-Based Relative Value Scale (RBRVS) fee schedule, which includes approximately 10,230 CPT codes, approximately 2,670 HCPCS codes.
RBRVS was developed for the Medicare program and implemented in 1992. Medicare does a major update annually, with smaller updates performed quarterly. Montana Healthcare Programs implemented its RBRVS-based fee schedule in August 1997. It is based largely on the Medicare model, with a few differences that are described below. By adapting the Medicare model to the needs of the Montana Healthcare Programs program, the Department was able to take advantage of the millions of dollars of research performed by the federal government and national associations of physicians and other healthcare professionals. RBRVS-based payment methods are widely used across the U.S. by Montana Healthcare Programs programs, Blue Cross and Blue Shield plans, workers’ compensation plans and commercial insurers.
Many Montana Healthcare Programs payment methods are based on Medicare, but there are differences, in these cases, the Montana Healthcare Programs method prevails.
The following paragraphs elaborate on aspects of the RBRVS fee schedule used by the Department.
Fee Calculation
Each fee is the product of a relative value times a conversion factor.
When Montana Healthcare Programs payment differs from the fee schedule, consider the following:
- The Department pays the lower of the established Montana Healthcare Programs fee or the provider’s charge
- Modifiers. See Other Modifiers in this chapter.
- Provider type. See Professional Differentials in this chapter.
- Place of service. See Site of Service Differential in this chapter.
- Date of service (fees for services may change over time).
- Also check for cost sharing and Medicare or TPL payments which will be shown on the remittance advice.
Basis of Relative Values
For almost all services, Montana Healthcare Programs uses the same relative values as Medicare does in Montana. (Nationally, Medicare adjusts the relative values for differences in practice costs between localities, but Montana is considered a single locality.) For fewer than 1% of codes, relative values are not available from Medicare. For these codes, the Department has set the relative values.
Composition of Relative Values
For each code, the relative value is the sum of a relative value for the work effort (including time, stress, and difficulty), the associated practice expense, and the associated malpractice expense.
Site of Service Differential
The Medicare program has calculated two sets of relative values for each code: one that reflects the practitioner’s practice cost of performing the service in an office and one that reflects the practitioner’s practice cost of performing the service in a hospital or ambulatory surgical center (ASC). When services are provided within a hospital or ASC (i.e., places of service 21, 22, 23, and 24), Montana Healthcare Programs typically pays a lower fee than if the service is provided in the office or another setting. The reason is that Montana Healthcare Programs typically also pays the hospital or ASC for the service.
Conversion Factor
The Department sets the conversion factor for the state fiscal year (July through June). The conversion factor is typically reviewed (and often changed) in July of each year.
Transition Adjustor
Because the move to an RBRVS-based fee schedule resulted in large changes in fees for some services, the Montana legislature directed the Department to pay transitional fees for about 2,250 of the 9,300 services covered by the fee schedule. For about 900 services, the transitional fee is lower than it otherwise would be; for 1,350 services, it is higher than it otherwise would be. The transitional fees are put in place by a transition adjustor.
Global Periods
For many surgical services, the fee covers both the service and all related care within a specified global period. For almost all such codes, the global periods used by Montana Healthcare Programs are identical to those used by Medicare, but in cases of differences the Montana Healthcare Programs policy applies. See the Billing Procedures chapter in this manual for more information on global periods.
Professional and Technical Components
Some services are divided into the technical component (performing the test) and the professional component (interpreting the test). A practitioner who only performs the test would bill the service with modifier TC; a practitioner who only interprets the test would bill with Modifier 26; and a practitioner who performs both components (referred to as a global service) would bill the code without a modifier. The fee schedule has separate fees for each component and for the global service.
Other Modifiers
Under the RBRVS fee schedule, certain other modifiers also affect payment.
How Modifiers Change Pricing
- Modifiers may not be applicable for all services. For services paid via the RBRVS fee schedule, the fee schedule shows the list of services for which Modifiers 26, TC, 50, 51, 62, and 80 apply.
- If a modifier does not appear in this list, then it does not affect pricing for Optometric and Eyeglass Services.
- The list shows summary modifier descriptions. See the CPT and HCPCS coding books for the full text.
Modifier: 22 Definition: Increased procedural service
How Payment Is Affected: The service is paid at 110% of fee.
Modifier: 26 Definition: Professional component
How Payment Is Affected: For services paid via the RBRVS fee schedule, see the specific service. For other services, payment equals 40% of the fee.
Modifier: 50 Definition: Bilateral procedure
How Payment Is Affected: The procedure is paid at 150% of the fee.
Modifier: 51 Definition: Multiple procedures
How Payment Is Affected: Each procedure is paid at 50% of the fee.
Modifier: 52 Definition: Reduced service
How Payment Is Affected: The service is paid at 50% of the fee.
Modifier: 53 Definition: Discontinued procedure
How Payment Is Affected: The service is paid at 50% of the fee.
Modifier: 54 Definition: Surgical care only
How Payment Is Affected: The service is paid at 75% of the fee.
Modifier: 55 Definition: Postoperative management only
How Payment Is Affected: The service is paid at 25% of the fee.
Modifier: 56 Definition: Preoperative management only
How Payment Is Affected: The service is paid at 25% of the fee.
Modifier: 62 Definition: Two surgeons
How Payment Is Affected: Each surgeon is paid at 62.5% of the fee.
Modifier: 80 Definition: Assistant surgeon
How Payment Is Affected: The service is paid at 16% of the fee.
Modifier: 81 Definition: Minimum assistant surgeon
How Payment Is Affected: The service is paid at 16% of the fee.
Modifier: 82 Definition: Assistant surgeon; qualified resident surgeon not available
How Payment Is Affected: The service is paid at 16% of the fee.
Modifier: 90 Definition: Reference laboratory
How Payment Is Affected: Modifier not allowed.
Modifier: AD Definition: Medical supervision of more than four concurrent anesthesia procedures
How Payment Is Affected: Each service is paid at 52.5% of the fee.
Modifier: AS Definition: Physician assistant, nurse practitioner or clinical nurse specialist as assistant at surgery
How Payment Is Affected: The service is paid at 16% of the fee.
Modifier: QK Definition: Medical supervision of 2--4 concurrent anesthesia procedures
How Payment Is Affected: Each service is paid at 52.5% of the fee.
Modifier: QX Definition: Certified registered nurse anesthetist service: medically directed by medical doctor.
How Payment Is Affected: Each service is paid at 52.5% of the fee.
Modifier: QZ Definition: Certified registered nurse anesthetist service without medical direction
How Payment Is Affected: The modifier does not reduce the fee, but a professional differential of 90% is applied due to provider type. See Professional Differentials below.
Modifier: TC Definition: Technical component
How Payment Is Affected: For services paid via the RBRVS fee schedule, see the specific service. For other services, payment equals 60% of the fee.
Modifier: U4 Definition: For Lenses only, due to change in RX
How Payment Is Affected: The modifier will allow a fitting procedure to be reimbursed if performed sooner than the allowed time frame.
Professional Differentials
For some services within the scope of RBRVS payment methods, mid-level practitioners are paid differently; however, optometrists, ophthalmologists, and opticians are always paid at 100% of the fee schedule.
Bundled Codes
A few services are covered by the Department but have a fee of zero, meaning that payment for the service is considered bundled into the payment for services that are usually provided with it. Examples are temporary tear duct plug, permanent tear duct plug, and special spectacles fitting. Because these services are covered by Montana Healthcare Programs , providers may not bill members for them on a private pay basis.
Status Codes
The RBRVS fee schedule includes status codes that show how each service is paid. The list of status codes is based on that used by Medicare, as shown in the table on the next page.
Medicare and Montana Healthcare Programs RBRVS Status Values
Medicare Status: A - Active code paid using RVUs
Montana Healthcare Programs Status: A - Active code paid using RVUs set by Medicare
Medicare Status: B - Bundled code
Montana Healthcare Programs Status: B - Bundled code
Medicare Status: C - Carrier determines coverage and payment
Montana Healthcare Programs Status: C - Pay by report
Medicare Status: D - Deleted code
Montana Healthcare Programs Status: D - Discontinued code
Medicare Status: E - Excluded from fee schedule by regulation
Montana Healthcare Programs Status: - [Montana Healthcare Programs reviews each code and usually assigns A, K, or X status]
Medicare Status: F - Deleted/discontinued code; no grace period
Montana Healthcare Programs Status: D - [Assigned to D status]
Medicare Status: G - Use another code; grace period allowed
Montana Healthcare Programs Status: G - Use another code; grace period set code-by-code
Medicare Status: H - Modifier deleted
Montana Healthcare Programs Status: - [Assigned to D status]
Medicare Status: I - Use another code; no grace period
Montana Healthcare Programs Status: - [Assigned to G status]
Montana Healthcare Programs Status: J - Anesthesia code
Montana Healthcare Programs Status: K - Active code paid using RVUs set by Montana Healthcare Programs
Montana Healthcare Programs Status: L - Not paid via RBRVS. See lab fee schedule.
Montana Healthcare Programs Status: M - Not paid via RBRVS. See non-RBRVS fee schedule.
Medicare Status: N - Excluded from fee schedule by policy
Montana Healthcare Programs Status: - [Montana Healthcare Programs reviews each code and usually assigns A, K, or X status]
Medicare Status: P - Bundled or excluded
Montana Healthcare Programs Status: - [Montana Healthcare Programs reviews each code and usually assigns B or X status]
Medicare Status: R - Restricted coverage
Montana Healthcare Programs Status: - [Montana Healthcare Programs reviews each code and usually assigns A or K status]
Medicare Status: T - Injections
Montana Healthcare Programs Status: - [Montana Healthcare Programs reviews each code and usually assigns A status]
Medicare Status: X - Excluded from fee schedule by statute
Montana Healthcare Programs Status: X - Not covered
Medicare publishes RVUs for codes that have Medicare status values of R and sometimes publishes RVUs for codes with status values of E, N, or X. Medicare uses the label “injections” for status T but now uses the code for other situations (e.g., pulse oximetry) where Medicare pays for the service only if no other service is performed on the same day.
Payment for Eyeglasses
Payment for eyeglasses is through a single volume purchase contract issued by the Department through the competitive Request for Proposal (RFP) process.
How Cost Sharing Is Calculated on Montana Healthcare Programs Claims
Member cost sharing fees are a set dollar amount per visit based on the average Montana Healthcare Programs allowed amount for the provider type and rounded to the nearest dollar. There is no cost sharing cap. The member’s cost sharing amount is shown on the remittance advice and deducted from the Montana Healthcare Programs allowed amount. See the Billing Procedures and Remittance Advices and Adjustments chapters.
How Payment Is Calculated on TPL Claims
When a member has coverage from both Montana Healthcare Programs and another insurance company, the other insurance company is often referred to as third party liability (TPL). In these cases, the other insurance is the primary payer (as described in the Coordination of Benefits chapter of this manual), and Montana Healthcare Programs makes a payment as the secondary payer.
How Payment Is Calculated on Medicare Crossover Claims
When a member has coverage from both Montana Healthcare Programs and Medicare, Medicare is the primary payer as described in the Coordination of Benefits chapter of this manual. Montana Healthcare Programs then makes a payment as the secondary payer. For the provider types covered in this manual, Montana Healthcare Programs ’s payment is calculated so that the total payment to the provider is either the Montana Healthcare Programs allowed amount less the Medicare paid amount or the sum of the Medicare coinsurance and deductible, whichever is lower. This method is sometimes called lower of pricing.
Other Programs
The payment method described in this chapter applies to eyeglass services for Healthy Montana Kids (HMK). This chapter does not apply to HMK optometric services, which are covered by Blue Cross and Blue Shield of Montana. For more information on HMK, visit the HMK website.
End of How Payment is Calculated Chapter
Appendix A: Forms
- Eyeglass Additional Feature and Contact Lens Prior Authorization Request
- Montana Individual Adjustment Request
- Paperwork Attachment Cover Sheet
End of Appendix A: Forms Chapter
Appendix B: Place of Service Codes
Place of Service Codes are two-digit codes placed on healthcare professional claims to indicate the setting in which a service was provided.
The Centers for Medicare and Medicaid CMS) maintain POS codes used throughout the healthcare industry.
Refer to http://cms.hhs.gov/Medicare/Coding/place-of-service-codes/index.html.
End of Appendix B: Place of Service Codes Chapter
Definitions and Acronyms
End of Definitions and Acronyms Chapter
Search Options
Previous editions of this manual contained an index.
This edition has three search options.
1. Search the whole manual. Open the Complete Manual pane. From your keyboard press the Ctrl and F keys at the same time. A search box will appear. Type in a descriptive or key word (for example "Denials". The search box will show all locations where denials discussed in the manual.
2. Search by Chapter. Open any Chapter tab (for example the "Billing Procedures" tab). From your keyboard press the Ctrl and F keys at the same time. A search box will appear. Type in a descriptive or key word (for example "Denials". The search box will show where denials discussed in just that chapter.
3. Site Search. Search the manual as well as other documents related to a particular search term on the Montana Healthcare Programs Site Specific Search page.
End of Search Options Chapter
End of Optometric and Eyeglass Services Manual
Update Log
Publication History
This publication supersedes all previous Optometric and Eyeglass Services provider handbooks. Published by the Montana Department of Public Health & Human Services, March 2003.
Updated July 2003, April 2004, January 2005, April 2005, August 2005, October 2005, April 2006, April 2010, May 2010, July 2014, May 2015, January 2016, April 2017,October 2017, March 2018, June 2018, January 2020, and April 2022.
CPT codes, descriptions and other data only are copyright 1999 American Medical Association (or such other date of publication of CPT). All Rights Reserved. Applicable FARS/DFARS Apply.
Update Log
04/12/2022
- Removed Nurse First Advice Line references.
- Updated Index to Search Options.
01/01/2020
- Cost Share references removed from Covered Services, Billing Procedures, and Submitting A Claim Chapters.
- Term "medicaid " replaced with "Montana Healthcare Programs" throughout the manual.
- Terms "client" and "patient" replaced with "member".
06/04/2018
Removed commercial resource references.
03/30/2018
Updated Covered Services and Billing Procedures chapters with new time requirements for services.
10/18/2017
Optometric and Eyeglass Services Manual converted to an HTML format and adapted to 508 Accessibility Standards.
04/10/2017
Optometric and Eyeglass Services, April 2017
In summary, the manual was updated to include current cost share language and co-pays and basic accessibility changes were made as approved by the Manuals Committee in September 2016.
12/31/2015
Optometric and Eyeglass Services, January 2016: HELP Plan-Related Updates and Others
06/24/2015
Optometric and Eyeglass Services, June 2015: Entire Manual
(Note: There are pages that have no text changes; however, the page layout is different than the previous manual due to changes on previous pages.)
08/11/2014
Entire Optometric and Eyeglass Services Manual
Information contained in the General Information for Providers manual or found elsewhere on the website has been removed, and links to those sources are included.
05/19/2010
Key Contacts and Prior Authorization
04/25/2006
Covered Services Information for Initial/New Prescriptions for Eyeglasses
10/12/2005
Covered Services Information for Initial/New Prescriptions
09/09/2005
Eyeglass Service Modifiers, New Place of Service Codes
04/18/2005
Clarification for Lens Add-Ons and Updated Key Contacts
01/19/2005
Rule References Added
04/29/2004
Updates for HIPAA, Covered Services, and Billing Procedures
07/09/2003
Covered Services
End of Update Log Chapter
Table of Contents
Key Websites
Introduction
Manual Organization
Manual Maintenance
Rule References
Claim Review (MCA 53-6-111, ARM 37.85.406)
Getting Questions Answered
Other Department Programs
Covered Services
General Coverage Principles
- Services within scope of practice (ARM 37.85.401)
- Licensing
- Services for children (ARM 37.86.2201 - 2221)
Noncovered Services (ARM 37.85.207)
Coverage of Specific Services
Verifying Coverage
Prior Authorization
Coordination of Benefits
When members Have Other Coverage
Identifying Additional Coverage
When a member Has Medicare
- Medicare Part B crossover claims
When a member Has TPL (ARM 37.85.407)
- Exceptions to billing third party first
- Requesting an exemption
- When the third party pays or denies a service
- When the third party does not respond
Billing Procedures
Claim Forms
Timely Filing Limits (ARM 37.85.406)
- Tips to avoid timely filing denials
When to Bill Montana Healthcare Programs members (ARM 37.85.406)
Member Cost Sharing (ARM 37.85.204)
When members Have Other Insurance
Billing for Retroactively Eligible members
Usual and Customary Charge (ARM 37.85.406)
Coding
Using the Montana Healthcare Programs Fee Schedule
Using Modifiers
The Most Common Billing Errors and How to Avoid Them
Submitting a Claim
Electronic Claims
Billing Electronically with Paper Attachments
Paper Claims
Member Has Montana Healthcare Programs Coverage Only
Member Has Montana Healthcare Programs and Third Party Liability Coverage
CMS-1500 Agreement
Remittance Advices and Adjustments
The Remittance Advice
- Electronic Remittance Advice
- Paper RA
Sample Remittance Advice
- Credit balance claims
Rebilling and Adjustments
- How long do I have to rebill or adjust a claim?
- Rebilling Montana Healthcare Programs
- When to rebill Montana Healthcare Programs
- How to rebill
- Adjustments
- When to request an adjustment
- Completing an Adjustment Request Form
- Mass adjustments
Payment and the RA
How Payment Is Calculated
Overview
How Payment is Calculated on TPL Claims
How Payment is Calculated on Medicare Crossover Claims
Other Factors That May Affect Payment
Appendix A: Forms
Claim Inquiry Form
Individual Adjustment Request
Paperwork Attachment Cover Sheet
Appendix B: Place of Service Codes
Definitions and Acronyms
Index
End of Table of Contents Chapter
Key Contacts
Hours for contacts are 8 a.m. to 5 p.m. Monday through Friday (Mountain Time), unless otherwise stated. The phone numbers designated only “In-state” will not work outside Montana. For additional contacts and a list of key websites, choose the Contact Us link in the left menu on the Provider Information website.
Eyeglass Contractor
Classic Optical Laboratories is contracted with DPHHS to provide eyeglasses to Montana Healthcare Programs members and
HMK members. Providers should call Classic Optical to verify the member is eligible for eyeglasses.
Classic’s contact information is:
Classic Optical Customer Service
3710 Belmont Avenue
P.O. Box 1341 (44501)
Youngstown, OH 44505
(888) 522-2020 Phone
Ext: 1316 - customer service
(888) 522-2022 Fax
HMK Eyeglass Services
HMK Eyeglass Services
P.O. Box 202951
Helena, MT 59620-2951
(877) 543-7669 Toll-free in-state
(406) 444-7045 Phone
(406) 444-1861 Fax
hmk@mt.gov
HMK Optometric Services
Blue Cross and Blue Shield of Montana processes optometric services for HMK members. For more information or a billing manual, contact:
Healthy Montana Kids
Blue Cross and Blue Shield of Montana
P.O. Box 4309
Helena, MT 59604
(800) 447-7828, X8647
(406) 447-8647
Optometric Program Officers
Providers should refer to their specific provider manual for prior authorization instructions.
Contact Montana Provider Relations to verify the member is eligible for eye exams.
Contact DPHHS for prior authorization for transition lenses, tints other than Rose 1 and Rose 2, UV and scratch resistant coating, polycarbonate lenses, and deluxe frames for Montana Healthcare Programs and HMK members
For Montana Healthcare Programs members:
(406) 444-4066 Phone
(406) 444-1861 Fax
Optometric Program Officer
Allied Health Services Bureau
P.O. Box 202951
Helena, MT 59620-2951
For HMK members:
877-543-7669 Toll-free, in-state callers
406-444-7045 Phone
406-444-1861 Fax
hmk@mt.gov
HMK Eyeglass Services
P.O. Box 202951
Helena, MT 59620-2951
End of Key Contacts Chapter
Introduction
Thank you for your willingness to serve members of the Montana Healthcare Program and other medical assistance programs administered by the Department of Public Health and Human Services.
Manual Organization
This manual provides information specifically for optometrists, opticians, and ophthalmologists. Other information for ophthalmologists is included in the Physician-Related Services manual.
Most chapters have a section titled Other Programs that includes information about other Department programs such as the Mental Health Services Plan (MHSP) and the Healthy Montana Kids Program (HMK). Other essential information for providers is contained in the separate General Information for Providers manual. Each provider is asked to review both the general manual and the specific manual for his/her provider type.
A table of contents and an index allow you to quickly find answers to most questions. The margins contain important notes with extra space for writing notes. There is a list of contacts at the beginning of this manual and on the Contact Us page on the Provider Information website. There is space on the inside of the front cover to record your NPI and HMK provider ID numbers for quick reference when calling Provider Relations.
Manual Maintenance
Manuals must be kept current. Changes are provided through provider notices and replacement pages, which are available on the Provider Information website. When replacing a page in a manual, file the old pages in the back of the manual for use with claims that originated under the old policy.
Rule References
Providers must be familiar with all current rules and regulations governing the Montana Healthcare Program. Provider manuals are to assist providers in billing Montana Healthcare Programs; they do not contain all Montana Healthcare Programs rules and regulations. Rule citations in the text are a reference tool; they are not a summary of the entire rule. In the event that a manual conflicts with a rule, the rule prevails. Links to rules are available on the Provider Information website and paper copies of rules are available through the Secretary of State’s office. (See the Contact Us page on the Provider Information website.)
Providers are responsible for knowing and following current Montana Healthcare Programs rules and regulations.
In addition to the Montana Healthcare Programs rules outlined in the General Information for Providers manual, the following rules and regulations are also applicable to the optometric and eyeglass programs:
- Code of Federal Regulations (CFR)
- 42 CFR 440.60 Montana Healthcare Programs or Other Remedial Care Provided by Licensed Practitioners
- 42 CFR 440.120 Prescribed Drugs, Dentures, Prosthetic Devices and Eyeglasses
- Montana Codes Annotated (MCA)
- MCA 37-10-101 through MCA 37-10-313 Optometry
- Administrative Rules of Montana (ARM)
- ARM 37.86.2001 through ARM 37.86.2005 Optometric
- ARM 37.86.2101 through ARM 37.86.2105 Eyeglasses
Claims Review (MCA 53-6-111 and ARM 37.85.406)
The Department is committed to paying Montana Healthcare Programs providers’ claims as quickly as possible. Montana Healthcare Programs claims are electronically processed and usually are not reviewed by medical experts prior to payment to determine if the services provided were appropriately billed. Although the computerized system can detect and deny some erroneous claims, there are many erroneous claims which it cannot detect. For this reason, payment of a claim does not mean that the service was correctly billed or the payment made to the provider was correct. Periodic retrospective reviews are performed which may lead to the discovery of incorrect billing or incorrect payment. If a claim is paid and the Department later discovers that the service was incorrectly billed or paid or the claim was erroneous in some other way, the Department is required by federal regulation to recover any overpayment, regardless of whether the incorrect payment was the result of Department or provider error or other cause.
Getting Questions Answered
The provider manuals are designed to answer most questions; however, questions may arise that require a call to a specific group (such as Provider Relations or a prior authorization unit). The list of at the front of this manual has important phone numbers and addresses pertaining to this manual. Additional contacts and websites are on the Contact Us page of the website. Providers should also read the monthly Claim Jumper newsletter for Montana Healthcare Programs updates and changes. Montana Healthcare Programs provider manuals, provider notices, replacement pages, fee schedules, forms, and more are available on the Provider Information website.
End of Introduction Chapter
Covered Services
General Coverage Principles
This chapter provides covered services information that applies specifically to optometrists, opticians, and ophthalmologists. It also covers information for the prescription of corrective lenses. Like all healthcare services received by Montana Healthcare Programs members, services provided by these practitioners must also meet the general requirements listed in the Provider Requirements chapter of the General Information for Providers manual. Ophthalmologists should also be familiar with the Physician-Related Services manual.
Services within Scope of Practice (ARM 37.85.401 and ARM 37.86.2001)
Services are covered when they are within the scope of the provider’s practice.
Dispensing Services (ARM 37.86.2102)
Dispensing services may be provided by ophthalmologists, optometrists, and opticians. Employees may also dispense if the provider complies with laws, rules, and licensing requirements regarding supervision and assistants or aides.
Services for Members with Limited Montana Healthcare Programs Coverage
Montana Healthcare Programs generally does not cover eye exams or eyeglasses for members with QMB only coverage. Always check member eligibility before providing services. For limits, see the General Information for Providers manual, Member Eligibility chapter; and Eye Exams and Eyeglass Services in this chapter. Montana Healthcare Programs may cover eye exams for members with QMB only coverage under the following conditions.
- Following cataract surgery. Members who have QMB only coverage are only eligible for eyeglasses following cataract surgery when Medicare approves the eyeglasses claim. Montana Healthcare Programs considers the Medicare coinsurance and deductible for this claim. Eyeglasses for these members are not provided through the Department’s eyeglass contractor but through Medicare’s purchasing plan. See the Coordination of Benefits chapter in this manual for more information.
- Diabetic diagnosis. Montana Healthcare Programs covers eye exams once every 365 days for members who have a diabetic diagnosis.
- Some optometric diagnostic conditions may be billed to Montana Healthcare Programs first. In these cases, Montana Healthcare Programs will “pay-and-chase” or recover payment itself from the third party payer.
Services for Children (ARM 37.86.2201–2235)
The Early and Periodic Screening, Diagnostic, and Treatment (EPSDT) Services program is a comprehensive approach to healthcare for Montana Healthcare Programs members age 20 and under. It is designed to prevent, identify, and then treat health problems before they become disabling. Under EPSDT, Montana Healthcare Programs eligible children may receive any medically necessary covered service, including all eye exam and eyeglass services described in this manual. All applicable Passport to Health and prior authorization requirements apply.
Non-Covered Services (ARM 37.85.206, ARM 37.85.207, ARM 37.85.406)
Some services not covered by Montana Healthcare Programs include the following:
- Services considered experimental or investigational
- Dispensing fees for a member who is not eligible for lenses and/or frames within the 760-day time period
- Services that the provider did not personally provide. The main exception is that the dispensing service may be performed by the provider’s employee when it is allowed by law.
Importance of Fee Schedules
The easiest way to verify coverage for a specific service is to check the Department’s fee schedule. Fee schedules list Montana Healthcare Programs covered codes and provide clarification of indicators such as whether a code requires prior authorization, can be applied to a co-surgery, can be billed bilaterally, etc. All services provided must also meet the coverage criteria listed in the Provider Requirements chapter of the General Information for Providers manual and in this chapter. Use the fee schedule in conjunction with the more detailed coding descriptions listed in the current CPT and HCPCS coding books. Take care to use the fee schedule and coding books that pertain to the date of service. Fee schedules are available on the Provider Information website.
Retroactive Eligibility
Montana Healthcare Programs does not cover eyeglasses for members who become retroactively eligible for Montana Healthcare Programs when the eyeglasses were purchased before retroactive eligibility was determined. However, Montana Healthcare Programs does cover eye exams for retroactively eligible members. For example, suppose that a member had an eye exam and purchased eyeglasses on July 15. On September 1, the Department determined the member was eligible for Montana Healthcare Programs retroactive to July 1. Montana Healthcare Programs would pay for the eye exam but not for the eyeglasses.
Use the current fee schedule for your provider type to verify coverage for specific services.
Coverage of Specific Services
The following are coverage rules for specific services provided by optometrists, opticians, and ophthalmologists. Due to limits on exams and eyeglasses, before providing these services, the provider should contact Provider Relations to verify the member is currently eligible for an exam, and contact the eyeglass contractor to verify the member is eligible for eyeglasses. Montana Healthcare Programs will only pay for eyeglasses and frames purchased through the Department’s eyeglass contractor. All services are subject to post payment review and payment recovery if they are not medically necessary. (See the Surveillance and Utilization Review chapter in the General Information for Providers manual.)
Montana Healthcare Programs will only pay for eyeglasses and frames purchased through the Department’s eyeglass contractor.
Contact Lenses
Contact lenses are covered only when medically necessary and not for cosmetic reasons. Dispensing providers must obtain prior authorization for all contact fitting, contact lenses and dispensing fees. (See the Prior Authorization chapter in this manual.) The same limits that apply to eyeglasses and repairs also apply to contacts. Contact lenses are not provided by the eyeglass contractor and therefore may be provided by other providers. Montana Healthcare Programs covers them when the member has one the following conditions:
- Keratoconus
- Sight that cannot be corrected to 20/40 with eyeglasses
- Aphakia
- Anisometropia of 2 diopters or more
Eye Exams
Before providing an eye exam, verify that the member is eligible for an exam by contacting Provider Relations. Montana Healthcare Programs members age 21 or over are limited to one eye examination for determining refractive state every 730 days. Montana Healthcare Programs members ages 20 or under are limited to one eye examination for determining refractive state every 365 days. See Eyeglass Services in the Billing Procedures chapter of this manual for details on how to bill.
The Department allows exceptions to these limits when one of the following conditions exists:
- Following cataract surgery, when more than one exam during the respective period is necessary.
- A screening shows a loss of one line acuity with present eyeglasses.
- Adult diabetic members may have exams every 365 days.
If a provider does not check member eligibility prior to an exam, and the claim is denied because the member’s exam limit was exceeded, the provider cannot bill Montana Healthcare Programs or the member.
Eyeglass Services
Before providing eyeglasses to a member, verify that the member is eligible by contacting Montana Provider Relations for exam and eyeglass frequency. Adults ages 21 or older are eligible for eyeglasses every 730 days. If the member has a diagnosed medical condition that prohibits the use of bifocals, Montana Healthcare Programs may cover two pairs of single vision eyeglasses every 365 days. Prior authorization is not required, but the provider must document the member’s inability to use bifocals and request a verbal approval from the Department Program Office. Children age 20 or under are eligible for eyeglasses every 365 days. If one of the following circumstances exists for one eye, within the respective time limits, lenses only will be replaced.
Adults (age 21 and older) are limited to one eye exam and one pair of eyeglasses every 730 days. Children (ages 20 and under) are limited to one eye exam and one pair of eyeglasses every 365 days.
- .50 diopter change in correction in sphere
- .75 diopter change in cylinder
- .5 prism diopter change in vertical prism
- .50 diopter change in the near reading power
- A minimum of a 5 degree change in axis of any cylinder less than or equal to 3.00 diopters
- A minimum of a 3 degree change in axis of any cylinder greater than 3.00 diopters
- Any 1 prism diopter or more change in lateral prism
If any one of these changes is in one eye, Montana Healthcare Programs will cover that lens only. Montana Healthcare Programs will not cover a new frame at the time of a prescription change within the respective time limits.
Eyeglasses are covered for an initial/new prescription when the member has at least one of the following circumstances in one or both eyes:
- Cataract surgery
- .50 diopter correction in sphere
- .75 diopter correction in cylinder
- .5 prism diopter correction in vertical prism
- .50 diopter correction in near reading power
- Any 1 prism diopter or more correction in lateral prism
Frame Services
The eyeglass contractor will provide a list of Montana Healthcare Programs-covered frames to dispensing providers. Montana Healthcare Programs members have the option of using their existing frames and Montana Healthcare Programs will cover lenses. The existing frame is a frame that the member owns or purchases. When a member chooses to use an existing frame, the following apply:
- Dispensing providers will evaluate existing frames to ensure lenses can be inserted.
- The eyeglass contractor will decide if the existing frame can be used for Montana Healthcare Programs covered lenses. If the existing frame cannot be used, the eyeglass contractor will inform the dispensing provider.
- If the existing frame breaks (after lenses are dispensed to the member), Montana Healthcare Programs will pay for a contract frame but not new lenses. The member can choose to pay privately for new lenses or find a contract frame that the lenses will fit. New lenses are not covered in this case.
Lens Add-Ons
Lens Feature: Photochromic - plastic (i.e., transition)
Children: Yes - if medically necessary
Adults: No
Charge: $18.00
Lens Feature: Photochromic - glass (i.e., photogray, photobrown)
Children: Yes - if medically necessary
Adults: No
Charge: $18.00
Lens Feature: Progressive - no line
Children: No
Adults: No
Charge: $27.00
Lens Feature: Polycarbonate lenses (Single vision, bifocal, or trifocal lenses)
Children: Yes - if member is monocular
Adults: Yes - if member is monocular
Charge: $4.00
Lens Feature: Tints Rose 1 and Rose 2 (applicable to CR-39 and Polycarbonate lenses only)
Children: Yes
Adults: Yes
Charge: No charge
Lens Feature: Deluxe Frames
Children: Yes - if medically necessary
Adults: No
Charge: $30.00
Lens Feature: Round bifocal/plastic only
Children: Yes - if medically necessary
Adults: No
Charge: $7.70
Lens Feature: Tints other than Rose 1 and Rose 2 (applicable to CR-39 and Polycarbonate lenses only)
Children: Yes - if medically necessary
Adults: No
Charge: $2.00
Lens Feature: UV and scratch-resistant coatings
Children: Yes - if medically necessary
Adults: No
Charge: $1.00
Children qualify as ages 20 and under.
Any lens style, lens material, tint, coating lens enhancement (polished edge, etc.) not specifically noted above or within this manual will be billed to the dispensing provider at the eyeglass contractor’s normal and customary charges. The Department requests that providers bill members the Classic Optical Montana Healthcare Programs rate for scratch guard and polycarbonate lenses. For other add-ons noted above that are not covered by Montana Healthcare Programs, payment is a private arrangement between the member and the provider, and the provider may charge the usual private-pay rate or the Classic Optical Montana Healthcare Programs rate to the member.
Lens Styles and Materials
All eyeglass lenses fabricated by the eyeglass contractor for Montana Healthcare Programs members must be in the edged form, edged to shape and size for a specific frame and returned to the dispensing provider as lenses only, or edged and mounted into a specific frame and returned to the dispensing provider as complete Rx order. Orders for uncut lenses are not accepted.
Montana Healthcare Programs covers the following lens styles:
- Single vision
- Flattop segments 25, 28, 35
- Flattop trifocals 7 x 25, 7 x 28, 8 x 35
- Round bifocals 22 and 34
- Executive style bifocals
Montana Healthcare Programs covers the following lens materials (no high index):
- Glass
- CR-39
- Polycarbonate for monocular members only. Montana Healthcare Programs members who are not monocular can choose polycarbonate lenses and pay the difference as an add-on. (See previous table titled Lens Add-Ons.)
Replacement Lenses and Frames
All frames provided by the Montana Healthcare Programs contractor carry a 12-month manufacturer warranty on replacement fronts and temples. Montana Healthcare Programs members must bring their broken frames into the dispensing provider for the contractor to repair. No new frame style or color can replace the broken frame.
If an adult (ages 21 and older) loses his/her eyeglasses within the 12 months, Montana Healthcare Programs will not cover another pair. If an adult’s lenses are broken or unusable, the member is eligible for replacement lenses (not frames) within the first 12 months after the initial dispensing of contract eyeglasses.
If a Montana Healthcare Programs/HMK child (ages 20 and under) loses or breaks the first pair of eyeglasses, and the damage is not covered by the warranty, Montana Healthcare Programs will replace one pair of eyeglasses within the 365 day period. Additional replacement requests must be reviewed by the Department Program Officer. Parents/guardians may purchase additional replacement eyeglasses at the Montana Healthcare Programs contract rate. If a HMK/CHIP (18 & under) member loses or break a pair of eyeglasses, and the damage is not covered by the warranty, HMK will NOT replace the eyeglasses. However, if there is a prescription change that meets criteria amount of change, lenses only will be replaced and not the frame. Members can purchase frames through Classic Optical at the contract price or the dispending providers usual and customary charge.
Eyeglass Ordering Procedures
The Montana contracted provider, Classic Optical, offers an online ordering system to order eyeglasses for Montana Healthcare Programs and HMK members. Dispensing providers need to be signed up with Classic Optical and the website and log-on information will be provided from Classic Optical. The contact phone number for Classic Optical is located in “Key Contacts” at the front of this manual.
When the date of service is near the end of the month, order online or fax orders to the eyeglasses contractor.
Tips for Completing the Classic Optical online order form:
- The date of service for dispensing eyeglasses (measuring, verifying, and fitting) is the date the eyeglasses are ordered from the contractor.
- The date of service for eyeglass materials is the date the order is received by the eyeglass contractor.
- Encounters with the member on and after the date the glasses are dispensed are considered follow-up and are covered within the measuring, verifying, and fitting fee.
- When the date of service is near the end of the month, please complete online or fax orders to the contractor. This will help ensure the member is eligible for eyeglasses since eligibility can change monthly. If you experience any difficulty faxing the contractor, contact the contractor manager immediately. (See Key Contacts.)
- When an order requires a Prior Authorization number from the department and one has been issued, the number needs to be on the order form. The order along with the department’s document of the Prior Authorization number will be faxed to Classic Optical.
- Check the EPSDT box when the Montana Healthcare Programs member is age 20 or under.
- 2nd PR S.V. is used when ordering two pairs of single vision eyeglasses (one for distance and one for reading) when a Montana Healthcare Programs member cannot wear multi-focal eyeglasses. An ophthalmologist or optometrist must keep documentation of the member’s inability to wear multi-focal eyeglasses.
Submitting the Montana Healthcare Programs Rx Form
- Place the order online with Classic Optical or fax or mail the order form to the eyeglass contractor. (See Key Contacts.) Phone orders are not accepted. To ensure orders will be processed accurately and on time, all sections of the order form must be completed.
- Errors in the fabrication of eyeglasses made by the eyeglass contractor will be corrected by the contractor at no additional charge.
- If the dispensing provider makes a mistake on a prescription, the eyeglass contractor will correct the error (but not cover the cost of the remaking of the eyeglasses). The dispensing provider will order the correct prescription and return the incorrect eyewear to Classic Optical. Classic Optical will charge the dispensing provider full price for the eyeglasses that were originally made. When the return eyewear arrives at Classic Optical, the dispensing provider will be reimbursed 50% of the cost of the first eyeglasses that were made incorrectly.
Other Programs
This is how the information in this chapter applies to Department programs other than Montana Healthcare Programs.
Healthy Montana Kids Program (HMK)/CHIP
Eyeglass services are covered by HMK/Montana Provider Relations, but optometric services are covered by Blue Cross and Blue Shield of Montana/CHIP. Most of the eyeglass services information in this chapter applies to HMK members. The exceptions are as follows:
- HMK members are eligible for eyeglasses every 365 days.
- HMK members do not receive retroactive eligibility.
- HMK members are not eligible for replacement lenses or frames that are not covered under manufacturer’s warranty or are lost or stolen.
- HMK members are 18 years of age or under.
- HMK members are not eligible for contact lenses or contacts lens exams.
Additional information regarding HMK is available on the HMK website at https://dphhs.mt.gov/HMK.
Mental Health Services Plan (MHSP)
Eye exams and eyeglasses are not covered under the Mental Health Services Plan (MHSP). See the mental health manual on the Provider Information website.
End of Covered Services Chapter
Prior Authorization
What Are Prior Authorization and the Team Care Program?
Although Passport to Health requirements do not apply to optometric, ophthalmologist and eyeglass services, prior authorization is required for some services, and the member may be part of the Team Care Program.
Team Care (ARM 37.86.5303)
Team Care is a restricted services program that is part of Passport to Health. Restricted services programs are designed to assist members in making better healthcare decisions so that they can avoid over utilizing health services. Team Care members are joined by a team assembled to assist them in accessing healthcare. The team consists of the member, the PCP, a pharmacy, and the Department. The team may also include a community-based care manager from the Department's Health Improvement Program.
Prior Authorization
Some services require prior authorization before providing them. If a service requires prior authorization, the requirement exists for all Montana Healthcare Programs members.
When seeking prior authorization, keep in mind the following:
- The referring provider should initiate all authorization requests.
- Always refer to the Montana Healthcare Programs fee schedule for prior authorization requirements on specific services.
- Eyeglasses have some services that are add-on features that require prior authorization. These features are not part of the contract of covered items with the eyeglass supplier and are listed as needing prior authorization on the Eyeglasses Fee Schedule, available on the Provider Information website.
- Have all required documentation that may be needed before submitting for prior authorization. For documentation requirements, see the Prior Authorization Criteria for Specific Services table.
Prior Authorization Criteria for Specific Services
Services: Dispensing and fitting of contact lenses
PA Contact:
DPHHS Optometric Program Officer
P.O. Box 202951
Helena, MT 59620
Phone: (406) 444-4066
Fax: (406) 444-1861
Documentation Required:
- Prior authorization is required for contact lenses and dispensing fees.
- Diagnosis must be one of the following:
- Keratoconus
- Aphakia
- Sight cannot be corrected to 20/40 with eyeglasses
- Anisometropia of 2 diopters or more
Services: Transition lenses, Tints other than Rose 1 and Rose 2 (including photochromic tints), UV and scratch resistant coating, Polycarbonate lenses, Round bifocals, and Deluxe frames.
PA Contact:
Optometric Program
Health Resources Division
P.O. Box 202951
Helena, MT 59620-2951
Fax: (406) 444-1861
Documentation Required:
- Requests for prior authorization must:
- Be submitted by fax or mailed to the Department.
- Include diagnosis and sufficient documentation from the optometrist or ophthalmologist that transition lenses, tints, UV and scratch resistant coating, or deluxe frames are medically necessary.
- For polycarbonate lenses, include documentation verifying member is monocular.
Services: Eye Prosthesis
PA Contact:
Mountain-Pacific Quality Health
3404 Cooney Drive
Helena, MT 59602
Phone: (877) 443-4021, Long-distance
(406) 457-3060 Local
Fax: (877) 443-2580 Long-distance
(406) 513-1923 Local
For HMK members, BCBSMT case managers review requests for durable medical equipment. If the cost is greater than $500, prior authorization is required.
Documentation Required:
- Documentation that supports medical necessity
- Documentation regarding the member’s ability to comply with any required after care
- Letters of justification from referring physician
- Documentation should be provided at least two weeks prior to the procedure date.
Other Programs
The prior authorization requirements apply to Healthy Montana Kids (HMK) eyeglass services. Optometric services are covered under the HMK plan of Blue Cross and Blue Shield of Montana (BCBSMT). Eye exams and eyeglasses are not covered under the Mental Health Services Plan (MHSP). Refer to the mental health services manual on the Provider Information website.
End of Prior Authorization Chapter
Coordination of Benefits
When Members Have Other Coverage
Montana Healthcare Programs members often have coverage through Medicare, workers’ compensation, employment-based coverage, individually purchased coverage, etc. Coordination of benefits is the process of determining which source of coverage is the primary payer in a particular situation. In general, providers must bill other carriers before billing Montana Healthcare Programs, but there are some exceptions. (See Exceptions to Billing Third Party First later in this chapter.) Medicare coverage is processed differently than other sources of coverage.
Identifying Other Sources of Coverage
The member’s Montana Healthcare Programs ID card may list other payers such as Medicare or other third party payers. (See Member Eligibility and Responsibilities in the General Information for Providers manual.) If a member has Medicare, the Medicare ID number is listed on the card. If a member has other coverage (excluding Medicare), it will be shown under the TPL section of the ID card. Some examples of third party payers include:
- Private health insurance
- Employment-related health insurance
- Workers’ compensation insurance*
- Health insurance from an absent parent
- Automobile insurance*
- Court judgments and settlements*
- Long-term care insurance
*These third party payers (and others) may not be listed on the member’s ID card.
Medicare claims are processed differently than other sources of coverage.
Providers must use the same procedures for locating third party sources for Montana Healthcare Programs members as for their non-Montana Healthcare Programs members. Providers cannot refuse service because of a third party payer or potential third party payer.
When a Member Has Medicare
Medicare claims are processed and paid differently than claims involving other payers. The other sources of coverage are referred to as third party liability (TPL), but Medicare is not.
Medicare Part A Claims
Medicare Part A covers inpatient hospital care, skilled nursing care and other services. Medicare Part A services are covered in more detail in specific program manuals where the providers bill for Part A services.
Medicare Part B Crossover Claims
Medicare Part B covers physician care, eye exams, and other services. The Department has an agreement with Medicare Part B carriers for Montana (Noridian) and the Durable Medical Equipment Regional Carrier (DMERC). Under this agreement, the carriers provide the Department with a magnetic tape of CMS-1500 claims for members who have both Medicare and Montana Healthcare Programs coverage. For claims to automatically cross over from Medicare to Montana Healthcare Programs, providers must:
- Accept Medicare assignment (otherwise payment and the Explanation of Medicare Benefits (EOMB) go directly to the member and will not cross over).
- Submit their Medicare and Montana Healthcare Programs provider numbers to Provider Relations.
In these situations, providers need not submit Medicare Part B crossover claims to Montana Healthcare Programs. Medicare will process the claim, submit it to Montana Healthcare Programs, and send the provider an EOMB. Providers must check the EOMB for the statement indicating that the claim has been referred to Montana Healthcare Programs for further processing. It is the provider’s responsibility to follow up on crossover claims and make sure they are correctly billed to Montana Healthcare Programs within the timely filing limit. (See Billing Procedures.)
When submitting electronic claims with paper attachments, see the Billing Electronically with Paper Attachments section of the Billing Procedures chapter in this manual.
When Medicare Pays or Denies a Service
- When Medicare pays an eye exam claim for a provider that is set up for automatic crossover, the claim should automatically cross over to Montana Healthcare Programs for processing, so the provider does not need to submit these claims to Montana Healthcare Programs. Providers that are not set up for automatic crossover should submit a claim to Montana Healthcare Programs after Medicare pays, and Montana Healthcare Programs will consider the claim for payment. If Medicare denies an eye exam claim, submit the claim to Montana Healthcare Programs. (See Submitting Medicare Claims to Montana Healthcare Programs later in this chapter.)
- Members who have Medicare/QMB or Medicare/Montana Healthcare Programs coverage must choose whether to access their Medicare or Montana Healthcare Programs benefits for eyeglasses. If a member chooses to use Medicare, do not bill Montana Healthcare Programs, and any claims that cross over from Medicare will be denied.
- For members who have QMB only coverage, the provider bills Medicare first for eyeglass claims, and if Medicare pays the claim, Montana Healthcare Programs will consider the claim for payment. If Medicare denies the claim, Montana Healthcare Programs will also deny the claim. For more information on QMB, see the General Information for Providers manual, Member Eligibility and Responsibilities chapter.
All Part B crossover claims submitted to Montana Healthcare Programs before Medicare’s 45-day response time will be returned to the provider.
When Montana Healthcare Programs Does Not Respond to Crossover Claims
When Montana Healthcare Programs does not respond within 45 days of the provider receiving the Medicare EOMB, submit a claim, with a copy of the Medicare EOMB, to Montana Healthcare Programs for processing.
Submitting Medicare Claims to Montana Healthcare Programs
When submitting a paper claim to Montana Healthcare Programs, attach the Medicare EOMB and use Montana Healthcare Programs billing instructions and codes. Medicare’s instructions, codes, and modifiers may not be the same as Montana Healthcare Programs’s. The claim must also include the provider’s NPI and Montana Healthcare Programs member ID number.
Remember to submit Medicare crossover claims to Montana Healthcare Programs only:
- When the referral to Montana Healthcare Programs statement is missing from the provider’s EOMB.
- When the provider does not hear from Montana Healthcare Programs within 45 days of receiving the Medicare EOMB.
When a Member Has TPL (ARM 37.85.407)
When a Montana Healthcare Programs member has additional medical coverage (other than Medicare), it is often referred to as third party liability (TPL). In most cases, providers must bill other insurance carriers before billing Montana Healthcare Programs.
Providers are required to notify their members that any funds the member receives from third party payers (when the services were billed to Montana Healthcare Programs) must be turned over to the Department. The following words printed on the member’s statement will fulfill this requirement: When services are covered by Montana Healthcare Programs and another source, any payment the member receives from the other source must be turned over to Montana Healthcare Programs.
It is the provider’s responsibility to follow up on TPL claims and make sure they are billed correctly to Montana Healthcare Programs within the 12-month timely filing period.
Exceptions to Billing Third Party First
In a few cases, providers may bill Montana Healthcare Programs first.
- When a Montana Healthcare Programs member is also covered by Indian Health Service (IHS) or the Montana Crime Victim Compensation Fund, providers must bill Montana Healthcare Programs before IHS or Crime Victims. These are not considered third party liability.
- If the third party has only potential liability, such as automobile insurance, the provider may bill Montana Healthcare Programs first. Do not indicate the potential third party on the claim. Instead, notify the Department of the potential third party by sending the claim and a note to Third Party Liability. (See the Contact Us page on the Provider Information website.)
Requesting an Exemption
- Providers may request to bill Montana Healthcare Programs first under certain circumstances. In each of these cases, the claim and required information must be sent directly to the Third Party Liability. See the Contact Us page on the Provider Information website.
- When a provider is unable to obtain a valid assignment of benefits, the provider must submit the claim with documentation that the provider attempted to obtain assignment and certification that the attempt was unsuccessful.
- When the Child Support Enforcement Division has required an absent parent to have insurance on a child, the claim can be submitted to Montana Healthcare Programs when the following requirements are met:
- The third party carrier has been billed, and 30 days or more have passed since the date of service.
- The claim is accompanied by a certification that the claim was billed to the third party carrier, and payment or denial has not been received.
- If another insurance has been billed, and 90 days have passed with no response, attach a note to the claim explaining that the insurance company has been billed or attach a copy of the letter sent to the insurance company Include the date the claim was submitted to the insurance company and certification that there has been no response.
- When the provider has billed the third party insurance and has received a non-specific denial (e.g., no member name, date of service, amount billed), submit the claim with a copy of the denial and a letter of explanation directly to Third Party Liability to avoid missing the timely filing deadline.
When the Third Party Pays or Denies a Service
When a third party payer is involved (excluding Medicare) and the other payer:
- Pays the claim. Indicate the amount paid in the Amount Paid field of the claim when submitting to Montana Healthcare Programs for processing. These claims may be submitted either electronically or on paper.
- Allows the claim, and the allowed amount went toward the member’s deductible. Include the insurance Explanation of Benefits (EOB) when billing Montana Healthcare Programs. These claims must be submitted on paper.
- Denies the claim. Include a copy of the denial (including the reason and the reason explanation) with the claim, and submit to Montana Healthcare Programs.
- Denies a line on the claim. Bill the denied lines together on a separate claim and submit to Montana Healthcare Programs. Include the explanation of benefits (EOB) from the other payer as well as an explanation of the reason for denial (e.g., definition of denial codes).
If the provider receives a payment from a third party after the Department has paid the provider, the provider must return the lower of the two payments to the Department within 60 days.
When the Third Party Does Not Respond
If another insurance has been billed, and 90 days have passed with no response, bill Montana Healthcare Programs as follows:
- Attach a note to the claim explaining that the insurance company has been billed, or attach a copy of the letter sent to the insurance company.
- Include the date the claim was submitted to the insurance company.
- Send this information to Third Party Liability. See the Contact Us page on the Provider Information website.
Other Programs
The information in this chapter does not apply to Healthy Montana Kids (HMK) or the Mental Health Services Plan (MHSP). The MHSP manual is available on the Provider Information website.
End of Coordination of Benefits Chapter
Billing Procedures
Claim Forms
Services provided by optometrists, opticians, and ophthalmologists must be billed either electronically on a Professional claim or on a CMS-1500 paper claim form. CMS-1500 forms are available from various publishing companies; they are not available from the Department or Provider Relations.
Timely Filing Limits (ARM 37.85.406)
Providers must submit clean claims to Montana Healthcare Programs within:
- Twelve months from whichever is later:
- The date of service
- The date retroactive eligibility or disability is determined
- Medicare Crossover Claims: Six months from the date on the Medicare explanation of benefits approving the service (if the Medicare claim was timely filed and the member was eligible for Medicare at the time the Medicare claim was filed).
- Claims involving other third party payers (excluding Medicare): Six months from the date on an adjustment notice from a third party payer who has previously processed the claim for the same service, and the adjustment notice is dated after the periods described above.
Clean claims are claims that can be processed without additional information or action from the provider. The submission date is defined as the date that the claim was received by the Department or the claims processing contractor. All problems with claims must be resolved within this 12-month period.
Tips to Avoid Timely Filing Denials
- Correct and resubmit denied claims promptly. (See the Remittance Advices and Adjustments chapter in this manual.)
- If a claim submitted to Montana Healthcare Programs does not appear on the remittance advice within 30 days, contact Provider Relations for claim status.
- If another insurer has been billed and 90 days have passed with no response, a provider can bill Montana Healthcare Programs. (See the Coordination of Benefits chapter in this manual for more information.)
- To meet timely filing requirements for Medicare/Montana Healthcare Programs crossover claims, see the Coordination of Benefits chapter in this manual.
When to Bill Montana Healthcare Programs Members (ARM 37.85.406)
In most circumstances, providers may not bill Montana Healthcare Programs members for services covered under Montana Healthcare Programs.
More specifically, providers cannot bill members directly:
- For the difference between charges and the amount Montana Healthcare Programs paid.
- For a covered service provided to a Montana Healthcare Programs-enrolled member who was accepted as a Montana Healthcare Programs member by the provider, even if the claim was denied.
- When a third party payer does not respond.
- When a member fails to arrive for a scheduled appointment. Montana Healthcare Programs may not be billed for no-show appointments either.
- When services are free to the member, such as in a public health clinic. Montana Healthcare Programs may not be billed for those services either.
Under certain circumstances, providers may need a signed agreement in order to bill a Montana Healthcare Programs member (see the following table).
If a provider bills Montana Healthcare Programs and the claim is denied because the member is not eligible, the provider may bill the member directly.

Routine Agreement: This may be a routine agreement between the provider and member which states that the member is not accepted as a Montana Healthcare Programs member, and that he/she must pay for the services received.
Custom Agreement: This agreement lists the service the member is receiving and states that the service is not covered by Montana Healthcare Programs and the member will pay for it.
Usual and Customary Charge (ARM 37.85.406)
Providers should bill Montana Healthcare Programs their usual and customary charge for each service; that is, the same charge that is made to other payers for that service.
Billing Members with Other Insurance
If a Montana Healthcare Programs member is also covered by Medicare, has other insurance, or some other third party is responsible for the cost of the members healthcare, see the Coordination of Benefits chapter in this manual.
Billing for Retroactively Eligible Members
When the provider accepts the member's retroactive eligibility, the provider has 12 months from the date retroactive eligibility was determined to bill for those services. When submitting claims for retroactively eligible members in which the date of service is more than 12 months earlier than the date the claim is submitted, attach a copy of the Notice of Retroactive Eligibility (Form 160-M). To obtain Form 160-M, the provider needs to contact the member's local Office of Public Assistance and request the form. For a list of local Offices of Public Assistance, see https://dphhs.mt.gov/hcsd/OfficeofPublicAssistance.
For more information on retroactive eligibility, see the Member Eligibility and Responsibilities chapter in the General Information for Providers manual.
Place of Service
Place of service must be entered correctly on each line. Montana Healthcare Programs typically reduces payment for services provided in hospitals and ambulatory surgical centers since these facilities typically bill Montana Healthcare Programs separately for facility charges. For a list of place of service codes, see the CMS website: http://cms.hhs.gov/Medicare/Coding/place-of-service-codes/index.html.
Multiple Visits on Same Date
Montana Healthcare Programs generally covers only one dispensing fee per member per day, unless two pairs of single vision eyeglasses are dispensed (distance/near).
When a member requires additional visits on the same day, use a modifier to describe the reason for multiple visits. When a modifier is not appropriate for the situation, attach documentation of medical necessity to the claim, and submit it to the Optometric program officer.
Coding Tips
Standard use of medical coding conventions is required when billing Montana Healthcare Programs. Provider Relations or the Department cannot suggest specific codes to be used in billing for services. For coding assistance and resources, see the table of Coding Resources on the following page. The following suggestions may help reduce coding errors and unnecessary claim denials:
- Use current CPT, HCPCS, and ICD diagnosis coding books.
- Always read the complete description and guidelines in the coding books. Relying on short descriptions can result in inappropriate billing.
- Attend classes on coding offered by certified coding specialists.
- Follow CPT guidelines on the difference between a new member and an established member.
- Bill for the appropriate level of service provided.
- Services covered within global periods for certain CPT procedures are not paid separately and must not be billed separately. Most surgical and some medical procedures include routine care before and after the procedure. Montana Healthcare Programs fee schedules show the global period for each CPT service.
- Use the correct number of units on CMS-1500 claims. In general, Montana Healthcare Programs follows the definitions in CPT and HCPCS coding manuals. Unless otherwise specified, one unit equals one visit or one procedure. For specific codes, however, one unit may be 15 minutes. Always check the long text of the code description.
- CPT codes that are billed based on the amount of time spent with the member must be billed with the code that is closest to the time spent.
Coding Resources
Please note that the Department does not endorse the products of any particular publisher.
CPT
Description:
CPT codes and definitions.
Updated each January.
Contact:
American Medical Association - https://commerce.ama-assn.org/store/
(800) 621-8335
CPT Assistant
Description:
A newsletter on CPT coding issues.
Contacts:
American Medical Association - https://commerce.ama-assn.org/store/
(800) 621-8335
HCPCS Level II
Description:
HCPCS codes and definitions.
Updated each January and throughout the year.
Contact:
Available through various publishers and bookstores or from CMS at www.cms.gov.
ICD
Description:
ICD diagnosis and procedure code definitions.
Updated each October .
Contact:
Available through various publishers and bookstores.
Miscellaneous Resources
Various newsletters and other coding resources are available in the commercial marketplace.
UB-04 National Uniform Billing Expert
Description:
National UB-04 billing instructions
Contact:
Available through various publishers and editors
Using the Montana Healthcare Programs Fee Schedule
When billing Montana Healthcare Programs, it is important to use the Department’s fee schedule for your provider type in conjunction with the detailed coding descriptions listed in CPT and HCPCS coding books. In addition to covered services and payment rates, fee schedules often contain helpful information such as global periods, if multiple surgery guidelines apply, if the procedure can be done bilaterally, if an assistant, co-surgeon, or team is allowed for the procedure, if the code is separately billable, if prior authorization is required, and more. Department fee schedules are updated each January and July; some also in April and October. Be aware of fee schedule publish dates. Fee schedules are available on the Provider Information website.
Using Modifiers
- Review the guidelines for using modifiers in the current CPT, HCPCS, or other helpful resources.
- Always read the complete description for each modifier; some modifiers are described in the CPT manual while others are in the HCPCS coding book.
- The Montana Healthcare Programs claims processing system recognizes three pricing modifiers and one informational modifier per claim line. Providers are asked to place any modifiers that affect pricing in the first two modifier fields.
- When billing with Modifier 50 for bilateral services, put all information on one line with one unit. You do not need to use modifiers for left and right, and do not bill on separate lines.
- Check the fee schedule to see if Montana Healthcare Programs allows the use of the following modifiers for a particular code: bilateral (50), multiple procedures (51), co-surgery (62), assistant at surgery (80, 81, 82, AS).
Billing Tips for Specific Services
Bundled Services
Certain services with CPT or HCPCS codes (e.g., tear duct plugs) are covered by Montana Healthcare Programs but have a fee of zero. This means that the service is typically “bundled” with an office visit or other service. Since the bundled service is covered by Montana Healthcare Programs, providers may not bill the member separately for it.
Contact Lenses
When billing Montana Healthcare Programs for contact lenses, include the prior authorization number on the claim.
Eye Exams
- A member may be eligible for an eye exam before the specified time limit expires if he/she meets the criteria described in the Covered Services chapter, Eye Exams section, of this manual. In this case, enter the reason for the exam on the claim.
- Medicare does not cover eye refraction but instructs providers to report this service as a separate line item from the other services performed. Montana Healthcare Programs covers this procedure, so providers can bill for the eye exam and the refraction.
- Children (age 20 or under for Montana Healthcare Programs or age 18 or under for HMK) may receive an additional exam before the 365-day limit has passed if they have had at least a one line acuity change resulting in prescribing replacement lenses that meet the criteria in the Eyeglass Services section of the Covered Services chapter in this manual. In this case, providers may bill Montana Healthcare Programs for the exam using EPSDT indicator 1 on the claim. See the Submitting a Claim chapter in this manual.
Eyeglass Services
- Adult members (ages 21 or older) may receive new lenses before the 730-day limit has passed if they meet the criteria described the Eyeglass Services and the Services for Children section of the Covered Services chapter in this manual. In this case, providers may bill Montana Healthcare Programs for a dispensing fee for new lenses using the appropriate modifiers with the dispensing fee procedure code. Adult members may be eligible for replacement lenses 12 months after the initial dispensing of contract eyeglasses if the lenses are broken or unusable.
- Children (age 20 or under for Montana Healthcare Programs or age 18 or under for HMK) may receive new lenses before the 365-day limit has passed if they meet the criteria in the Eyeglass Services section of the Covered Services chapter in this manual. In this case, providers may bill Montana Healthcare Programs for a dispensing fee for new lenses using EPSDT indicator 1 on the claim.
- If the adult Montana Healthcare Programs member (age 21 or over) is not eligible for lenses and/or frame within the 730-day period, the dispensing provider may not bill Montana Healthcare Programs for a dispensing fee. If the member chooses to purchase eyeglasses privately, the provider may bill the Montana Healthcare Programs member for dispensing services and eyeglass materials.
- The eyeglass contractor will bill Montana Healthcare Programs for the laboratory and material costs for lenses and frames.
- Bill HMK for eyeglass services and optometric services.
Frame Services
- When the Montana Healthcare Programs member uses an existing frame, the dispensing provider bills Montana Healthcare Programs for dispensing services, lenses only.
- Providers may not charge a dispensing fee for minor frame repairs that they provide themselves.
- If a member who is covered by Medicare and Montana Healthcare Programs chooses a frame outside the Montana Healthcare Programs contract, the provider cannot bill Montana Healthcare Programs for the dispensing fee. All charges must be billed to Medicare and the member.
Lens Add-Ons
The eyeglass contractor bills the dispensing provider their usual and customary charge for any lens style, lens material, tint, coating, lens enhancement (e.g., polished edge) not covered by Montana Healthcare Programs. It is the dispensing provider’s responsibility to bill the Montana Healthcare Programs member for these items. Do not bill Montana Healthcare Programs.
For example, FT7x35 Trifocal is billed to the dispensing provider at the contractor’s usual and customary price, not at a price which would reflect the difference between the contract price for 7x28, and the usual and customary 7x35 price. For FT 28 CR-39 with polished edges, only the polished edge price is billed to the dispensing provider at the contractor’s usual and customary charge.
Replacement Lenses and Frames
If a member has selected to use an existing frame, and the existing frame breaks after lenses were dispensed to the member, Montana Healthcare Programs will not cover new lenses. The Montana Healthcare Programs member may privately pay for new lenses or select a contract frame into which the existing lenses will fit. If a contract frame is selected, the dispensing provider may bill Montana Healthcare Programs for dispensing services, frame only.
Submitting Electronic Claims
Institutional claims submitted electronically are referred to as ANSI ASC X12N 837 transactions. Providers who submit claims electronically experience fewer errors and quicker payment. Providers should be familiar with federal rules and regulations regarding electronic transactions. Claims may be submitted electronically by the following methods:
- WINASAP 5010. Montana Provider Relations makes this free software available to providers who may use it to submit claims for Montana Healthcare Programs, MHSP, HMK (dental and eyeglasses only) and FQHC/RHC. It does not support submissions to Medicare or other payers. This software creates an 837 transaction, but does not accept an 835 transaction back from the Department.)
- Montana Access to Health (MATH) Web Portal. A secure website on which providers may view members’ medical history, verify member eligibility, submit electronic claims to Montana Healthcare Programs via a HIPAA-compliant X12 837 file, check the status of a claim, verify the status of a warrant, and download remittance advice reports.
- EDI Clearinghouse. Providers can send claims to the EDI clearinghouse (EDI Solutions) in X12 837 format. Electronic submitters are required to certify their 837 transactions as HIPAA-compliant before sending their transactions through the EDI clearinghouse. EDIFECS certifies the 837 HIPAA transactions at no cost to the provider. EDIFECS certification is completed through EDI Solutions.
- Clearinghouses. Providers can contract with a clearinghouse and send claims in whatever format the clearinghouse accepts. The provider’s clearinghouse then sends the claim to the EDI clearinghouse in the X12 837 format. The provider’s clearinghouse also needs to have their 837 transactions certified through EDIFECS before submitting claims to the EDI clearinghouse. EDIFECS certification is completed through EDI Solutions. For more information on electronic claims submission, contact the EDI Support Unit.
- MOVEit DMZ. Providers use this secure transmission protocol and secure storage landing zone (intermediate storage) for the exchange of files between trading partners and EDI. It is intended for trading partners/submitters who submit in excess of 20 files per day or whose physical file sizes regularly exceed 2 MB.
- B2B Gateway SFTP/FTPS Site. Providers use this method to send electronic transactions through the secure FTP process. This is typically encountered with high-volume/high-frequency submitters.
Billing Electronically with Paper Attachments
When submitting claims that require additional supporting documentation, the Attachment Control Number field must be populated with an identifier. Identifier formats can be designed by software vendors or clearinghouses, but the preferred method is the provider’s NPI followed by the member’s ID number and the date of service, each separated by a dash:

The supporting documentation must be submitted with a Paperwork Attachment Cover Sheet. (See the Forms page of the Provider Information website.) The number in the paper Attachment Control Number field must match the number on the cover sheet.
Submitting Paper Claims
For instructions on completing a paper claim, see the Submitting a Claim chapter in this manual. Unless otherwise stated, all paper claims must be mailed to:
Claims Processing
P.O. Box 8000
Helena, MT 59604
Claim Inquiries
If you have questions on a specific claim, contact Provider Relations. See the Contact Us page on the Provider Information website.
The Most Common Billing Errors and How to Avoid Them
Paper claims are often returned to the provider before they can be processed, and many other claims (both paper and electronic) are denied.
To avoid unnecessary returns and denials, double-check each claim to confirm the following items are included and accurate.
Common Billing Errors
Reasons for Return or Denial: Provider NPI missing or invalid
How to Prevent Returned or Denied Claims: The provider NPI is a 10-digit number assigned to the provider by the National Plan and Provider Enumeration System. Verify the correct provider NPI is on the claim.
Reasons for Return or Denial: Authorized signature missing
How to Prevent Returned or Denied Claims: Each claim must have an authorized signature belonging to the provider, billing clerk, or office personnel. The signature may be typed, stamped, or hand-written.
Reasons for Return or Denial: Signature date missing
How to Prevent Returned or Denied Claims: Each claim must have a signature date.
Reasons for Return or Denial: Incorrect claim form used
How to Prevent Returned or Denied Claims: The claim must be the correct form for the provider type. Services covered in this manual require a CMS-1500 claim form (or electronic Professional claim).
Reasons for Return or Denial: Information on claim form not legible
How to Prevent Returned or Denied Claims: Information on the claim form must be legible. Use dark ink and center the information in the field. Information must not be obscured by lines.
Reasons for Return or Denial: Member number not on file, or member was not eligible on date of service
How to Prevent Returned or Denied Claims: Before providing services to the member:
- View the member’s ID card at each visit. Montana Healthcare Programs eligibility may change monthly.
- Verify member eligibility by using one of the methods described in the Member Eligibility and Responsibilities chapter of the General Information for Providers manual.
Reasons for Return or Denial: Duplicate claim
How to Prevent Returned or Denied Claims:
- Check all remittance advices for previously submitted claims before resubmitting.
- When making changes to previously paid claims, submit an adjustment form rather than a new claim. (See Remittance Advices and Adjustments in this manual.)
- Allow 45 days for the Medicare/Montana Healthcare Programs Part B crossover claim to appear on the remittance advice before submitting the claim directly to Montana Healthcare Programs.
Reasons for Return or Denial: Medicare Part B crossover claims submitted before Medicare’s 45-day crossover limit
How to Prevent Returned or Denied Claims: Claims that cross over between Medicare Part B and Montana Healthcare Programs should not be billed on paper to Montana Healthcare Programs until 45 days after the Medicare Part B paid date. These claims will be returned to the provider.
Reasons for Return or Denial: Prior authorization number is missing
How to Prevent Returned or Denied Claims:
- Prior authorization is required for certain services, and the prior authorization number must be on the claim. (See the Prior Authorization chapter in this manual.)
- Mental Health Services Plan (MHSP) claims must be billed and services performed during the prior authorization span. The claim will be denied if it is not billed according to the spans on the authorization. See mental health services manual.
Reasons for Return or Denial: TPL on file and no credit amount on claim
How to Prevent Returned or Denied Claims:
- If the member has any other insurance (or Medicare), bill the other carrier before Montana Healthcare Programs. See Coordination of Benefits in this manual.
- If the member’s TPL coverage has changed, providers must notify TPL before submitting a claim. See the Contact Us page on the Provider Information website.
Reasons for Return or Denial: Claim past 365-day filing limit
How to Prevent Returned or Denied Claims:
- Claims Processing must receive all clean claims and adjustments within the timely filing limits described in this chapter.
- To ensure timely processing, claims and adjustments must be mailed to Claims Processing. See the Contact Us page on the Provider Information website.
Reasons for Return or Denial: Missing Medicare EOMB
How to Prevent Returned or Denied Claims: All Medicare crossover claims on CMS-1500 forms must have an Explanation of Medicare Benefits (EOMB) attached, and be billed to Montana Healthcare Programs on paper.
Reasons for Return or Denial: Provider is not eligible during dates of services, or provider NPI terminated
How to Prevent Returned or Denied Claims:
- Out-of-state providers must update enrollment early to avoid denials. If enrollment has lapsed, claims submitted with a date of service after the expiration date will be denied until the provider updates his/her enrollment.
- New providers cannot bill for services provided before Montana Healthcare Programs enrollment begins.
- If a provider is terminated from the Montana Healthcare Programs, claims submitted with a date of service after the termination date will be denied.
Reasons for Return or Denial: Type of service/procedure is not allowed for provider type
How to Prevent Returned or Denied Claims:
- Provider is not allowed to perform the service, or type of service is invalid.
- Verify the procedure code is correct using applicable CPT and HCPCS coding books.
- Check the Montana Healthcare Programs fee schedule to verify the procedure code is valid for your provider type.
Other Programs
Billing procedures for eyeglass services apply to Healthy Montana Kids (HMK); however, billing procedures for eye exams do not apply to HMK because optometric services are covered by Blue Cross and Blue Shield of Montana. These billing procedures do not apply to the Mental Health Services Plan (MHSP); that manual is available on the Provider Information website.
End of Billing Procedures Chapter
Submitting a Claim
The services described in this manual are billed either electronically on a Professional claim or on a paper CMS-1500 claim form. Claims submitted with all of the necessary information are referred to as clean and are usually paid in a timely manner. (See the Billing Procedures chapter in this manual.)
Claims are completed differently for the different types of coverage a member has. The following are accepted codes:
EPSDT/Family Planning Indicators
Code: 1 Member/Service: EPSDT
Purpose: Used when the member is under age 21.
Code: 2 Member/ Service: Family Planning
Purpose: Used when providing family planning services.
Code: 3 Member/ Service: EPSDT and Family Planning
Purpose: Used when the member is under age 21 and is receiving family planning services.
Code: 4 Member/ Service: Pregnancy (any service provided to a pregnant woman)
Purpose: Used when providing services to pregnant women.
Code: 6 Member/ Service: Nursing facility member
Purpose: Used when providing services to nursing facility residents.
Unless otherwise stated, all paper claims must be mailed to the following address:
Claims Processing
P.O. Box 8000
Helena, MT 59604
Avoiding Claim Errors
Claims are often denied or even returned to the provider before they can be processed. To avoid denials and returns, double-check each claim to confirm the items below are accurate. For more information on returned and denied claims, see the Billing Procedures chapter in this manual.
Common Claim Errors
Claim Error: Required field is blank
Prevention: Check the claim instructions earlier in this chapter for required fields (indicated by * or **). If a required field is blank, the claim may either be returned or denied.
Claim Error: member ID number missing or invalid
Prevention: This is a required field (Field 10d); verify that the member’s Montana Healthcare Programs ID number is listed as it appears on the member’s eligibility information.
Claim Error: member name missing
Prevention: This is a required field (Field 2); check that it is correct.
Claim Error: NPI/API missing or invalid
Prevention: The NPI is a 10-digit number (API is a 7-digit) assigned to the provider. Verify the correct NPI/API is on the claim.
Claim Error: Referring or Passport provider name and ID number missing
Prevention: When a provider refers a member to another provider, include the referring provider’s name and ID number or Passport number (see the Passport chapter in this manual).
Claim Error: Prior authorization number missing
Prevention: When prior authorization (PA) is required for a service, the PA number must be on the claim (see the Prior Authorization chapter in this manual).
Claim Error: Not enough information regarding other coverage
Prevention: Fields 1a and 11d are required fields when a member has other coverage (see examples earlier in this chapter).
Claim Error: Authorized signature missing
Prevention: Each claim must have an authorized signature belonging to the provider, billing clerk, or office personnel. The signature may be typed, stamped, or handwritten.
Claim Error: Signature date missing
Prevention: Each claim must have a signature date.
Claim Error: Incorrect claim form used
Prevention: Services covered in this manual require a CMS-1500 claim form.
Claim Error: Information on claim form not legible
Prevention: Information on the claim form must be legible. Use dark ink and center the information in the field. Information must not be obscured by lines.
Claim Error: Medicare EOMB not attached
Prevention: When Medicare is involved in payment on a claim, the Medicare EOMB must be submitted with the claim or it will be denied.
Other Programs
This chapter applies to claims completed for HMK eyeglass services. This chapter does not apply to HMK optometric services because they are covered by Blue Cross and Blue Shield of Montana.
End of Submitting a Claim Chapter
Remittance Advices and Adjustments
The Remittance Advice
The remittance advice is the best tool providers have to determine the status of a claim. Remittance advices accompany payment for services rendered and provide details of all transactions that have occurred during the previous remittance advice cycle.
Each line of the remittance advice represents all or part of a claim and explains whether the claim or service has been paid, denied, or suspended (also referred to as pending). If the claim was suspended or denied, the remittance advice shows the reason.
Providers may receive the remittance advice electronically as an ANSI ASC X12 835 transaction, or once registered with the Montana Access to Health (MATH) web portal, they may receive remittance advices through the web portal.
To register for the MATH web portal and receive electronic remittance advices (ERAs), providers must complete the Trading Partner Agreement available on the Provider Enrollment page of the Provider Information website.
After this form has been processed, you will receive a password. Entry into the system requires a valid provider or group number and password. Each provider or group number requires a unique password, so providers must complete a separate request form for each provider or group.
Remittance advices are available from the MATH web portal in PDF format.
Electronic remittance advices (ERAs) are available on the MATH web portal for 90 days.
Due to space limitations, ERAs are available for 90 days.
Credit Balance Claims
Credit balance claims are shown until the credit has been satisfied.
Credit balances occur when claim adjustments reduce original payments causing the provider to owe money to the Department. These claims are considered in process and continue to appear on the remittance advice until the credit has been satisfied.
Credit balances can be resolved in two ways:
- By working off” the credit balance. Remaining credit balances can be deducted from future claims. These claims continue to appear on consecutive remittance advices until the credit has been paid.
- By sending a check payable to DPHHS for the amount owed. This method is required for providers who no longer submit claims to Montana Healthcare Programs. Include your NPI and indicate that the check is to pay off a credit balance. Send to the Third Party Liability unit. See the Contact Us page on the Provider Information website.
Rebilling and Adjustments
Rebillings and adjustments are important steps in correcting any billing problems you may experience. Knowing when to use the rebilling process versus the adjustment process is important.
Timeframe for Rebilling or Adjusting a Claim
- Providers may resubmit or adjust any initial claim within the timely filing limits described in the Billing Procedures chapter of this manual.
- These time periods do not apply to overpayments that the provider must refund to the Department. After the 12-month time period, a provider may not refund overpayments to the Department by completing a claim adjustment. The provider may refund overpayments by issuing a check or requesting a gross adjustment be made.
Rebilling Montana Healthcare Programs
Rebilling occurs when a provider submits a claim/claim line to Montana Healthcare Programs that was previously submitted for payment but was returned/denied. Claims are often returned to the provider before processing because information (e.g., provider NPI, authorized signature, date) is missing or unreadable. (See the Billing Procedures and Submitting a Claim chapters.)
When to Rebill Montana Healthcare Programs
- Claim Denied. Providers can rebill Montana Healthcare Programs when a claim is denied in full, as long as the claim was denied for reasons that can be corrected. When the entire claim is denied, check the Explanation of Benefits (EOB) code, make the appropriate corrections, and resubmit the corrected claim on a CMS-1500 form (not the Individual Adjustment form).
- Line Denied. When an individual line is denied on a multiple-line claim, correct any errors and rebill Montana Healthcare Programs. Either submit the denied service on a new CMS-1500 form, or cross out paid lines and resubmit the form. Do not use an Individual Adjustment form.
- Claim Returned. Rebill Montana Healthcare Programs when the claim is returned under separate cover. Occasionally, Montana Healthcare Programs is unable to process the claim and returns it to the provider with a letter indicating additional information is needed to process the claim. Correct the claim as directed and resubmit it.
How to Rebill
- Check any EOB code listed and make your corrections on a copy of the claim, or produce a new claim with the correct information.
- When making corrections on a copy of the claim, remember to cross out or omit all lines that have already been paid. The claim must be neat and legible for processing.
- Enter any insurance (third party liability) information on the corrected claim, or attach insurance denial information to the corrected claim, and send it to the Claims unit. See the Contact Us page of the Provider Information website.
Adjustments
If a provider believes that a claim has been paid incorrectly, the provider may call Provider Relations. Once an incorrect payment has been verified, the provider should submit an Individual Adjustment Request form to Provider Relations. If incorrect payment was the result of a Claims keying error, contact Provider Relations.
When adjustments are made to previously paid claims, the Department recovers the original payment and issues appropriate repayment. The result of the adjustment appears on the provider’s remittance advice as two transactions. The original payment will appear as a credit transaction. The replacement claim reflecting the corrections will be listed as a separate transaction and may or may not appear on the same remittance advice as the credit transaction. The replacement transaction will have nearly the same ICN number as the credit transaction, except the 12th digit will be a 2, indicating an adjustment. Adjustments are processed in the same time frame as claims.
When to Request an Adjustment
- Request an adjustment when a claim was overpaid or underpaid.
- Request an adjustment when a claim was paid but the information (e.g., member ID, provider NPI, date of service, procedure code, diagnoses, units) on the claim was incorrect.
How to Request an Adjustment
To request an adjustment, use Individual Adjustment Request form on the Forms page of the Provider Information website. The requirements for adjusting a claim are as follows:
- Claims Processing must receive individual claim adjustment requests within 12 months from the date of service. (See Timely Filing Limits in the Billing Procedures chapter.) After this time, gross adjustments are required.
- Use a separate adjustment request form for each ICN.
- If you are correcting more than one error per ICN, use only one adjustment request form, and include each error on the form.
Payment and the Remittance Advice
Providers receive their Montana Healthcare Programs payment and remittance advices electronically. Payment is via electronic funds transfer (EFT). Direct deposit is another name for EFT. Remittance advices are available through the MATH web portal for 90 days.
With EFT, the Department deposits the funds directly to the provider’s bank account. If the scheduled deposit day is a holiday, payments and ERAs will be available on the next business day.
To participate in EFT and receive ERAs, providers must complete the Montana Healthcare Programs Electronic Funds Transfer (EFT) and Electronic Remittance Advice (ERA) Authorization Agreement. In addition, a letter from the provider’s financial institution is required, and Passport providers have additional requirements. Contact Provider Relations for assistance.
Once electronic transfer testing shows payment to the provider’s account, Montana Healthcare Programs payments will be made through EFT. Contact Montana Provider Relations if you have questions.
Required Forms for EFT and ERA
Form: Montana Healthcare Programs Electronic Funds Transfer (EFT) & Electronic Remittance Advice (ERA) Authorization Agreement
Purpose: Allows the Department to automatically deposit Montana Healthcare Programs payment into provider’s bank account.
Where to Get: Provider Information website.
Form: Trading Partner Agreement
Purpose: Allows provider to access their ERA on the Montana Access to Health web portal (must also include the form above).
Where to Get: Provider Information website.
Form: Letter from the provider’s financial institution verifying the account number and routing number. Do not send voided checks or deposit slips.
Purpose: Paperwork requirement.
Where to Get: Your financial institution.
All forms should be faxed to Provider Relations (406) 442-4402.
Other Programs
The information in this chapter applies to the Healthy Montana Kids Program (HMK) eyeglasses only. Optometric services are covered under the HMK plan of Blue Cross and Blue Shield of Montana.
End of Remittance Advices and Adjustments Chapter
How Payment Is Calculated
Overview
Though providers do not need the information in this chapter in order to submit claims to the Department, the information allows providers to understand how payment is calculated and to predict approximate payment for particular claims.
The RBRVS Fee Schedule
Most services provided by optometrists, opticians, and ophthalmologists are paid for using the Department’s Resource-Based Relative Value Scale (RBRVS) fee schedule, which includes approximately 10,230 CPT codes, approximately 2,670 HCPCS codes.
RBRVS was developed for the Medicare program and implemented in 1992. Medicare does a major update annually, with smaller updates performed quarterly. Montana Healthcare Programs implemented its RBRVS-based fee schedule in August 1997. It is based largely on the Medicare model, with a few differences that are described below. By adapting the Medicare model to the needs of the Montana Healthcare Programs program, the Department was able to take advantage of the millions of dollars of research performed by the federal government and national associations of physicians and other healthcare professionals. RBRVS-based payment methods are widely used across the U.S. by Montana Healthcare Programs programs, Blue Cross and Blue Shield plans, workers’ compensation plans and commercial insurers.
Many Montana Healthcare Programs payment methods are based on Medicare, but there are differences, in these cases, the Montana Healthcare Programs method prevails.
The following paragraphs elaborate on aspects of the RBRVS fee schedule used by the Department.
Fee Calculation
Each fee is the product of a relative value times a conversion factor.
When Montana Healthcare Programs payment differs from the fee schedule, consider the following:
- The Department pays the lower of the established Montana Healthcare Programs fee or the provider’s charge
- Modifiers. See Other Modifiers in this chapter.
- Provider type. See Professional Differentials in this chapter.
- Place of service. See Site of Service Differential in this chapter.
- Date of service (fees for services may change over time).
- Also check for cost sharing and Medicare or TPL payments which will be shown on the remittance advice.
Basis of Relative Values
For almost all services, Montana Healthcare Programs uses the same relative values as Medicare does in Montana. (Nationally, Medicare adjusts the relative values for differences in practice costs between localities, but Montana is considered a single locality.) For fewer than 1% of codes, relative values are not available from Medicare. For these codes, the Department has set the relative values.
Composition of Relative Values
For each code, the relative value is the sum of a relative value for the work effort (including time, stress, and difficulty), the associated practice expense, and the associated malpractice expense.
Site of Service Differential
The Medicare program has calculated two sets of relative values for each code: one that reflects the practitioner’s practice cost of performing the service in an office and one that reflects the practitioner’s practice cost of performing the service in a hospital or ambulatory surgical center (ASC). When services are provided within a hospital or ASC (i.e., places of service 21, 22, 23, and 24), Montana Healthcare Programs typically pays a lower fee than if the service is provided in the office or another setting. The reason is that Montana Healthcare Programs typically also pays the hospital or ASC for the service.
Conversion Factor
The Department sets the conversion factor for the state fiscal year (July through June). The conversion factor is typically reviewed (and often changed) in July of each year.
Transition Adjustor
Because the move to an RBRVS-based fee schedule resulted in large changes in fees for some services, the Montana legislature directed the Department to pay transitional fees for about 2,250 of the 9,300 services covered by the fee schedule. For about 900 services, the transitional fee is lower than it otherwise would be; for 1,350 services, it is higher than it otherwise would be. The transitional fees are put in place by a transition adjustor.
Global Periods
For many surgical services, the fee covers both the service and all related care within a specified global period. For almost all such codes, the global periods used by Montana Healthcare Programs are identical to those used by Medicare, but in cases of differences the Montana Healthcare Programs policy applies. See the Billing Procedures chapter in this manual for more information on global periods.
Professional and Technical Components
Some services are divided into the technical component (performing the test) and the professional component (interpreting the test). A practitioner who only performs the test would bill the service with modifier TC; a practitioner who only interprets the test would bill with Modifier 26; and a practitioner who performs both components (referred to as a global service) would bill the code without a modifier. The fee schedule has separate fees for each component and for the global service.
Other Modifiers
Under the RBRVS fee schedule, certain other modifiers also affect payment.
How Modifiers Change Pricing
- Modifiers may not be applicable for all services. For services paid via the RBRVS fee schedule, the fee schedule shows the list of services for which Modifiers 26, TC, 50, 51, 62, and 80 apply.
- If a modifier does not appear in this list, then it does not affect pricing for Optometric and Eyeglass Services.
- The list shows summary modifier descriptions. See the CPT and HCPCS coding books for the full text.
Modifier: 22 Definition: Increased procedural service
How Payment Is Affected: The service is paid at 110% of fee.
Modifier: 26 Definition: Professional component
How Payment Is Affected: For services paid via the RBRVS fee schedule, see the specific service. For other services, payment equals 40% of the fee.
Modifier: 50 Definition: Bilateral procedure
How Payment Is Affected: The procedure is paid at 150% of the fee.
Modifier: 51 Definition: Multiple procedures
How Payment Is Affected: Each procedure is paid at 50% of the fee.
Modifier: 52 Definition: Reduced service
How Payment Is Affected: The service is paid at 50% of the fee.
Modifier: 53 Definition: Discontinued procedure
How Payment Is Affected: The service is paid at 50% of the fee.
Modifier: 54 Definition: Surgical care only
How Payment Is Affected: The service is paid at 75% of the fee.
Modifier: 55 Definition: Postoperative management only
How Payment Is Affected: The service is paid at 25% of the fee.
Modifier: 56 Definition: Preoperative management only
How Payment Is Affected: The service is paid at 25% of the fee.
Modifier: 62 Definition: Two surgeons
How Payment Is Affected: Each surgeon is paid at 62.5% of the fee.
Modifier: 80 Definition: Assistant surgeon
How Payment Is Affected: The service is paid at 16% of the fee.
Modifier: 81 Definition: Minimum assistant surgeon
How Payment Is Affected: The service is paid at 16% of the fee.
Modifier: 82 Definition: Assistant surgeon; qualified resident surgeon not available
How Payment Is Affected: The service is paid at 16% of the fee.
Modifier: 90 Definition: Reference laboratory
How Payment Is Affected: Modifier not allowed.
Modifier: AD Definition: Medical supervision of more than four concurrent anesthesia procedures
How Payment Is Affected: Each service is paid at 52.5% of the fee.
Modifier: AS Definition: Physician assistant, nurse practitioner or clinical nurse specialist as assistant at surgery
How Payment Is Affected: The service is paid at 16% of the fee.
Modifier: QK Definition: Medical supervision of 2--4 concurrent anesthesia procedures
How Payment Is Affected: Each service is paid at 52.5% of the fee.
Modifier: QX Definition: Certified registered nurse anesthetist service: medically directed by medical doctor.
How Payment Is Affected: Each service is paid at 52.5% of the fee.
Modifier: QZ Definition: Certified registered nurse anesthetist service without medical direction
How Payment Is Affected: The modifier does not reduce the fee, but a professional differential of 90% is applied due to provider type. See Professional Differentials below.
Modifier: TC Definition: Technical component
How Payment Is Affected: For services paid via the RBRVS fee schedule, see the specific service. For other services, payment equals 60% of the fee.
Modifier: U4 Definition: For Lenses only, due to change in RX
How Payment Is Affected: The modifier will allow a fitting procedure to be reimbursed if performed sooner than the allowed time frame.
Professional Differentials
For some services within the scope of RBRVS payment methods, mid-level practitioners are paid differently; however, optometrists, ophthalmologists, and opticians are always paid at 100% of the fee schedule.
Bundled Codes
A few services are covered by the Department but have a fee of zero, meaning that payment for the service is considered bundled into the payment for services that are usually provided with it. Examples are temporary tear duct plug, permanent tear duct plug, and special spectacles fitting. Because these services are covered by Montana Healthcare Programs , providers may not bill members for them on a private pay basis.
Status Codes
The RBRVS fee schedule includes status codes that show how each service is paid. The list of status codes is based on that used by Medicare, as shown in the table on the next page.
Medicare and Montana Healthcare Programs RBRVS Status Values
Medicare Status: A - Active code paid using RVUs
Montana Healthcare Programs Status: A - Active code paid using RVUs set by Medicare
Medicare Status: B - Bundled code
Montana Healthcare Programs Status: B - Bundled code
Medicare Status: C - Carrier determines coverage and payment
Montana Healthcare Programs Status: C - Pay by report
Medicare Status: D - Deleted code
Montana Healthcare Programs Status: D - Discontinued code
Medicare Status: E - Excluded from fee schedule by regulation
Montana Healthcare Programs Status: - [Montana Healthcare Programs reviews each code and usually assigns A, K, or X status]
Medicare Status: F - Deleted/discontinued code; no grace period
Montana Healthcare Programs Status: D - [Assigned to D status]
Medicare Status: G - Use another code; grace period allowed
Montana Healthcare Programs Status: G - Use another code; grace period set code-by-code
Medicare Status: H - Modifier deleted
Montana Healthcare Programs Status: - [Assigned to D status]
Medicare Status: I - Use another code; no grace period
Montana Healthcare Programs Status: - [Assigned to G status]
Montana Healthcare Programs Status: J - Anesthesia code
Montana Healthcare Programs Status: K - Active code paid using RVUs set by Montana Healthcare Programs
Montana Healthcare Programs Status: L - Not paid via RBRVS. See lab fee schedule.
Montana Healthcare Programs Status: M - Not paid via RBRVS. See non-RBRVS fee schedule.
Medicare Status: N - Excluded from fee schedule by policy
Montana Healthcare Programs Status: - [Montana Healthcare Programs reviews each code and usually assigns A, K, or X status]
Medicare Status: P - Bundled or excluded
Montana Healthcare Programs Status: - [Montana Healthcare Programs reviews each code and usually assigns B or X status]
Medicare Status: R - Restricted coverage
Montana Healthcare Programs Status: - [Montana Healthcare Programs reviews each code and usually assigns A or K status]
Medicare Status: T - Injections
Montana Healthcare Programs Status: - [Montana Healthcare Programs reviews each code and usually assigns A status]
Medicare Status: X - Excluded from fee schedule by statute
Montana Healthcare Programs Status: X - Not covered
Medicare publishes RVUs for codes that have Medicare status values of R and sometimes publishes RVUs for codes with status values of E, N, or X. Medicare uses the label “injections” for status T but now uses the code for other situations (e.g., pulse oximetry) where Medicare pays for the service only if no other service is performed on the same day.
Payment for Eyeglasses
Payment for eyeglasses is through a single volume purchase contract issued by the Department through the competitive Request for Proposal (RFP) process.
How Cost Sharing Is Calculated on Montana Healthcare Programs Claims
Member cost sharing fees are a set dollar amount per visit based on the average Montana Healthcare Programs allowed amount for the provider type and rounded to the nearest dollar. There is no cost sharing cap. The member’s cost sharing amount is shown on the remittance advice and deducted from the Montana Healthcare Programs allowed amount. See the Billing Procedures and Remittance Advices and Adjustments chapters.
How Payment Is Calculated on TPL Claims
When a member has coverage from both Montana Healthcare Programs and another insurance company, the other insurance company is often referred to as third party liability (TPL). In these cases, the other insurance is the primary payer (as described in the Coordination of Benefits chapter of this manual), and Montana Healthcare Programs makes a payment as the secondary payer.
How Payment Is Calculated on Medicare Crossover Claims
When a member has coverage from both Montana Healthcare Programs and Medicare, Medicare is the primary payer as described in the Coordination of Benefits chapter of this manual. Montana Healthcare Programs then makes a payment as the secondary payer. For the provider types covered in this manual, Montana Healthcare Programs ’s payment is calculated so that the total payment to the provider is either the Montana Healthcare Programs allowed amount less the Medicare paid amount or the sum of the Medicare coinsurance and deductible, whichever is lower. This method is sometimes called lower of pricing.
Other Programs
The payment method described in this chapter applies to eyeglass services for Healthy Montana Kids (HMK). This chapter does not apply to HMK optometric services, which are covered by Blue Cross and Blue Shield of Montana. For more information on HMK, visit the HMK website.
End of How Payment is Calculated Chapter
Appendix A: Forms
- Eyeglass Additional Feature and Contact Lens Prior Authorization Request
- Montana Individual Adjustment Request
- Paperwork Attachment Cover Sheet
End of Appendix A: Forms Chapter
Appendix B: Place of Service Codes
Place of Service Codes are two-digit codes placed on healthcare professional claims to indicate the setting in which a service was provided.
The Centers for Medicare and Medicaid CMS) maintain POS codes used throughout the healthcare industry.
Refer to http://cms.hhs.gov/Medicare/Coding/place-of-service-codes/index.html.
End of Appendix B: Place of Service Codes Chapter
Definitions and Acronyms
End of Definitions and Acronyms Chapter
Search Options
Previous editions of this manual contained an index.
This edition has three search options.
1. Search the whole manual. Open the Complete Manual pane. From your keyboard press the Ctrl and F keys at the same time. A search box will appear. Type in a descriptive or key word (for example "Denials". The search box will show all locations where denials discussed in the manual.
2. Search by Chapter. Open any Chapter tab (for example the "Billing Procedures" tab). From your keyboard press the Ctrl and F keys at the same time. A search box will appear. Type in a descriptive or key word (for example "Denials". The search box will show where denials discussed in just that chapter.
3. Site Search. Search the manual as well as other documents related to a particular search term on the Montana Healthcare Programs Site Specific Search page.